Diseases & Conditions
Medial Epicondylitis (Golfer's Elbow)
This article was written and/or reviewed by a member of American Shoulder and Elbow Surgeons (ASES).
Medial epicondylitis is a painful condition of the elbow that can be caused by overuse or through overexertion.
While it commonly affects golfers — which is why it was coined "Golfer's elbow" — many different types of activities can cause the condition, including overhead throwing, tennis, and weightlifting. Medial epicondylitis can also develop in non-athletes or without a specific injury.
With overuse, meaning repeating the same motions again and again, or with overexertion, the tendons of the forearm muscles that attach to the inside of the elbow can partially tear and wear down over time, which leads to pain.
Medial epicondylitis can usually be treated successfully without surgery. In patients who do not see improvement after several months of appropriate nonsurgical treatment, surgery may be considered.
Anatomy
The elbow joint is made up of three bones:
- The humerus (the upper arm bone)
- The radius (the outer bone in the forearm)
- The ulna (the inner bone in the forearm)
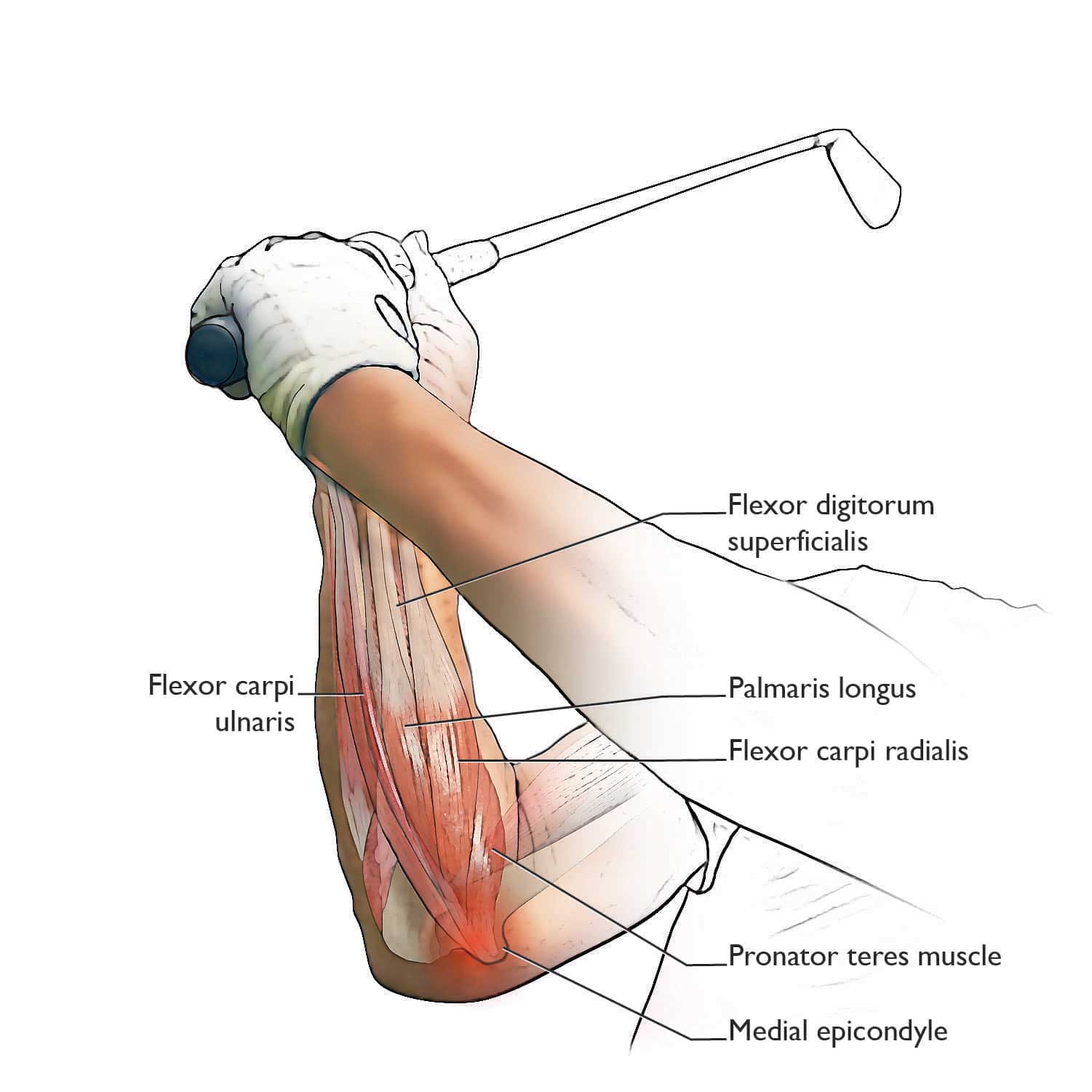
Many of the muscles that allow you to rotate your forearm inward (pronation) and flex (bend) your wrist and fingers are attached by tendons to the end of the humerus on the inside of the elbow joint. The tendons — strong, flexible cords of tissue — attach at a prominent portion of the bone you can feel, called the medial epicondyle.
One of these muscles, the pronator teres, is the muscle that is most often injured in medial epicondylitis, although all of these muscles can be involved.
- The pronator teres tendon, which attaches the pronator teres muscle to the medial epicondyle, is one of several tendons that may be involved when you have medial epicondylitis.
- Others include the flexor carpi radialis, palmaris longus, flexor digitorum superficialis, and flexor carpi ulnaris.
The ulnar nerve, which passes just behind the medical epicondyle (and is what causes symptoms when you strike your "funny bone"), can also sometimes be irritated where it enters the forearm muscles.
Cause
Repetitive motions of these muscles lead to tendon injuries in the place where the tendon attaches to the medial epicondyle. Over time, this leads to the tendon wearing down, such as fraying or tearing.
These types of motions are common with sporting activities, such as golf, but can occur without any recognized injury. Improper swing technique or improper equipment may be risk factors in people who develop the condition with sporting activities.
Age also plays a role in development of the condition, which usually occurs in adults between the ages of 40 and 60. Medial epicondylitis may also occur with repetitive activities of daily living, like doing certain household chores.
Symptoms
Symptoms of medial epicondylitis often develop gradually, typically growing worse over weeks to months.
Common symptoms include:
- Pain or burning in the inner part of the elbow, with occasional shooting pain down toward the hand
- Weak grip strength
- Decreased wrist and/or elbow range of motion, typically due to pain
Occasionally, people with medial epicondylitis will develop irritation of the nearby ulnar nerve, due to inflammation where the ulnar nerve enters the forearm muscles. This condition is called ulnar neuritis, and the main symptom is pain. Some patients may also develop numbness and tingling in their ring and pinky fingers.
More about this condition can be found in the article Ulnar Nerve Entrapment at the Elbow (Cubital Tunnel Syndrome).
Doctor Examination
Medical History and Physical Examination
Your doctor will typically begin by asking you questions about your symptoms:
- Was there a specific injury?
- What kinds of activities cause the pain?
- How long the pain has been there?
Your doctor may then perform a physical examination:
- Palpation. Your doctor may palpate (push on) the various bony prominences of your elbow to determine where the pain is coming from.
- Strength testing. Your doctor may have you perform various wrist, forearm, or elbow motions while the doctor applies resistance.
- Testing of the ulnar nerve. Your doctor may perform a special test called a Tinel test by tapping on the "funny bone" nerve to see if it is irritated, as well as testing the strength and sensation (feeling) in your hand.
Imaging Tests
Your doctor may order some imaging tests to help make the diagnosis.
- X-rays. An X-ray is commonly ordered. X-rays do not show the tendons and muscles but are important to make sure you do not have a fracture or arthritis in the elbow.
- Ultrasound or magnetic resonance imaging (MRI). Doctors sometimes order an ultrasound or MRI to help confirm and assess the how serious the tendon injury is. MRI may also be used to rule out other conditions that can have similar symptoms, such as an ulnar collateral ligament (UCL) injury. However, these tests are typically not ordered unless the symptoms have been going on for a long time and are not responding to nonsurgical treatment.
- Electromyography (EMG) studies are sometimes ordered to rule out nerve compression, particularly when patients have symptoms of ulnar nerve irritation.
Treatment
Various treatments can be used to treat medial epicondylitis, with the main goals being:
- Relieving the acute pain
- Rehabilitating the injured tendon
- Preventing the condition from coming back
Most cases of medial epicondylitis can be effectively treated without surgery. Surgery is usually considered only for patients:
- Who do not see improvement after several months of nonsurgical treatment
- Who have chronic (long-standing) symptoms
Relieving Acute Pain
Treatment for acute symptoms typically involves:
- Activity modification. Do your best to avoid activities that cause pain.
- Icing. Apply ice to the painful area several times a day for 20 minutes at a time. Do not apply ice directly to the skin; use an ice pack or wrap the ice in a towel.
- Medications. Take a short course of nonsteroidal anti-inflammatory medications (NSAIDs) if you can tolerate them. Some people have medical conditions (e.g., kidney disease) or take other medications that make it dangerous to take NSAIDs.
- Bracing. Your doctor may recommend a counterforce brace or a wrist brace (cock-up). The counterforce brace is used to limit the amount of force that is placed through the injured tendons. This may occasionally cause more forearm pain. A wrist brace is used to rest the muscles and tendons that are affected.
- Injections. Steroid injections to the injured tendons may sometimes be considered. While these injections provide initial relief, some research suggests that they may lengthen the rehabilitation process and lead to worsening damage of the tendons. If you are considering a corticosteroid injection, discuss the risks and benefits with your physician so you can make an informed decision.
Rehabilitation and Prevention
Once the acute pain has improved, there are many different treatments that have been shown to help rehabilitate the injured tendon and keep the condition from coming back.
Stretching and Strengthening
Exercises have long been the main treatment for medial epicondylitis.
- Early on, stretching to regain full, pain-free movement of the wrist is the goal.
- Once that is achieved, you begin strengthening exercises, focusing on wrist flexion (bending the elbow) and pronation (a movement that turns your hand so your palm faces downward).
- Eccentric strengthening exercises are thought to be particularly beneficial. An eccentric exercise is when a load is applied to a muscle while it lengthens. You can see examples of eccentric strengthening exercises here: Therapeutic Exercise Program for Epicondylitis (Tennis Elbow/Golfer's Elbow).
Other Nonsurgical Treatments
Several other potential treatments have shown — through research — that they may be beneficial. These include:
- Platelet-rich plasma (PRP) injections
- Dry needling
- Extracorporeal shock wave therapy (EWST)
These treatments are used to help trigger the body's natural healing responses, although it is not yet known how effective they are compared to typical stretching and strengthening programs. You may want to discuss these options with your physician if your symptoms are severe or have not been improving with a stretching and strengthening program.
Surgical Treatment
Surgery for medial epicondylitis is typically only considered for patients whose symptoms fail to improve after trying recommended nonoperative treatments for at least several months.
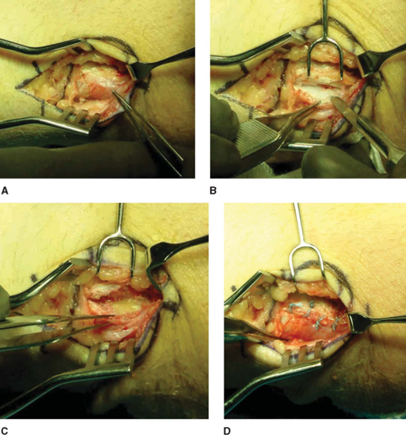
Surgery involves cutting open the tendons near where they attach to the medial epicondyle and removing the damaged area of the pronator teres tendon — a procedure called debridement.
- When the damaged area of the tendon is relatively small, the tendon can be repaired in a side-to-side manner.
- When there is a larger amount of damage, the surgeon may place anchors in the medial epicondyle to reattach the healthy part of the tendon back to the bone after the debridement.
In patients who also have ulnar nerve symptoms, occasionally ulnar nerve decompression or transposition is also performed during the same procedure. See the article Ulnar Nerve Entrapment at the Elbow (Cubital Tunnel Syndrome) for more information on these procedures.
Post-Surgical Care
Typically, patients will be placed in a splint and/or sling to immobilize the arm (hold it still) for 1 to 2 weeks after surgery. Whether a splint or sling is needed and for how long depends on how much debridement was necessary at the time of surgery. If you have surgery, your surgeon will provide you with specific instructions after the procedure.
After a period of immobilization and rest, patients are typically allowed to resume normal range of motion, likely with some restrictions on activities.
- Strengthening exercises typically start 6 to 8 weeks after surgery.
- You can usually resume normal activities and sports 3 to 6 months after surgery.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.