Diseases & Conditions
Nonunions
With modern treatment methods, most broken bones (fractures) heal without any problems. After a broken bone is treated, new bone tissue (callus) begins to form and connect the broken pieces.
Some broken bones do not heal even with the best possible surgical or nonsurgical treatment. In some cases, certain risk factors make it more likely that a bone will fail to heal.
- When a broken bone fails to heal it is called a nonunion.
- A delayed union is when a fracture takes longer than usual to heal.
Bone Healing
For bone healing to happen, the bone needs adequate stability and blood supply. Good nutrition also plays a role in bone healing.
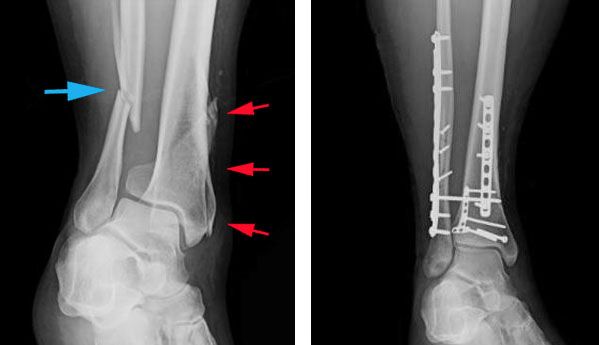
- Stability. All treatment of broken bones follows one basic rule: The broken pieces must be put back into position and prevented from moving out of place until they heal. Some fractures can be held in position with a cast. Some fractures require surgery and are stabilized with devices like screws, plates, rods, and frames.
- Blood supply. Blood delivers the components (oxygen, growth factors etc.) required for healing to the fracture site. The blood supply to the injured bone usually returns on its own during the healing process.
- Nutrition. A broken bone also needs adequate nutrition to heal. Eating a healthy and well-balanced diet that includes protein, calcium, vitamin C, and vitamin D is the best way to ensure adequate nutrition; dietary supplements that go beyond the daily requirements are not effective. (The rare exception is the severely malnourished patient with many injured organs. In this case, the doctor will discuss dietary guidelines and make recommendations for adding dietary supplements.)
Causes
Nonunions occur when the bone lacks adequate stability, blood flow/nutrition, or both. They also are more likely if the bone breaks from a high-energy injury, such as from a motor vehicle collision, because severe injuries often disrupt blood supply to the broken bone.
Risk Factors
Several factors increase the risk of nonunion.
- Use of tobacco or nicotine in any form (smoking, vaping, chewing tobacco, and nicotine gum or patches) inhibits bone healing and increases the chance of a nonunion. Learn more: Smoking and Musculoskeletal Health
- Older age
- Severe anemia
- Diabetes
- A low vitamin D level
- Hypothyroidism
- Poor nutrition
- Medications, including anti-inflammatory drugs such as aspirin, ibuprofen, and prednisone. The physician and patient should always discuss the risks and benefits of using these medications during fracture healing
- Infection
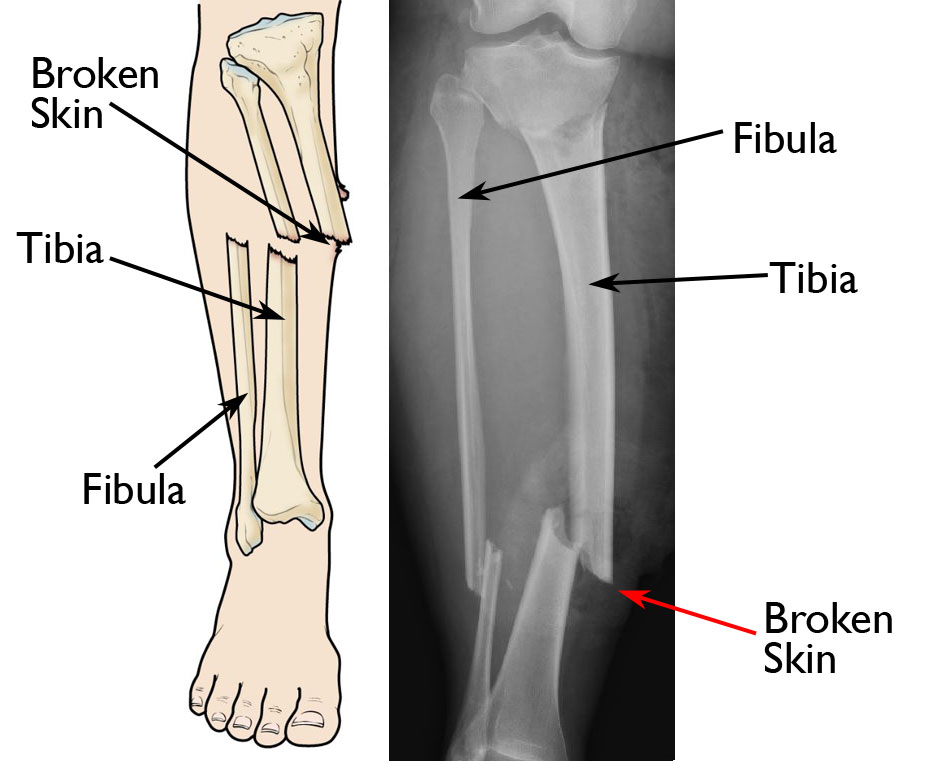
- A complicated open fracture (also known as a compound fracture); with an open fracture, there is an open wound near the fracture, usually caused by a piece of bone breaking through the skin
Blood Supply
Nonunions are more likely to happen if the injured bone has a limited blood supply.
- Some bones, such as toe bones, are naturally stable and have an excellent blood supply. They can be expected to heal with minimal treatment.
- Some bones, such as the femoral head and neck (upper thighbone) and scaphoid (small wrist bone), have a limited blood supply. The blood supply can be destroyed when these bones are broken. Learn more: Hip Fractures, Scaphoid Fractures
- Some bones, such as the tibia (shinbone), have a moderate blood supply; however, an injury can disrupt it. For example, a high-energy injury can damage the skin and muscle over the bone and destroy the external blood supply. In addition, the injury can destroy the internal blood supply found in the marrow at the center of the bone. Learn more: Tibia (Shinbone) Shaft Fractures
Symptoms
Patients with nonunions usually feel pain at the site of the break long after the initial pain of the fracture disappears. This pain may last months, or even years. It may be constant, or it may occur only when the broken arm or leg is used.
Doctor Examination
To diagnose a nonunion, the doctor uses imaging tests that provide detailed pictures of the bone and surrounding soft tissues. Depending on which bone is involved, these tests may include:
- X-rays
- Computed tomography (CT) scans
- Magnetic resonance imaging (MRI).
These imaging tests let the doctor see the broken bone and follow the progress of its healing.
A nonunion may be diagnosed if the doctor finds one or more of the following:
- Persistent pain at the fracture site
- A persistent gap with no bone spanning the fracture site
- No progress in bone healing when repeated imaging tests are compared over several months
- Inadequate healing in a time period that is usually enough for normal healing
If the doctor diagnoses a nonunion, they may order blood tests to investigate the cause of the fracture not healing. These tests may show infection or another medical condition that may slow bone healing, such as anemia or diabetes.
Treatment
Nonsurgical and surgical treatments for nonunions have advantages and disadvantages. More than one alternative may be appropriate. Talk to your doctor about the benefits and risks of the various options to treat your nonunion. Your doctor will recommend the treatment option that is best for you.
Nonsurgical Treatment
Some nonunions can be treated nonsurgically.
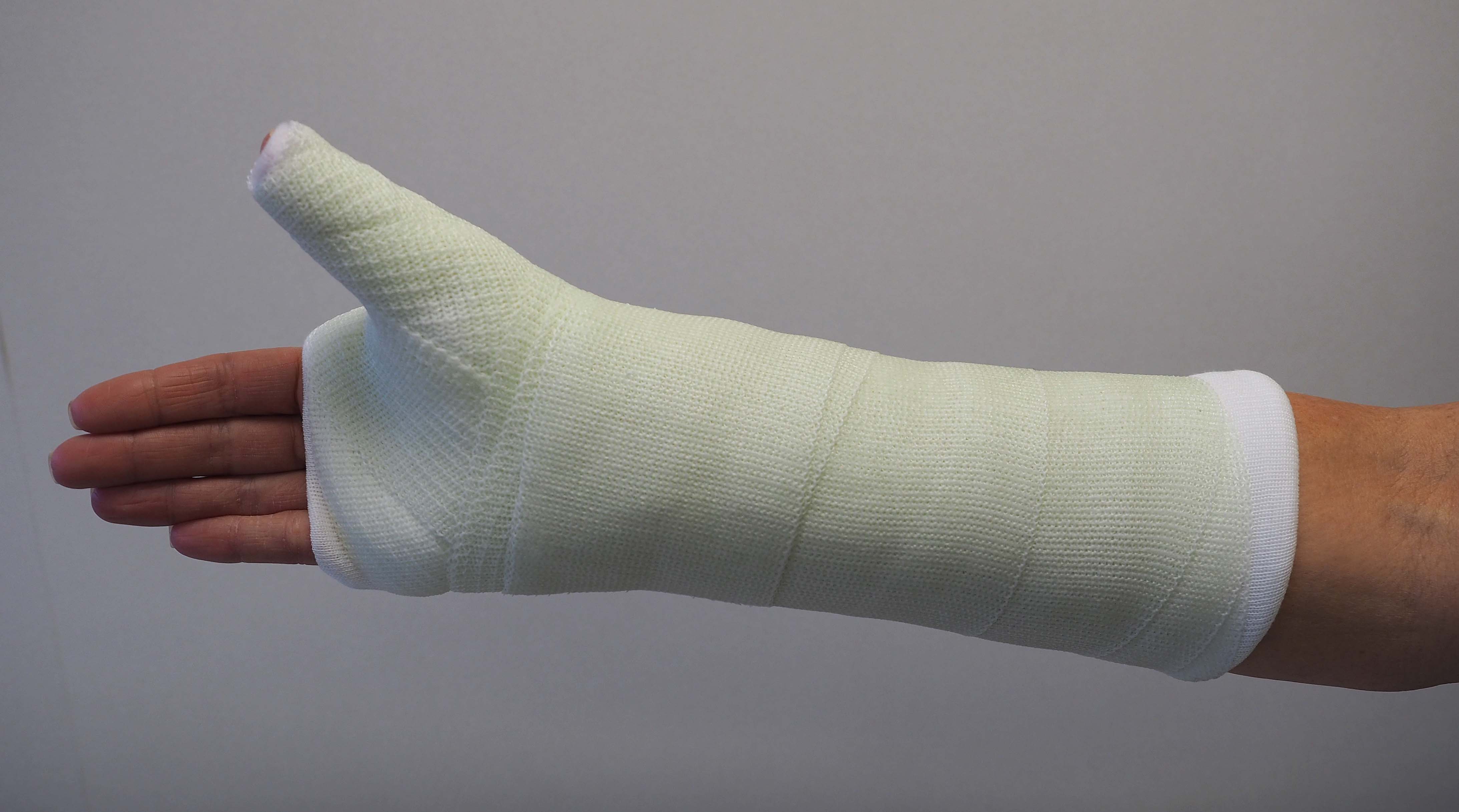
- One form of nonsurgical treatment is to immobilize the nonunion with a splint, cast, or brace for a period of time.
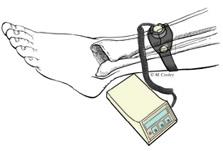
- In addition to immobilizing the nonunion, your doctor may have you use a bone stimulator. This small device delivers ultrasonic or pulsed electromagnetic waves that stimulate healing. The patient places the stimulator on the skin over the nonunion for 20 minutes to several hours daily. This treatment must be used every day to be effective.
Surgical Treatment
Surgery is needed when nonsurgical methods fail. You may also need a second surgery if the first surgery failed. Surgical options include bone graft or bone graft substitute, internal fixation, and/or external fixation.
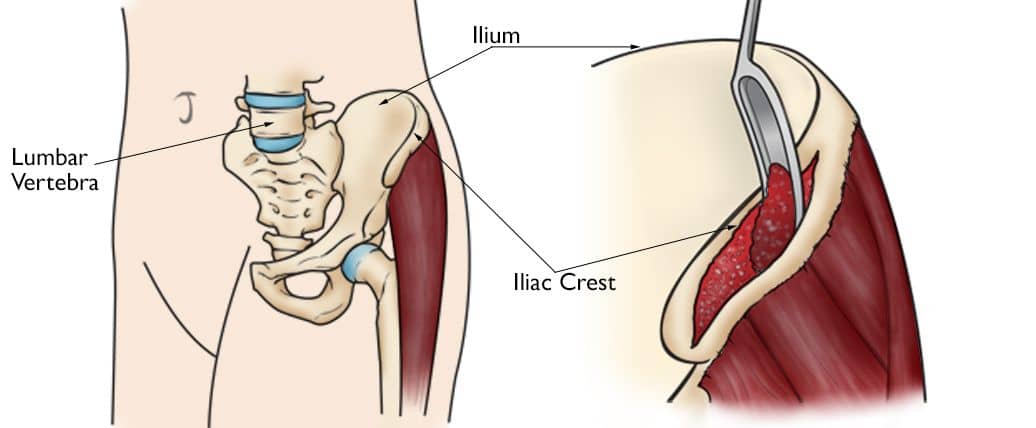
- Bone Graft. During this procedure, bone from another part of the body may be placed into the fracture nonunion site to "jump start" the healing process. A bone graft provides a scaffold on which new bone may grow. Bone grafts also provide fresh bone cells and the naturally occurring chemicals the body needs for bone healing.
During the procedure, the surgeon makes an incision and removes (harvests) pieces of bone from different areas of the patient's body. These pieces of bone are then transplanted to the nonunion site. The rim of the pelvis, or iliac crest, is a common location for harvesting bone. However, bone grafts can be taken from a variety of locations that your surgeon will discuss with you. The amount of bone removed usually does not cause functional, structural, or cosmetic problems.
-
- Allograft (cadaver bone graft). With an allograft (cadaver) bone graft, surgeons do not have to harvest bone from the patient, which reduces the pain involved with treating the nonunion. Like a traditional bone graft, an allograft provides scaffolding for the patient's bone to heal across the area of the nonunion. As time goes on, the patient's bone replaces the cadaver bone. Although there is a theoretical risk of infection, the cadaver bone graft is processed and sterilized to minimize this risk, and the transmission of diseases from donor bone is very rare.
- Bone graft substitutes and/or osteobiologics. As with allografts, the use of bone graft substitutes enables patients to avoid the bone harvesting procedure and related pain. Although bone graft substitutes do not provide the fresh bone cells needed for normal healing, they do provide a scaffold of chemicals needed for growth.
Depending on the type of nonunion, any of the above materials, or a combination of materials, may be used to fix the nonunion.
Bone grafts (or bone graft substitutes) alone provide no stability to the fracture site. Unless the nonunion is inherently stable, you may also need more surgical procedures (internal or external fixation) to improve stability.
- Internal Fixation. Internal fixation stabilizes a nonunion. The surgeon attaches metal plates and screws to the outside of the bone or places a nail (rod) inside the bone to hold the bone in position.
If a nonunion occurs after internal fixation, another internal fixation surgery may be needed to increase stability. The surgeon may use a more rigid device, such as a larger rod (nail) or a longer plate. Removing a previously inserted nail and inserting a larger one (exchange nailing) increases stability and stimulates healing within the bone. Internal fixation can be combined with bone grafting to help stability and stimulate healing.
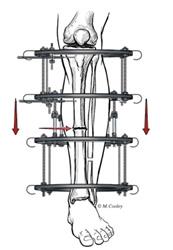
- External fixation. External fixation stabilizes the injured bone, as well. The surgeon attaches a rigid frame to the outside of the injured arm or leg. The frame is attached to the bone with wires or pins. External fixation may be used to increase the stability of the fracture site if instability contributed to the development of the nonunion. External fixation can treat nonunions in a patient who also has bone loss and/or infection.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.