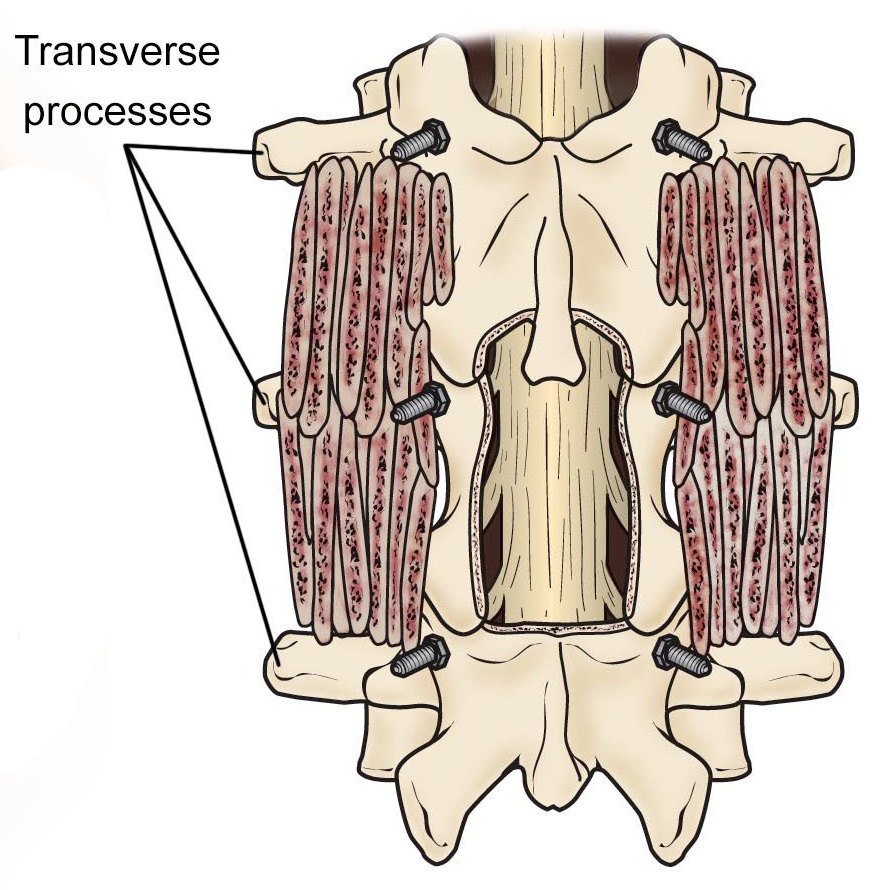
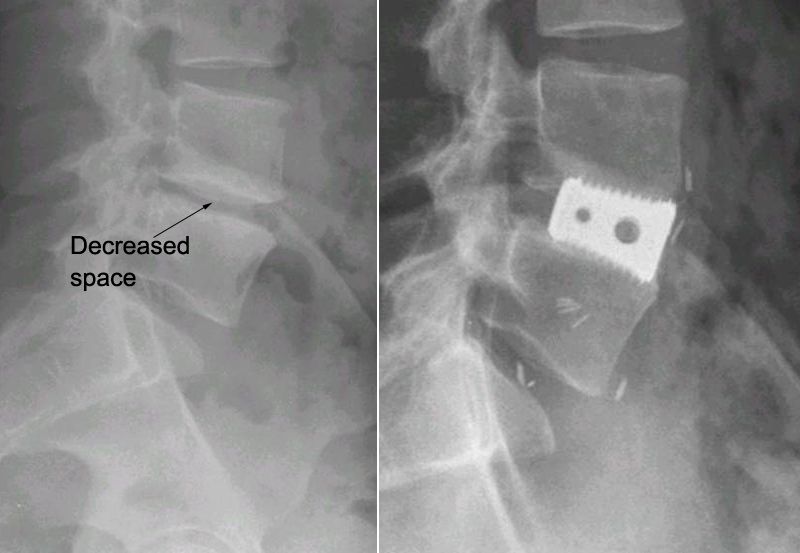
Treatment
Spinal Fusion
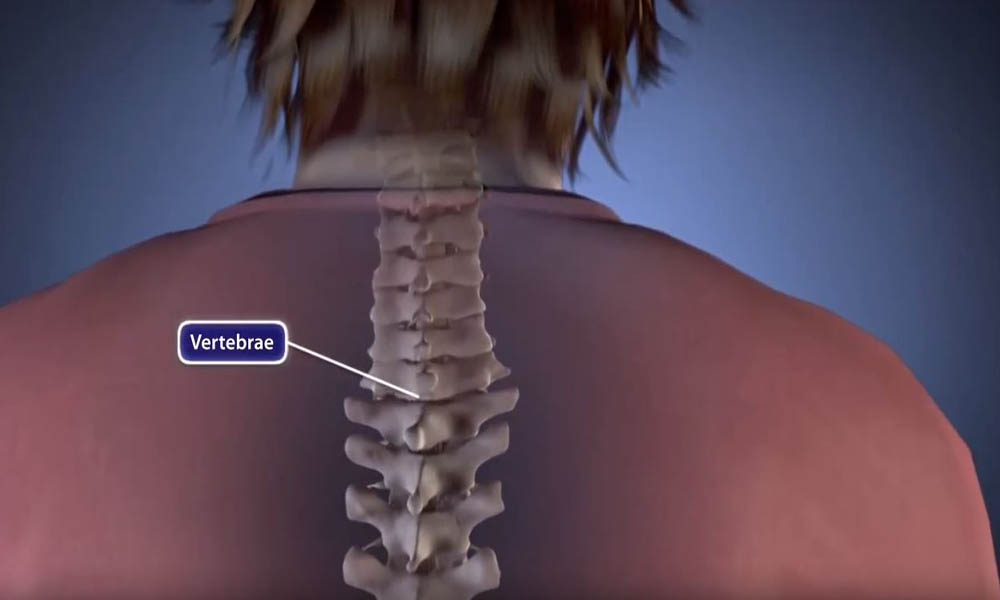
Spinal fusion is a surgical procedure used to correct problems with the small bones in the spine (vertebrae). It is essentially a welding process. The basic idea is to fuse together two or more vertebrae so that they heal into a single, solid bone. This is done to eliminate painful motion or to restore stability to the spine.
Spine surgery is usually recommended only when your doctor can pinpoint the source of your pain. To do this, your doctor may use imaging tests, such as X-rays, computed tomography (CT) scans, and magnetic resonance imaging (MRI) scans.
Spinal fusion may help relieve symptoms of many back problems, including:
- Degenerative disk disease
- Spondylolisthesis
- Spinal stenosis
- Scoliosis
- Fractured vertebra
- Infection
- Herniated disk
- Tumor
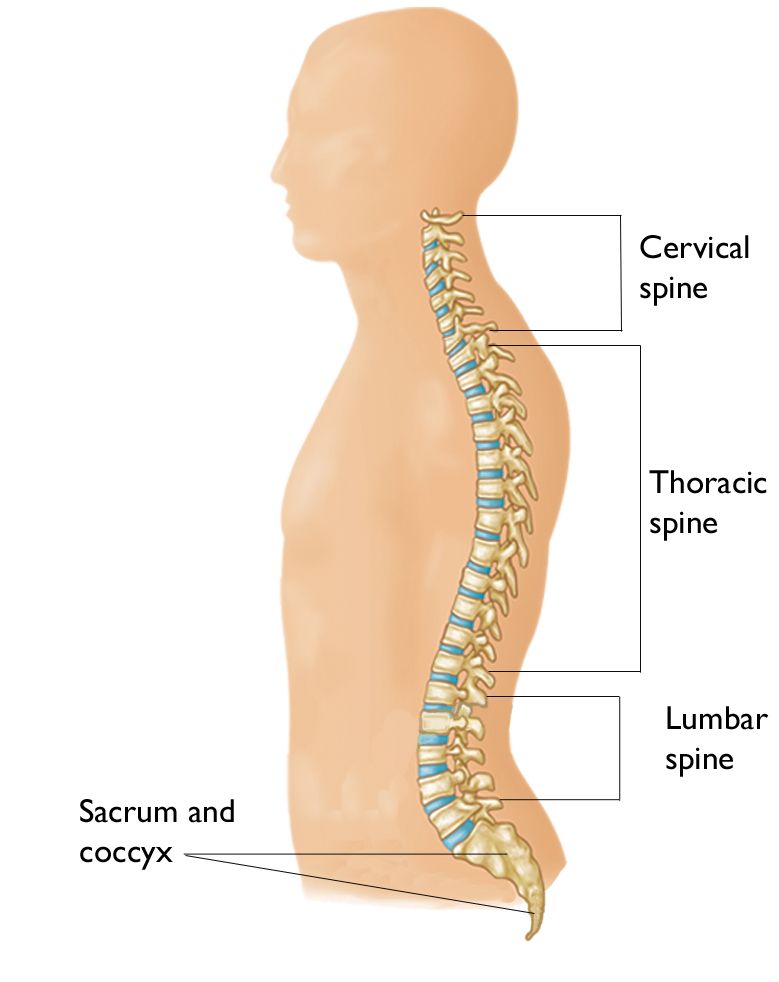
Understanding how your spine works will help you better understand spinal fusion. Learn more about your spine: Spine Basics.
Description
Spinal fusion eliminates motion between vertebrae. It also prevents the stretching of nerves and surrounding ligaments and muscles. It is an option when motion is the source of pain, such as movement that occurs in a part of the spine that is arthritic or unstable due to injury, disease, or the normal aging process. The theory is if the painful vertebrae do not move, they should not hurt.
If you have leg pain or arm pain in addition to back pain, your surgeon may also perform a decompression (laminectomy). This procedure involves removing bone and diseased tissues that are putting pressure on spinal nerves.
Fusion will take away some spinal flexibility, but most spinal fusions involve only small segments of the spine and do not limit motion very much. The majority of patients will not notice a decrease in range of motion. Your surgeon will talk with you about whether your specific procedure may impact flexibility or range of motion in your spine.
Procedure
Lumbar and cervical spinal fusion have been performed for decades. There are several different techniques that may be used to fuse the spine. There are also different "approaches" your surgeon can take to reach your spine.
Your surgeon may approach your spine from the front. This is called an anterior approach and requires an incision in the lower abdomen for a lumbar fusion or in the front of the neck for a cervical fusion. (Related Article: Anterior Lumbar Interbody Fusion)
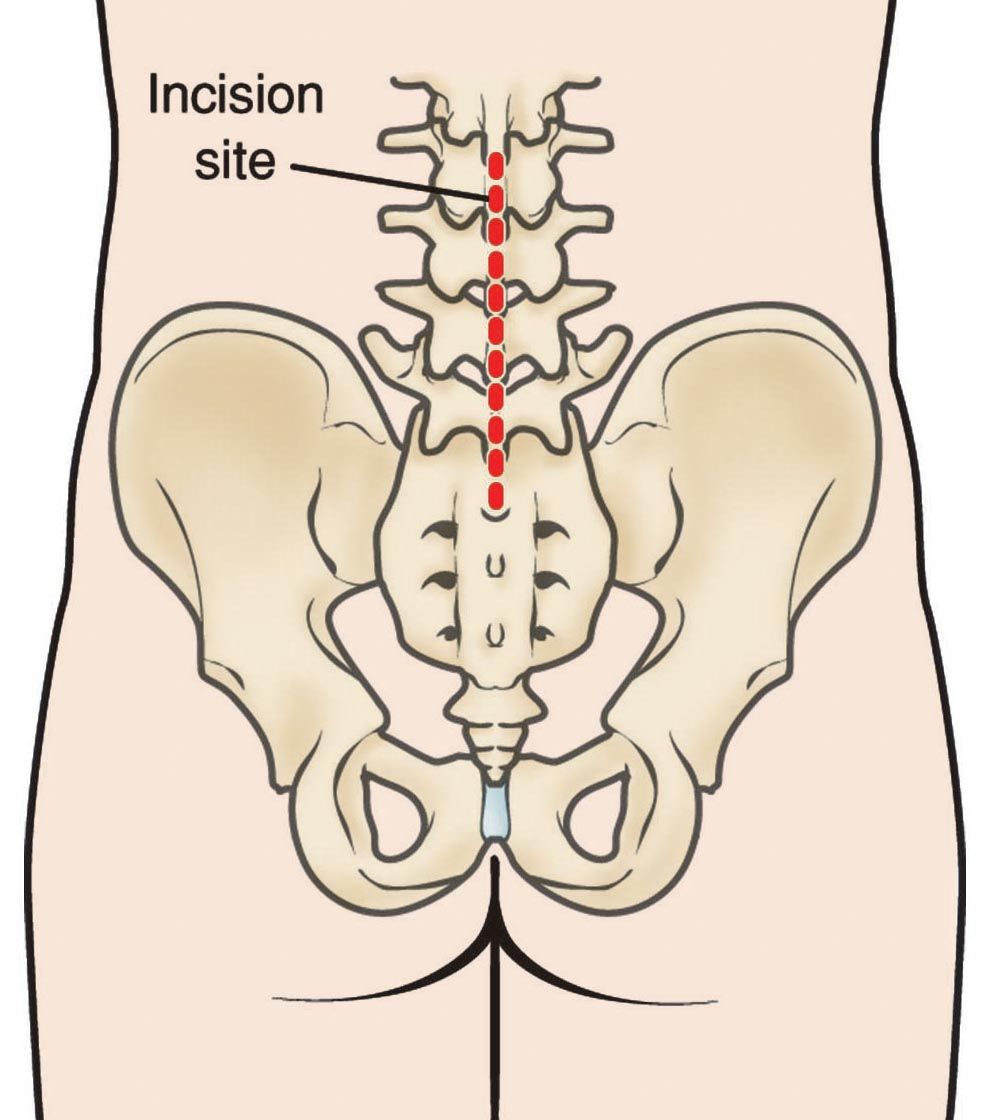
A posterior approach is done from the back. (Related Articles: Posterolateral Lumbar Fusion and Posterior Lumbar Interbody Fusion and Transforaminal Lumbar Interbody Fusion)
In a lateral approach, your surgeon approaches your spine from the side. (Related Article: Lateral Lumbar Interbody Fusion)
Minimally invasive techniques have also been developed. These allow fusions to be performed with smaller incisions.
The right procedure for you will depend on the nature and location of your disease.
Watch: Spinal Fusion Animation
Bone Grafting
All spinal fusions use some type of bone material, called a bone graft, to help promote the fusion. Generally, small pieces of bone are placed into the space between the vertebrae to be fused.
A bone graft is primarily used to stimulate bone healing. It increases bone production and helps the vertebrae heal together into a solid bone. Sometimes larger, solid pieces are used to provide immediate structural support to the vertebrae.
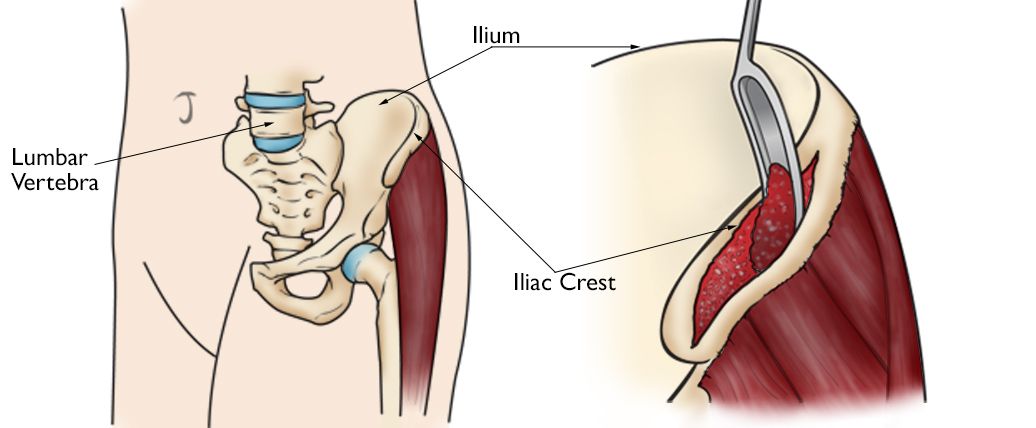
In the past, a bone graft harvested from the patient's pelvis was the only option for increasing the material needed for fusing the vertebrae. This type of graft is called an autograft. Harvesting a bone graft requires an additional incision during the operation. It lengthens surgery and can cause increased pain after the operation.
If you are having a decompression procedure, the surgeon may harvest your bone from the site of the decompression and use it as the graft. This type of graft is called a local autograft. The bone is essentially recycled; it is moved from where it is compressing your nerves to the area the surgeon wants to fuse.
One alternative to harvesting a bone graft is an allograft, which is cadaver bone. An allograft is typically acquired through a bone bank. These tissues are highly processed, and the chance of infection or disease from this tissue is very low.
Today, several artificial bone graft materials have also been developed:
- Demineralized bone matrices (DBMs). Calcium is removed from cadaver bone to create DBMs. Without the mineral, the bone can be changed into a putty or gel-like consistency. DBMs are usually combined with other grafts and may contain proteins that help in bone healing.
- Bone morphogenetic proteins (BMPs). These very powerful synthetic bone-forming proteins promote a solid fusion. They are approved by the U.S. Food and Drug Administration for use in the spine in certain situations. Autografts may not be needed when BMPs are used.
- Synthetic bone. Synthetic bone grafts are made from calcium/phosphate materials and are often called “ceramics.” They are similar in shape and consistency to autograft bone.
Your surgeon will discuss with you the type of bone graft material that will work best for your condition and procedure.
Immobilization
After bone grafting, the vertebrae need to be held together to help the fusion progress.
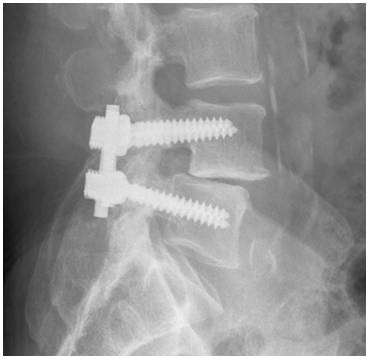
In many cases, surgeons will use plates, screws, and rods to help hold the spine still. This is called internal fixation, and it may increase the rate of successful healing. With the added stability from internal fixation, most patients are able to move earlier after surgery. Your surgeon may suggest that you wear a brace to help protect the welding process.
Complications
As with any surgery, there are risks associated with spinal fusion. Your doctor will discuss each of the risks with you before your procedure and will take specific measures to help avoid potential complications. Potential risks and complication of spinal fusion include:
- Infection. Antibiotics are regularly given to the patient before, during, and often after surgery to lessen the risk of infections.
- Bleeding. A certain amount of bleeding is expected, but this is not typically significant. It is not usually necessary to donate blood before spinal fusion.
- Pain at graft site. A small percentage of patients will experience persistent pain at the bone graft site.
- Recurring symptoms. Some patients may experience a recurrence of their original symptoms. There are various causes for this. If your original symptoms recur, inform your doctor so that he or she can determine what is causing your symptoms.
- Pseudarthrosis. This is a condition in which there is not enough bone formation to create a solid fusion. Patients who smoke are more likely to develop a pseudarthrosis. Other causes include diabetes and older age. Moving too soon — before the bone is able to start fusing — may also result in a pseudarthrosis. If this occurs, a second surgery may be needed.
- Nerve damage. It is possible that nerves or blood vessels may be injured during these operations. These complications are very rare.
- Blood clots. Another uncommon complication is the formation of blood clots in the legs. These pose significant danger if they break off and travel to the lungs.
Warning Signs
It is important that you carefully follow any instructions from your doctor relating to the warning signs of blood clots and infection. These complications are most likely to occur during the first few weeks after surgery.
Blood clots. Warning signs of a possible blood clot include:
- Swelling in the calf, ankle, or foot
- Tenderness or redness, which may extend above or below the knee
- Pain in the calf
Occasionally, a blood clot will travel through the bloodstream and may settle in the lungs. If this happens, you may experience sudden chest pain and shortness of breath or coughing. If you experience any of these symptoms, you should notify your doctor immediately. If you cannot reach your doctor, have someone take you to the hospital emergency room or call 911.
Infection. Infection following spine surgery occurs very rarely. Warning signs of infection include:
- Redness, tenderness, and swelling around the wound edges
- Persistent drainage from the wound
- Pain or tenderness
- Shaking chills
- Elevated temperature, usually above 101°F if taken with an oral thermometer
If any of these symptoms occur, you should contact your doctor or go to the nearest emergency room immediately.
Recovery
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor and nurses will work to reduce your pain, which can help you recover from surgery faster.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Opioids can provide excellent pain relief; however, their use has risks and complications. These medications can be addictive and potentially dangerous. It is therefore important to use opioids only as directed by your doctor, to use as little as possible for as short a time as possible, and to stop taking them as soon as your pain starts to improve. Tell your doctor if your pain has not begun to improve within a few days after surgery.
If you are already taking narcotics prior to surgery, talk to your surgeon before your procedure so you can plan your postoperative pain regimen together.
Rehabilitation
The fusion process takes time. It may be several months before the bone is solid, although your comfort level will often improve much faster. During this healing time, the fused spine must be kept in proper alignment. You will be taught how to move properly, reposition, sit, stand, and walk.
Your symptoms will gradually improve, as will your activity level. Right after your operation, your doctor may recommend only light activity, like walking. As you regain strength, you will be able to slowly increase your activity level. Physical therapy is typically started 6 weeks to 3 months after surgery. Your surgeon will talk with you about whether physical therapy is needed in your situation.
Maintaining a healthy lifestyle and following your doctor's instructions will greatly increase your chances for a successful outcome.
Research
Recent research has focused on developing new bone graft materials that may act as safe and effective substitutes for a patient's own tissue.
In addition, total disk replacements and other motion-sparing techniques have recently been proposed as alternatives to spinal fusion for the treatment of spinal disorders.
Biological products are also being developed to help stop disk degeneration before it leads to nerve compression.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.