Treatment
Cervical Spondylotic Myelopathy: Surgical Treatment Options
This article provides information on surgery for cervical spondylotic myelopathy. For more general information: Cervical Spondylotic Myelopathy (Spinal Cord Compression)
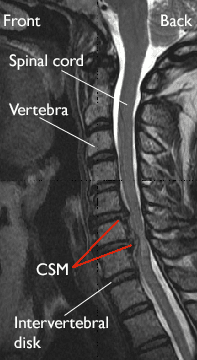
When symptoms of cervical spondylotic myelopathy (CSM) continue or worsen despite nonsurgical treatment, your doctor may recommend surgery.
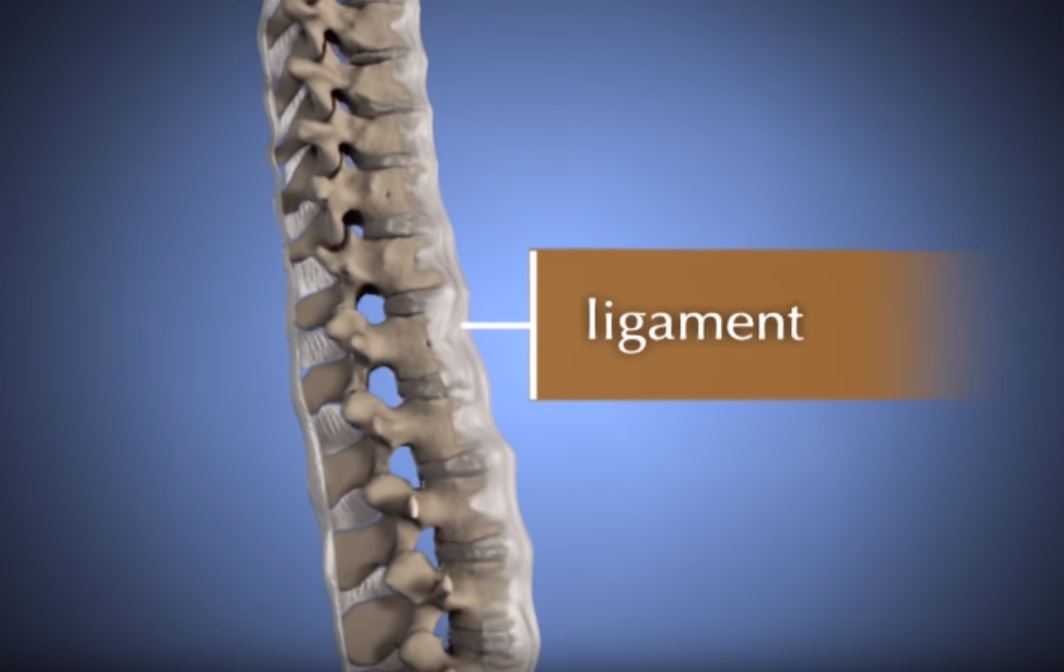
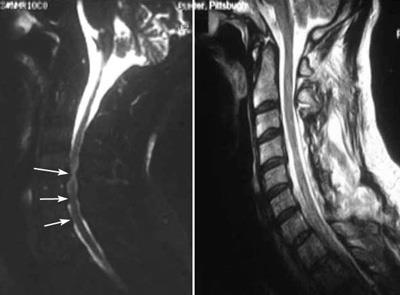
The goal of surgery is to relieve symptoms by decompressing, or relieving pressure on the spinal cord. This involves removing the pieces of bone or soft tissue (such as a herniated disk or thickened ligament) that may be taking up space in the spinal canal. This relieves pressure by creating more space for the spinal cord.
Candidates for Cervical Spondylotic Myelopathy Surgery
Candidates for surgery include patients who have worsening neurological changes with signs of severe spinal cord compression or spinal cord swelling. These neurological changes may include:
- Weakness in the arms or legs.
- Numbness in the hands.
- Loss of dexterity (fine motor skills) in your hands; you may have trouble with tasks that require precise control over hand movements, such as handwriting, buttoning your clothing, or feeding yourself.
- Imbalance and other coordination problems. You may have trouble walking, or you may fall down. With myelopathy, there is no sensation of spinning, or vertigo. Rather, your head and eyes feel unsteady, but your body feels unable to follow through with what you are trying to do.
- Changes in how you walk.
Patients with severe or disabling pain may also be helped with surgery.
Patients who experience better outcomes from cervical spine surgery often:
- Are younger
- Have had symptoms for a shorter amount of time
- Have only one area of the spinal cord involved
- Have more space available within the spinal canal for the spinal cord
Surgical Procedures for Cervical Spondylotic Myelopathy
The are the surgical procedures commonly performed to treat CSM:
- Anterior cervical diskectomy and fusion
- Anterior cervical corpectomy and fusion
- Anterior cervical diskectomy and disk replacement
- Laminectomy and fusion
- Laminoplasty
The procedure your surgeon may recommend will depend on several factors, including your overall health and the type and location of your problem. Studies have not shown one approach to be better than another. Surgery should be individualized.
Depending on the procedure, surgery for CSM is performed from either the front of the neck (anterior) or the back (posterior). In some cases, both anterior and posterior approaches may be needed to address spinal cord compression and instability.
Each approach has advantages and disadvantages, as shown in the table below. Your doctor will talk to you about the risks and benefits of surgery and which approach is best for you.
Spinal Fusion
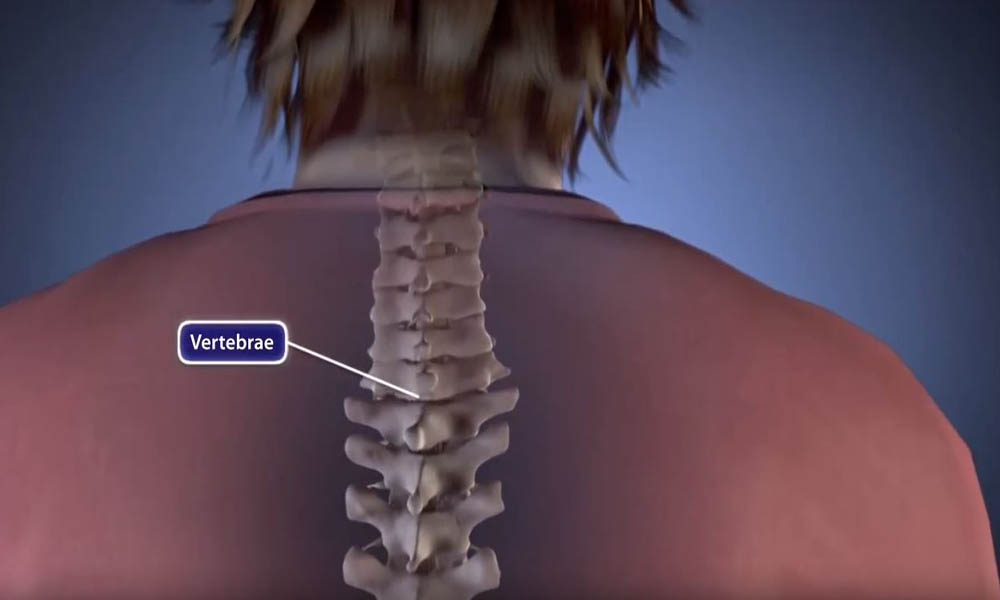
Whether an anterior or posterior approach is used, procedures for CSM often include spinal fusion to help stabilize the spine. Spinal fusion is essentially a welding process. The basic idea is to fuse together the vertebrae so that they heal into a single, solid bone.
Degeneration, or wearing out, of the spine can lead to parts of vertebrae grinding against each other — something that does not happen normally. This grinding can lead to pain. By fusing painful segments together, your surgeon tries to stop this grinding and improve pain. Since fusion eliminates motion between the degenerated vertebrae, it takes away some spinal flexibility. How much flexibility you lose depends on how many spine segments, or levels, of your spine are fused.
To help fusion occur, your surgeon may use bone graft, or small pieces of bone. Bone graft is used to fill in the space left after a disk is removed. It is often placed along the sides of the vertebrae to assist the fusion. Larger pieces can also be placed to add immediate structural support. The goal of using the bone graft is to stimulate bone healing. It can increase new bone production and may help the vertebrae heal together into a solid bone.
There are different types of bone graft. The bone graft can come from either your own bone (autograft) or from a donor (allograft).
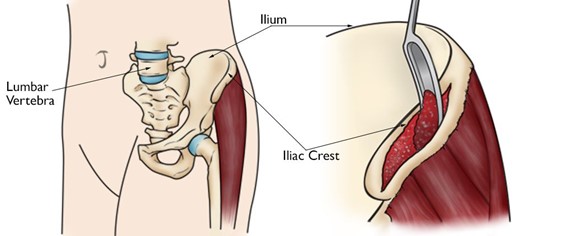
If an autograft is used, the bone is usually harvested (taken) from your hip area. But if only a small amount is needed, your surgeon may be able to use the bone spurs removed from your neck as the autograft. With an autograft, the bone is essentially recycled; it is moved from an area where it is no longer needed to the area that the surgeon wants to fuse.
Your doctor will talk to you about the advantages and disadvantages of using an autograft versus an allograft, as well as potentially using traditional bone grafts versus a cage.
In some cases, the surgeon may implant a spacer or synthetic cage between the two adjoining vertebrae. This cage usually contains bone graft material to allow a spinal fusion to occur between the two vertebrae.
After the bone graft is placed or the cage is inserted, your surgeon will use metal screws, plates, rods, or a combination of these fixation devices to increase the rate of fusion and further stabilize the spine.
Anterior Approach
An anterior approach means that the surgeon will approach your neck from the front. They will operate through a 1- to 2-inch incision along the neck crease. The exact location and length of your incision may vary depending on your specific condition.
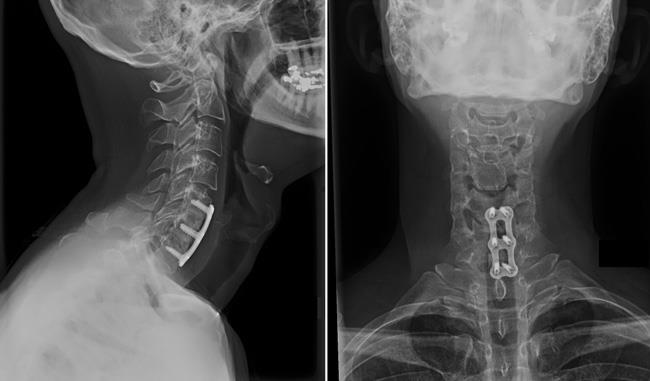
Anterior cervical diskectomy and fusion. During this procedure, your surgeon will remove the problematic disk and any additional bone spurs, if necessary, the surgeon will then stabilize the spine with a spinal fusion. Typically, a plate with screws is added to the front of the spine for added stability.
Anterior cervical corpectomy and fusion. This procedure is similar to diskectomy, except instead of only the disk, one or more of the vertebrae are also removed because the compression is caused by a significant bone spur.
The difference between a corpectomy and diskectomy is the amount of bone removed. As in diskectomy, the spine is then stabilized with a spinal fusion.
In some cases, both the disk and bone may be pressing on the spinal cord. In this situation, your doctor may perform a combination of diskectomy and corpectomy.
Anterior cervical diskectomy and disk replacement. During this procedure, your surgeon will remove the problematic disk and any additional bone spurs, if necessary, just as in the anterior cervical diskectomy and fusion. But instead of placing bone, cages, plates, or screws, the surgeon places an artificial disk.
Unlike fusion, which eliminates motion, disk replacement is designed to preserve motion in the neck. However, not every patient is a candidate for a disk replacement.
Posterior Approach
A posterior approach means that the surgeon will approach your neck from the back. They will make an incision along the midline of the back of the neck. Posterior approaches for decompression include laminectomy and laminoplasty. These procedures, especially laminectomy, are often also accompanied by spinal fusion.
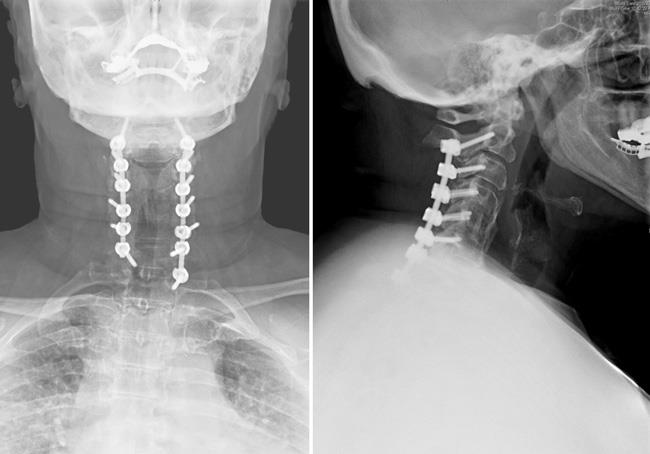
Laminectomy. In this procedure, the surgeon removes the bony arch that forms the backside of the spinal canal (lamina), along with any bone spurs and ligaments that are compressing the spinal cord. Laminectomy relieves pressure on the spinal cord by providing extra space for it to drift backward.
Although laminectomy ensures complete decompression of the spinal cord, the procedure makes the bones less stable. For this reason, patients who have a laminectomy often need spinal fusion with a bone graft and possibly screws and rods.
Posterior laminectomy is often recommended for people who have:
- Very small spinal canals
- Enlarged or swollen soft tissues at the back of the spine
- Problems in more than four spine segments (levels)
In a patient with a kyphotic (bent forward) spine, the spinal cord will not float or shift backward — so the doctor will often use a combined posterior and anterior approach to ensure the best outcome.
Laminoplasty. This procedure is an alternative to laminectomy. Instead of removing the bone, the lamina is thinned out on one side and then cut on the other side to create a hinge — much like a door. Using the hinge to open this bony area expands the space available for the spinal cord. It also allows the surgeon to address nearby spine segments, or levels, that may be mildly compressed.
Laminoplasty preserves 60 to 88% of motion at the affected levels of the spine. This is a greater percentage than either laminectomy or anterior surgery. Since neck pain is often related to motion — and some motion still remains after the procedure — patients may still have neck pain after laminoplasty.
Another disadvantage is that, in some cases, the lamina that is hinged can close by accident.
Combined Approach
Some patients will need combined anterior and posterior approaches to ensure the best outcome. This includes patients who have:
- Fixed or severe kyphosis (abnormal forward cervical spine curvature)
- Severe osteoporosis that has weakened the bone
- Multiple levels of involvement requiring extra stabilization
| Advantages | Disadvantages | |
|---|---|---|
| Anterior Approach |
|
|
| Advantages | Disadvantages | |
| Posterior Approach |
|
|
Risks of Cervical Spondylotic Myelopathy Surgery
As with any surgery, there are risks associated with cervical spine surgery. Possible complications can be related to the approach used, bone graft, healing, or long-term changes. In general, higher rates of complications from surgery are found in:
- Elderly patients
- Patients who are overweight
- Smokers
- Patients with diabetes
- Patients with multiple medical problems
Before your surgery, your doctor will discuss each of the risks with you and will take specific measures to help avoid potential complications.
General Risks
The potential risks and complications for any cervical spine surgery include:
- Infection
- Bleeding
- Nerve injury
- Spinal cord injury
- Reaction to anesthesia
- The need for additional surgery in the future
- Failure to relieve symptoms
- Tear of the sac covering the nerves (dural tear)
- Life-threatening medical problems, such as heart attack, lung complications, or stroke
Anterior Cervical Spine Surgery Risks
The potential risks and complications of anterior cervical spine surgery include:
- Soreness when swallowing or trouble swallowing
- Voice changes
- Trouble breathing
- Injury to the esophagus
- Degeneration of disk levels above or below the surgery level
Additional risks and complications of anterior cervical diskectomy and spinal fusion include:
- Misplaced, broken, or loosened plates and screws
- Complications relating to the bone graft, including hip pain (if an autograft is used), dislodgement (the graft moves out of place), fracture, or severe settling
- Nonunion of the spinal fusion (failure of the bone to fuse)
Posterior Cervical Spine Surgery Risks
The potential risks and complications of posterior cervical spine surgery include:
- Degeneration of disk levels above or below surgery level
- Injury to the vertebral artery
- Stretch on the nerves from the spinal cord drifting backwards
- Wound breakdown
Recovery From Cervical Spondylotic Myelopathy Surgery
After surgery, you will typically stay in the hospital for 1 or 2 days. This will vary, however, depending on the type of surgery you have and how many disk levels were involved. Most patients are able to walk and eat on the first day after surgery.
Depending on the procedure you have, a drain may be placed in your spine to collect any fluid or blood that may remain after surgery.
After anterior cervical spine surgery, it is normal to have trouble swallowing solid foods for a few weeks or have some hoarseness. For this reason, your doctor may prescribe antacids or recommend that your diet include softer foods, such as soup or milkshakes, in the early postoperative period.
You may need to wear a soft or rigid (stiff) collar at first. How long you should wear it will depend on the type of surgery you have.
Discharge Instructions
When you are discharged, your doctor will give you specific instructions to follow at home. These instructions will depend on the type of procedure you have.
General examples of discharge instructions after surgery may include the following (please note that your doctor may have different instructions that are customized to your specific circumstances):
- You will be encouraged to walk and sit in a chair as much as you are able to.
- Contact your doctor if you see signs of infection. Signs of infection include:
- Persistent fever (higher than 101.5°)
- Shaking chills
- Increased redness, tenderness, or swelling of your wound
- Drainage from your wound
- Increasing pain with both activity and rest
- Your staples or sutures can be removed at the follow-up office visit around 2 weeks after surgery. Sometimes your surgeon will use absorbable suture that will dissolve after your wound heals. This type of suture does not have to be removed.
- Your doctor may ask you to stop taking anti-inflammatory medication for six weeks after surgery.
- Do not lift anything heavier than 10 to 15 pounds.
- Do not drive a car until you are cleared by your doctor.
After spinal fusion, it may take 6 to 12 months for the bone to become solid. For this reason, your doctor may give you additional restrictions to follow. For example, right after your operation, your doctor may recommend only light activity, like walking. As you regain your strength, you will be able to slowly increase your activity level.
New Symptoms
Depending on the extent of your surgery and the number of spine levels fused, you may notice some neck stiffness or loss of motion after your procedure. Also, as nerves begin to wake up after surgery, you may experience different nerve symptoms or feelings than you had before. This is normal. Often, these symptoms and feelings will gradually improve after surgery over a period of 1 to 2 years.
If your nerve symptoms and pain get worse over time, or if you have any problems with infection or wound healing, contact your doctor.
Physical Therapy
Usually by 4 to 6 weeks, you can gradually begin to do range-of-motion and strengthening exercises as advised by your surgeon. Your surgeon may prescribe physical therapy during the recovery period to help you regain full function.
Return to Work
Most people are able to return to a desk job within a few days to a few weeks after surgery. They may be able to return to full activities by 3 to 4 months, depending on the procedure. For some people, healing may take longer.
Outcomes After Surgery for Cervical Spondylotic Myelopathy
Regardless of the approach used, the desired outcome of surgery is to stabilize the spine and prevent neurologic problems from worsening. A secondary goal is to potentially improve neck pain — as well as the motor, sensory, and other neurological symptoms that may be present. The goal of surgery is not necessarily to restore normal function.
Outcomes will vary from patient to patient. Typically, compared to pre-surgical symptoms:
- One-third (33%) of patients improve
- One-third (33%) stay the same
- One-third (33%) continue to worsen over time
In most cases, the symptoms you experience after surgery will be similar to the symptoms you experienced before surgery. Your doctor will discuss this with you and provide information on the likelihood of improvement in your specific situation.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.