Diseases & Conditions
Scaphoid Fracture of the Wrist
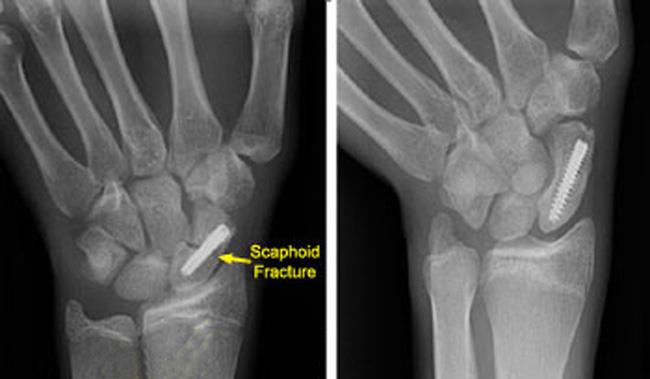
A scaphoid (navicular) fracture is a break in one of the small bones (carpal bones) of the wrist. This type of fracture occurs most often after a fall onto an outstretched hand.
Symptoms of a scaphoid fracture typically include swelling and pain in the wrist just below the base of the thumb. Pinching, grasping, pushing, and pulling often make pain worse.
Treatment for a scaphoid fracture can range from casting to surgery. Optimal treatment can depend on the fracture's severity (how bad the break is) and location in the bone. Because parts of the scaphoid have a poor blood supply — and a fracture can further disrupt (slow or stop) the flow of blood to the bone — complications with the healing process are more common in scaphoid fractures than in fractures of other bones.
Anatomy
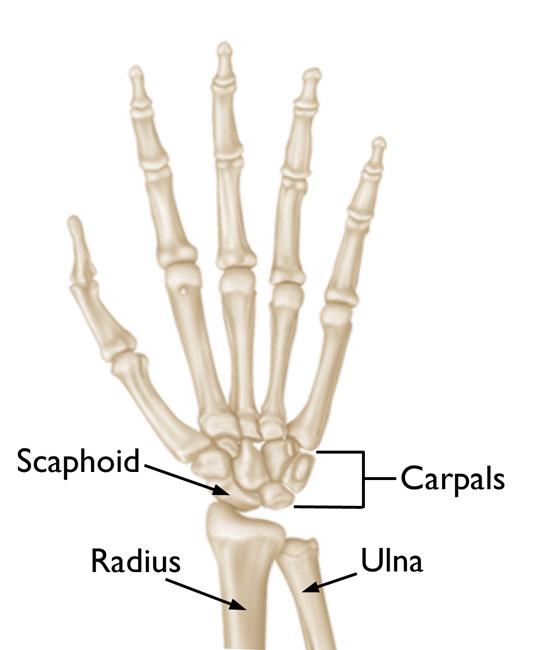
The wrist is formed by the two bones of the forearm — the radius and the ulna — and eight small carpal bones. The carpal bones are arranged in two rows at the base of the hand. There are four bones in each row.
The scaphoid bone is one of the carpal bones on the thumb side of the wrist, just above the radius. The bone is important for both motion and stability of the wrist joint.
The word "scaphoid" comes from the Greek term for "boat." The scaphoid bone resembles a boat with its relatively long and curved shape. The scaphoid is especially important to wrist function because it links the proximal row of carpal bones (the bones closer to the radius and ulna) to the distal row of carpal bones (the bones closer to the fingers). Smooth and unrestricted (free) motion of the scaphoid is necessary to allow for optimal motion of the wrist.
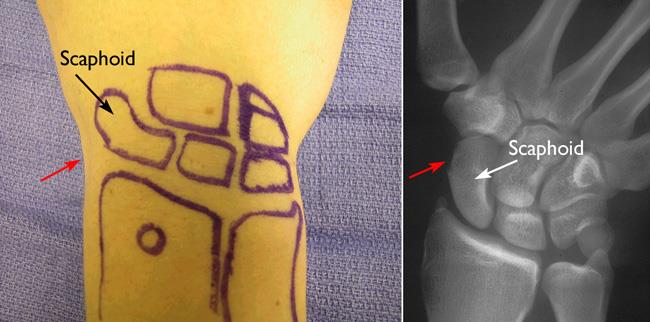
The scaphoid bone can most easily be identified when your thumb is held in a "hitch-hiking" or "thumbs-up" position. It is located at the base of the hollow made by the thumb tendons on the back of the wrist. Often referred to as the "anatomic snuffbox," this area is typically where you feel the most tenderness or pain when a scaphoid fracture occurs.
As mentioned above, the scaphoid has a poor blood supply.
Throughout the body, blood runs from the heart to the extremities (arms and legs) — from close to the body (proximal) to the fingers and toes (distal). This direction of flow is found in most bones in the arms and legs, with the blood running from the part of the bone that is closest to the body to the part of the bone that is closest to the fingers or toes.
However, the blood supply to the scaphoid runs “backwards”: Blood enters the part of the scaphoid closest to the thumb (distal) and runs back toward the part of the scaphoid closest to the body (proximal). For this reason, fractures of the distal scaphoid heal much more quickly than fractures of the proximal scaphoid. In fact, there is a risk that fractures of the proximal scaphoid will completely disrupt the blood supply, causing part of the scaphoid to necrose, or die. This phenomenon, called “avascular necrosis,” can cause long-term problems in the wrist.
Description
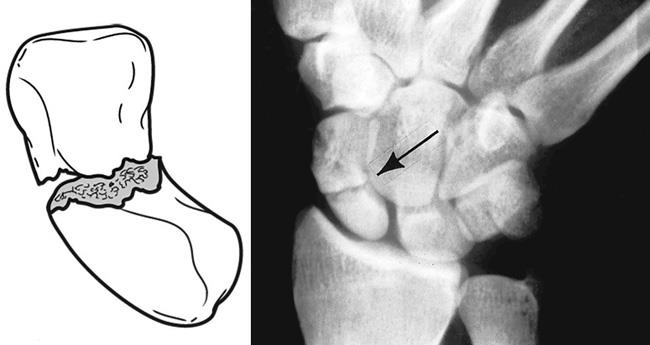
A scaphoid fracture is usually described by its location within the bone. Most commonly, the scaphoid breaks in its mid-portion, called the "waist." Fractures can also occur at both the proximal and distal ends of the bone.
Scaphoid fractures are classified according to the severity of displacement — or how far the pieces of bone have moved out of their normal position:
- Non-displaced fracture. In this type of fracture, the bone fragments line up correctly.
- Displaced fracture. In this type of fracture, the bone fragments have moved out of their normal position. There may be gaps between the pieces of bone or fragments may overlap each other.
Cause
A scaphoid fracture usually occurs when you fall onto an outstretched hand, with your weight landing on your palm. The end of the larger forearm bone (the radius) may also break in this type of fall, depending on the position of the hand on landing.
The injury can also happen during sports activities or motor vehicle collisions.
Fractures of the scaphoid occur in people of all ages, including children. There are no specific risk factors or diseases that make you more likely to experience a scaphoid fracture. Some studies have shown that using wrist guards during high-energy activities like inline skating, skateboarding, and snowboarding can help decrease your chance of breaking a bone around the wrist.
Symptoms
Scaphoid fractures usually cause swelling and pain at or near the anatomic snuffbox and on the thumb side of the wrist. The pain may be severe when you move your thumb or wrist, or when you try to pinch, grasp, push, or pull something.
Unless your wrist is deformed, it might not be obvious to you that your scaphoid bone is broken. With some scaphoid fractures, the pain is not severe and may be mistaken for a wrist sprain.
Pain in your wrist that does not go away within a day of injury may be a sign of a fracture — so it is important to see a doctor if your pain does not go away. Prompt treatment of a scaphoid fracture may help avoid potential complications.
Doctor Examination
Physical Examination
During the exam, your doctor:
- May talk with you about your general health
- Will ask how your injury happened
- Will ask you to describe your symptoms
Your doctor will also examine your wrist. With most fractures, there will be tenderness directly over the scaphoid in the anatomic snuffbox. Your doctor will also look for:
- Swelling
- Bruising
- Loss of motion
Tests
X-rays. X-rays provide images of dense structures, such as bone. Your doctor will likely order an X-ray to help determine whether you have a scaphoid fracture and whether the broken pieces of bone are displaced. An X-ray will also help your doctor determine if you have any other fractures or dislocations.
In some cases, a scaphoid fracture does not show up on an X-ray right away. If your doctor suspects you have a fracture but it is not visible on X-ray, they may recommend that you wear a wrist splint or cast for 2 to 3 weeks and then return for a follow-up X-ray. Often, scaphoid fractures become visible on X-ray only after a period of time. During this waiting period, you should wear your splint or cast and avoid activities that might cause further injury.
Magnetic resonance imaging (MRI) scan. Your doctor may order an MRI to learn more about the bones and soft tissues in your wrist. An MRI can sometimes show a fracture of the scaphoid before it can be seen on X-ray.
Computerized tomography (CT) scan. A CT scan can be helpful in revealing a fracture of the scaphoid and can also show whether the bones are displaced. Your doctor may use information from the CT scan to help determine your treatment plan.
Treatment
The treatment your doctor recommends will depend on several factors, including but not limited to:
- The location of the break in the bone
- Whether the bone fragments are displaced
- How long ago your injury happened
- Your age and general health
Nonsurgical Treatment
Fracture near the thumb. Non-displaced scaphoid fractures that are closer to the thumb (distal pole) are likely to heal with proper protection and restricted activity. This part of the scaphoid bone has a good blood supply, which is necessary for healing.
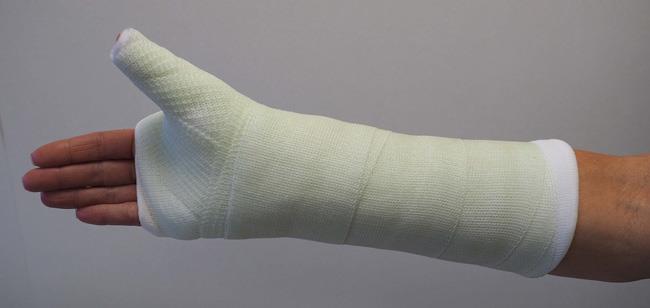
For this type of fracture, your doctor may place your forearm and hand in a cast or a splint. The cast or splint will usually be below the elbow and will include your thumb.
Healing time varies from patient to patient. Your doctor will monitor your healing with X-rays or other imaging studies.
Fracture near the forearm. If the scaphoid is broken (but non-displaced) in the middle of the bone (waist) or closer to the forearm (proximal pole), healing can be more difficult. These areas of the scaphoid do not have a very good blood supply, as explained above.
If your doctor treats this type of fracture with a cast, the cast may include the thumb and may extend above the elbow. Typically, you will have to stay in the cast or splint longer with this type of fracture compared to a more distal fracture near the thumb.
Bone stimulator. In some cases, your doctor may recommend the use of a bone stimulator to assist in fracture healing. This small device delivers low-intensity ultrasonic or pulsed electromagnetic waves that stimulate healing.
Surgical Treatment
If your scaphoid is broken at the waist or proximal pole and/or if the fracture is displaced, your doctor may recommend surgery. The goal of surgery is to realign and stabilize the fracture, giving it a better chance to heal.
Reduction. During the surgery, your doctor will manipulate the bone back into its proper position. In some cases, this is done using a limited (smaller) incision and special guided instruments. In other cases, it is performed through an open incision with direct manipulation of the fracture. For some fractures, your doctor may use a tiny camera called an arthroscope to aid in the reduction.
Internal fixation. During this part of the procedure, metal implants — including screws, plates, and/or wires — are used to secure the fractured ends together and hold the scaphoid in place until the bone is fully healed.
The location and size of the surgical incision depend on which part of the scaphoid is broken. Sometimes, the implants can be placed in bone fragments through a small incision. In other cases, a larger incision is needed to ensure that the fragments of the scaphoid line up properly before fixing it. The incision may be made on either the palm side or the back of your wrist.
Bone graft. In some cases, a bone graft may be used with or without internal fixation. A bone graft is new bone that is placed around the broken bone. It can stimulate bone production and healing. The bone graft may be taken from your forearm, elbow, hip, or other area. Some companies also make grafts that can be placed in the fracture, so the surgeon does not have to take bone from your body.
Recovery
Whether your treatment is surgical or nonsurgical, you may be required to wear a cast or splint for up to 6 months or until your fracture has healed. Unlike most other fractures, scaphoid fractures tend to heal slowly. During this time, unless advanced activity is approved by your doctor, you should avoid the following activities:
- Lifting, carrying, pushing, or pulling more than 1 pound of weight
- Throwing with your injured arm
- Participating in contact sports
- Climbing ladders or trees
- Participating in activities with a risk of falling onto your hand, such as inline skating or jumping on a trampoline
- Using heavy machinery or machines/pieces of equipment that vibrate
- Smoking (which can delay or prevent fracture healing; it can also affect healing after surgery)
Some patients have wrist stiffness after scaphoid fractures. This is more common in patients who wear a cast for a long time or require more extensive surgery.
It is important to maintain full finger motion throughout your recovery period. Your doctor will provide an exercise program, and may refer you to a trained hand therapist who will help you regain as much range of motion and strength in your wrist as possible.
Despite hand therapy and a great deal of effort by the patient during home therapy, some patients may not recover the same range of motion and strength that they had before their injury.
Complications
Nonunion
A bone that fails to heal is called a nonunion. Nonunions are more common after scaphoid fractures because the blood supply to the scaphoid bone is poor. Good blood supply to a bone is very important in fracture healing — since blood carries oxygen and nutrients to the site of the fracture to aid in healing.
If your scaphoid fracture does not heal, your doctor may consider more surgery to insert a bone graft. There are several types of bone grafts.
- For nonunions, your doctor may use a special kind of graft with its own blood supply (vascularized graft).
- In the case of a fracture that has collapsed, your doctor may use a structural graft with plenty of strength — possibly taken from your hip.
Avascular Necrosis
In scaphoid fractures — especially those in which the bone fragments have become displaced — the blood supply to the bone may be disrupted. If the blood supply to one of the fragments is reduced significantly or lost completely, that fragment of bone will not get enough nutrients and the cells in the bone will die. The bone will not heal properly if this occurs. This condition is called avascular necrosis.
A vascularized bone graft may be the most effective treatment for this condition — as long as the bone has not collapsed significantly or arthritis has not developed in the wrist.
Arthritis
Over time, nonunion and avascular necrosis of the scaphoid can lead to arthritis of the wrist. Arthritis occurs when the articular cartilage in the joint becomes worn and frayed — sometimes to the point where bone rubs on bone.
Symptoms of arthritis in the wrist may include:
- Aching
- Stiffness
- Decreased range of motion in the wrist
- Pain with activities such as lifting, gripping, or weightbearing
Treatment for arthritis focuses on improving symptoms. At first, this may include:
- Taking anti-inflammatory medicine or over-the-counter analgesics (pain relievers)
- Wearing a splint when the wrist is painful
- Avoiding activities that aggravate the wrist
- Possibly, a steroid injection into the wrist, which can help relieve pain
If conservative treatment does not relieve your symptoms, your doctor may recommend surgery. There are many types of procedures that can be performed for wrist arthritis.
New Developments
For specific fracture patterns, some doctors are now using a very small incision — less than 1/2-inch long — to align the fracture and to place a screw in the scaphoid. This procedure is performed using a special X-ray machine to help guide the placement of the screw.
Additionally, your doctor may insert a small camera called an arthroscope into your wrist to look directly at the fracture. This may help with the reduction and the fixation of the bone and may decrease the surgical incision length needed.
There is ongoing research on different types of bone grafts and bone graft substitutes to speed bone healing. Additional substances, such as bone morphogenic proteins (BMP), are also being evaluated to improve healing potential.
Newer types of wrist braces may help prevent injury, and better imaging may lead to earlier diagnosis of these difficult fractures.
Contributed and/or Updated by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.