Treatment
Revision Total Shoulder Replacement
This article was written and/or reviewed by a member of American Shoulder and Elbow Surgeons (ASES).
Shoulder arthroplasty (replacement) has been used to treat a variety of shoulder conditions for more than 30 years.
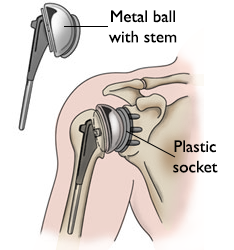
The shoulder is a ball-and-socket joint: The head of the humerus (arm bone) fits into a shallow socket in the shoulder blade called the glenoid. In a shoulder replacement, one or both portions of the bones and articular cartilage (the smooth substance within the joints) is removed and replaced with metal and plastic components (parts).
Unfortunately, not all of these replacements last for a patient's entire lifetime. A shoulder replacement can fail for a variety of reasons, including infection, pain, loosening, or instability (dislocations) of the components. Whatever the cause, the patient may lose shoulder function, develop pain, or both.
When a shoulder replacement fails, it needs to be removed and revised (re-done). Revising (re-doing) a problematic shoulder replacement is a significant undertaking. This article will help you better understand the procedure and what happens after surgery.
Description
The glenohumeral joint (ball-and-socket between the arm and shoulder blade) can be replaced with metal or plastic on one or both surfaces of the joint. These procedures are typically done through an open incision, not arthroscopically. Muscles surrounding the shoulder are typically retracted (moved out of the way) and repaired as necessary during the operation.
A total shoulder replacement involves both the humerus (arm bone) and glenoid (socket.)
The implants are placed with precise tools and instruments during surgery. During revision surgery, your surgeon uses the bone, muscles, and soft tissues around the replacement to determine the best type and method for the new replacement. The large muscles around the shoulder (deltoid, pectoralis major) are very important to motion, and surgeons carefully place the implants around these muscles to avoid damaging them.
Symptoms
Pain after a shoulder replacement is the most common symptom that patients experience. It is common for patients to develop pain after having the shoulder replacement for many years; however, some patients have pain sooner after surgery.
Discuss any changes in pain or function after your shoulder replacement with your surgeon.
Similarly, some patients have a loss in function or use of the shoulder. Limited range of motion, instability (shoulder replacement popping in and out), or loss of strength may affect function in the arm. Patients may also experience mechanical symptoms like grinding, catching, or shifting after the replacement had the joint moving smoothly and normally again.
Doctor Examination
Medical History
Your surgical team will typically begin by asking specific questions about the timing and location of your previous replacement. If you have this information, it can be very helpful in determining which type of shoulder replacement you have, as there are many different types of replacements. Any operative reports (the notes from your prior surgery) can also be very helpful. If you do not have this information, do not worry; you can still be treated.
Physical Examination
During the physical exam, your surgeon will evaluate your incision (scar) and check for muscle and nerve function. Pain is one of the most common signs that a shoulder replacement that may require revision.
Some of the movements or tests may be uncomfortable or painful; however, they are necessary because they provide your surgeon with information about which parts of the shoulder or implants are causing problems. Your surgeon will also test for strength by taking you through a variety of movements.
Imaging Tests
Your doctor will also require imaging, such as X-rays, ultrasound, a magnetic resonance imaging (MRI) scan, and/or a computed tomography (CT) scan to evaluate the bone, muscles/tendons, and implants. This imaging will help your surgeon determine the cause of your symptoms and potential options to redo your shoulder replacement and improve your pain and function.
Treatment
Nonsurgical Treatment
Occasionally, the cause of your shoulder symptoms is a minor issue that may be easily addressed with simple measures such as rest, physical therapy, and, in rare cases, corticosteroid or platelet-rich plasma (PRP) injections.
You may also not be a good candidate for surgery. For instance, if you have a significant health condition, complex revision surgery may be too risky for you.
Surgical Treatment
If the exam reveals a concern about the implant and you are generally healthy, your surgeon may recommend revision surgery. These are some of the specific issues that may lead your surgeon to suggest a revision:
Infection (bacteria on or around the implant). Bacteria that lives underneath your skin may stick to the components (parts) of the implant. While surgical teams take a lot of precautions to avoid this, it may still affect a small number of patients. If your team suspects an infection, they will typically order additional tests and imaging to help determine if revision surgery is necessary for infection.
Fractures. Fractures (breaks in the bone around a shoulder replacement) may also occur. Not all fractures around a shoulder replacement require another operation or revision surgery. If the implant is damaged or loose as a result of the broken bone, or if the broken bone cannot heal because of the implant, you may need revision surgery.
Revision Procedure
Surgeons specifically try to limit damage to the shoulder — especially the shoulder muscles — during joint replacement surgery. During revision surgery, many of these same muscles need to be moved again, and scarring can occur. Typically, surgeons will use an incision (cut) over the front of the shoulder, although revision surgery may require a longer or different incision.
During revision surgery, parts of the prior shoulder replacement will be removed or changed in some way.
Occasionally, the surgeon will need to use an allograft (bone from a donor) or autograft (bone taken from another part of your body) to help secure the new replacement.
In some cases, depending on how badly damaged the bones around the old implant are, your surgeon may need to order custom or complex implants.
Recovery and Complications
Recovery from a revision surgery can be challenging. Many patients experience some frustration during the recovery phase, as return to previous function can take up to 1 to 2 years, which is longer than the recovery for their first (or primary) shoulder replacement.
You may be prescribed physical therapy to help regain shoulder range of motion and strength. However, it is important to be aware that some patients do not return to full function following a revision surgery.
Risks and complications related to revision surgery are typically greater than for primary (first-time) shoulder replacement surgery. These may include:
- Dislocation (popping out of socket)
- Fracture (breaks in the bone)
- Infection
Some patients may continue to have pain or difficulty using the shoulder, and some will require additional surgery to improve the symptoms related to their shoulder revision. Your surgeon will explain the specific risks of your shoulder surgery.
Outcomes
Outcomes after revision shoulder replacement vary widely between patients and depend on many different factors. Your surgical team will help you set a realistic expectation based on the revision surgery you need. Often, results of revision surgery are not quite as good as the results of the original shoulder replacement surgery.
Summary
Revision shoulder replacement surgery is an uncommon and challenging surgical procedure. Pain and loss of function are the most common symptoms that can indicate a problem with the implant. Patients should be prepared for a prolonged recovery and should carefully weigh the risks and benefits of revision with their surgeon.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.