Diseases & Conditions
Sprains, Strains, and Other Soft-Tissue Injuries
Soft tissue injuries typically affect muscles, tendons, and ligaments and most often occur during sports and exercise.
Sprains, strains, and contusions, as well as tendinitis and bursitis, are common soft-tissue injuries. Even with appropriate treatment, these injuries may require a long time to heal.
Cause
Soft-tissue injuries fall into two basic categories: acute injuries and overuse injuries.
- Acute injuries are caused by a sudden trauma, such as a fall, twist, or blow to the body. Examples include sprains, strains, and contusions.
- Overuse injuries occur gradually over time when an athletic or other activity is repeated so often that the soft tissues do not have enough time to recover before they are put under stress again. Tendinitis and bursitis are common soft-tissue overuse injuries.
Common Acute Soft-Tissue Injuries
Acute soft-tissue injuries vary in type and severity. When an acute injury occurs, initial treatment with the RICE protocol is usually very effective.
- Rest. Take a break from the activity that caused the injury. If the injury is to your leg, your doctor may also recommend that you use crutches to avoid bearing weight.
- Ice. Use cold packs for 20 minutes out of 1 hour, several times a day. Do not apply ice directly to the skin.
- Compression. To prevent additional swelling, wear an elastic compression bandage.
- Elevation. To reduce swelling, elevate the injury higher than your heart while resting.
Sprains
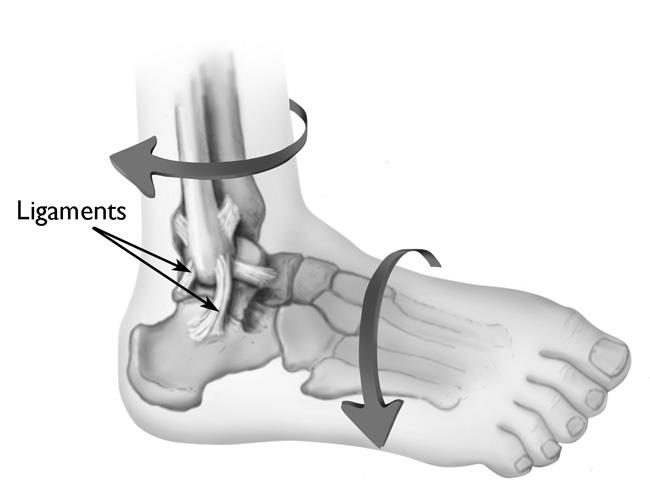
A sprain is a stretch and/or tear of a ligament, a strong band of connective tissue that connects the end of one bone with another. Ligaments stabilize and support the body's joints. For example, ligaments in the knee connect your femur (thighbone) to your tibia (shinbone), enabling you to walk.
The areas of the body that are most vulnerable to sprains are the ankles, knees, and wrists.
- A sprained ankle can occur when your foot turns inward, placing extreme tension on the ligaments of your outer ankle.
- A sprained knee can result from a sudden twist.
- A wrist sprain can occur if you fall onto an outstretched hand.
Sprains are classified by severity:
- Grade 1 sprain (mild): Slight stretching and some damage to the fibers of the ligament.
- Grade 2 sprain (moderate): Partial tearing of the ligament. There is abnormal looseness (laxity) in the joint when it is moved in certain ways.
- Grade 3 sprain (severe): Complete tear of the ligament. This may cause significant instability.
While the intensity varies, pain, bruising, swelling, and inflammation are common to all three categories of sprains.
- Treatment for sprains begins with the RICE protocol and physical therapy.
- Moderate sprains often require a period of bracing. For example, a CAM walking boot can be worn to help support and immobilize a sprained ankle, and a hinged knee brace might be worn to support a sprained knee.
- The most severe sprains may require surgery to repair torn ligaments.
Strains
A strain is an injury to a muscle and/or tendon. Tendons are fibrous cords of tissue that attach muscles to bone. Strains often occur in the back, neck, or leg (typically, the hamstring).
Similar to a sprain, a strain may be a simple stretch of your muscle or tendon, or it may involve a partial or complete tear of the muscle and tendon. Symptoms of a strain may include pain, muscle spasm, muscle weakness, swelling, inflammation, and cramping.
- Soccer, football, hockey, boxing, wrestling and other contact sports put athletes at risk for hamstring strains, as do sports that feature quick starts, such as basketball, sprinting, hurdling, and long jumping.
- Calf strains are common in runners, as well as sports that involve a lot of running, such as football, soccer, tennis, and basketball.
- Gymnastics, tennis, rowing, golf and other sports that require extensive gripping have a high incidence of hand sprains.
- Elbow strains frequently occur in racquet, throwing, and contact sports.
The recommended treatment for a strain is the same as for a sprain: rest, ice, compression and elevation. This should be followed by simple exercises to relieve pain and restore mobility. Surgery may be required for a more severe tear.
Contusions (Bruises)
Contusions occur when a direct blow (or repeated blows) by a blunt object strikes part of the body, crushing underlying muscle fibers and connective tissue without breaking the skin. A contusion can result from falling or jamming the body against a hard surface. Discoloration of the skin is caused by blood pooling around the injury.
Most contusions are mild and respond well to the RICE protocol.
A quadriceps contusion caused by a direct blow, such as a helmet to the thigh, can be minimized with a compression wrap and temporary immobilization of the thigh with the knee in a bent position.
If symptoms persist, seek medical care to prevent permanent damage to the soft tissues.
Common Overuse Soft-Tissue Injuries
Tendinitis
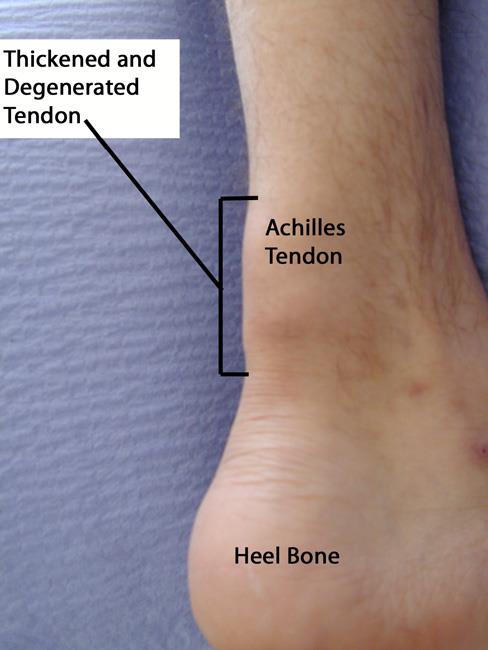
Tendinitis is an inflammation or irritation of a tendon or the covering of a tendon (called a sheath). It is caused by a series of small stresses that repeatedly aggravate the tendon. Symptoms typically include swelling and pain that worsens with activity.
- Baseball and softball players, swimmers, tennis players, volleyball players, and golfers are susceptible to tendinitis in their shoulders and elbows.
- Soccer and basketball players, runners, and aerobic dancers are prone to tendon inflammation in their knees and ankles.
Tendinitis may be treated by rest to eliminate stress, anti-inflammatory medication, steroid injections, splinting, and exercises to correct muscle imbalance and improve flexibility. Persistent inflammation may cause significant damage to the tendon, which may require surgery.
Bursitis
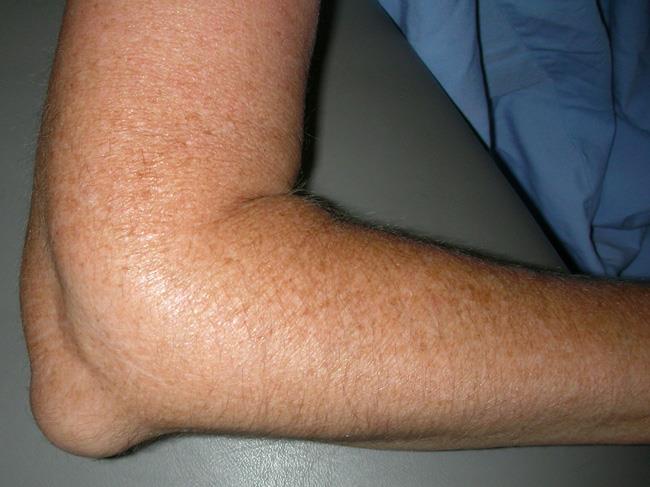
Bursae, are small, jelly-like sacs that are located throughout the body, including around the shoulder, elbow, hip, knee, and heel. They contain a small amount of fluid, and are positioned between bones and soft tissues, acting as cushions to help reduce friction.
Bursitis is inflammation of a bursa. Repeated small stresses and overuse can cause the bursa to swell. Many people experience bursitis in association with tendinitis.
Bursitis can usually be relieved with changes in activity and anti-inflammatory medications, such as ibuprofen. If swelling and pain do not respond to these measures, your doctor may recommend removing fluid from the bursa and injecting a corticosteroid medication. The steroid medication is an anti-inflammatory drug that is stronger than the medication that can be taken by mouth. Corticosteroid injections usually help relieve pain and swelling.
Although surgery is rarely necessary for bursitis, if the bursa becomes infected, an operation to drain the fluid from the bursa may be necessary. In addition, if the bursa remains infected or the bursitis returns after all nonsurgical treatments have been tried, your doctor may recommend removal of the bursa.
Removal (excision) of the bursa can be done using a standard incision (open procedure), or as an arthroscopic procedure with small incisions and miniature surgical instruments. Your doctor will talk to you about which procedure is right for your situation.
Prevention
Injuries often occur when people suddenly increase the duration, intensity, or frequency of their activities. Many soft-tissue injuries can be prevented through proper conditioning and training. Other prevention tips include:
- Use proper equipment. Replace your athletic shoes as they wear out. Wear comfortable, loose-fitting clothes that let you move freely and are light enough to release body heat.
- Aim for balanced fitness. Develop a balanced fitness program that incorporates cardiovascular exercise, strength training, and flexibility. Add activities and new exercises cautiously. Whether you have been sedentary or are in good physical shape, do not try to take on too many activities at one time. It is best to add no more than one or two new activities per workout.
- Warm up. Warm up to prepare for exercise, even before stretching. Run in place for a few minutes, breathe slowly and deeply, or gently rehearse the motions of the exercise to follow. Warming up increases your heart and blood flow rates and loosens up muscles, tendons, ligaments, and joints.
- Stretch. Begin stretches slowly and carefully until reaching a point of muscle tension. Hold each stretch for 10 to 20 seconds, then slowly and carefully release it. Inhale before each stretch and exhale as you release. Do each stretch only once. Never stretch to the point of pain, always maintain control, and never bounce on a muscle that is fully stretched.
- Drink water. Drink enough water to prevent dehydration and heat injury. Drink 1 pint of water 15 minutes before you start exercising and another pint after you cool down. Have a drink of water every 20 minutes or so while you exercise.
- Cool down. Make cooling down the final phase of your exercise routine. It should take twice as long as your warm-up. Slow your motions and lessen the intensity of your movements for at least 10 minutes before you stop completely. This phase of a safe exercise program should end when your skin is dry and you have cooled down.
- Rest. Schedule regular days off from vigorous exercise and rest when tired. Fatigue and pain are good reasons not to exercise.
- Don't be a "weekend warrior." Try to get at least 30 minutes of moderate physical activity every day. If you are pressed for time, you can break it up into 10-minute chunks. And be aware that jumping back into an activity or sport after a long time away from it can lead to injury. If you are resuming a sport you haven't played recently, start slowly and give your body time to adjust before you go all-out.
Whether an injury is acute or due to overuse, if your symptoms persist, contact your doctor.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.