Diseases & Conditions
Prepatellar (Kneecap) Bursitis
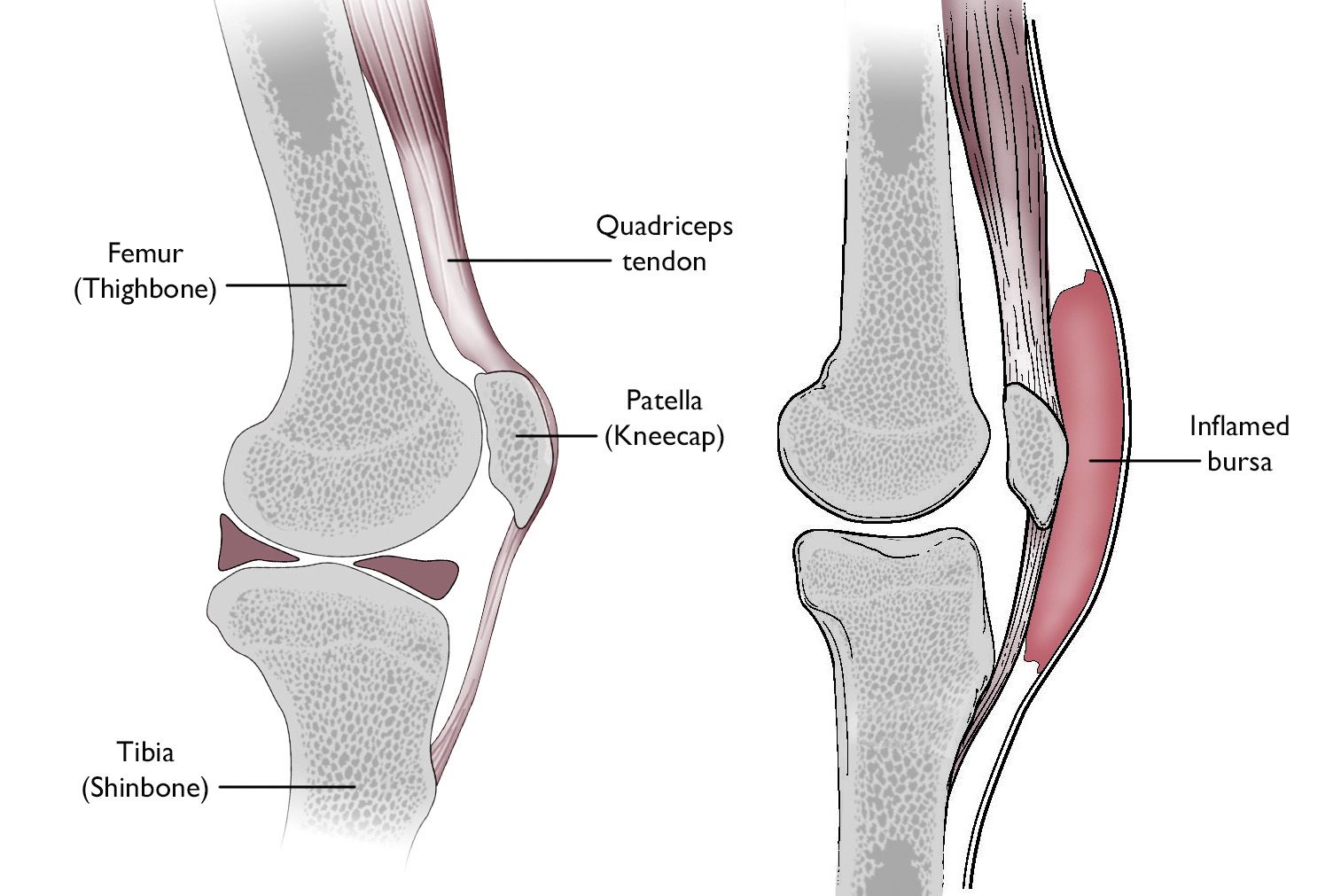
Bursae are small, jelly-like sacs that are located throughout the body, including around the shoulder, elbow, hip, knee, and heel. They contain a small amount of fluid, and they are positioned between bones and soft tissues, acting as cushions to help reduce friction.
Prepatellar bursitis is an inflammation of the bursa in the patella (front of the kneecap). It occurs when the bursa becomes irritated and produces too much fluid, which causes it to swell and put pressure on the nearby parts of the knee.
Cause
Prepatellar bursitis is often caused by pressure from constant kneeling. Plumbers, roofers, carpet layers, coal miners, and gardeners have a greater risk of developing the condition.
A direct blow to the front of the knee can also cause prepatellar bursitis. Athletes who participate in sports in which direct blows or falls on the knee are common, such as football, wrestling, or basketball, have a greater risk of the condition.
Other people who are more vulnerable to the condition include those with rheumatoid arthritis or gout.
Prepatellar bursitis can also be caused by a bacterial infection. If a knee injury — such as an insect bite, scrape, or puncture wound — breaks the skin, bacteria may get inside the bursa sac and cause an infection. This is called infectious bursitis. Infectious bursitis is less common, but more serious and must be treated more urgently, though not always with surgery.
Symptoms
- Pain with activity, but not usually at night
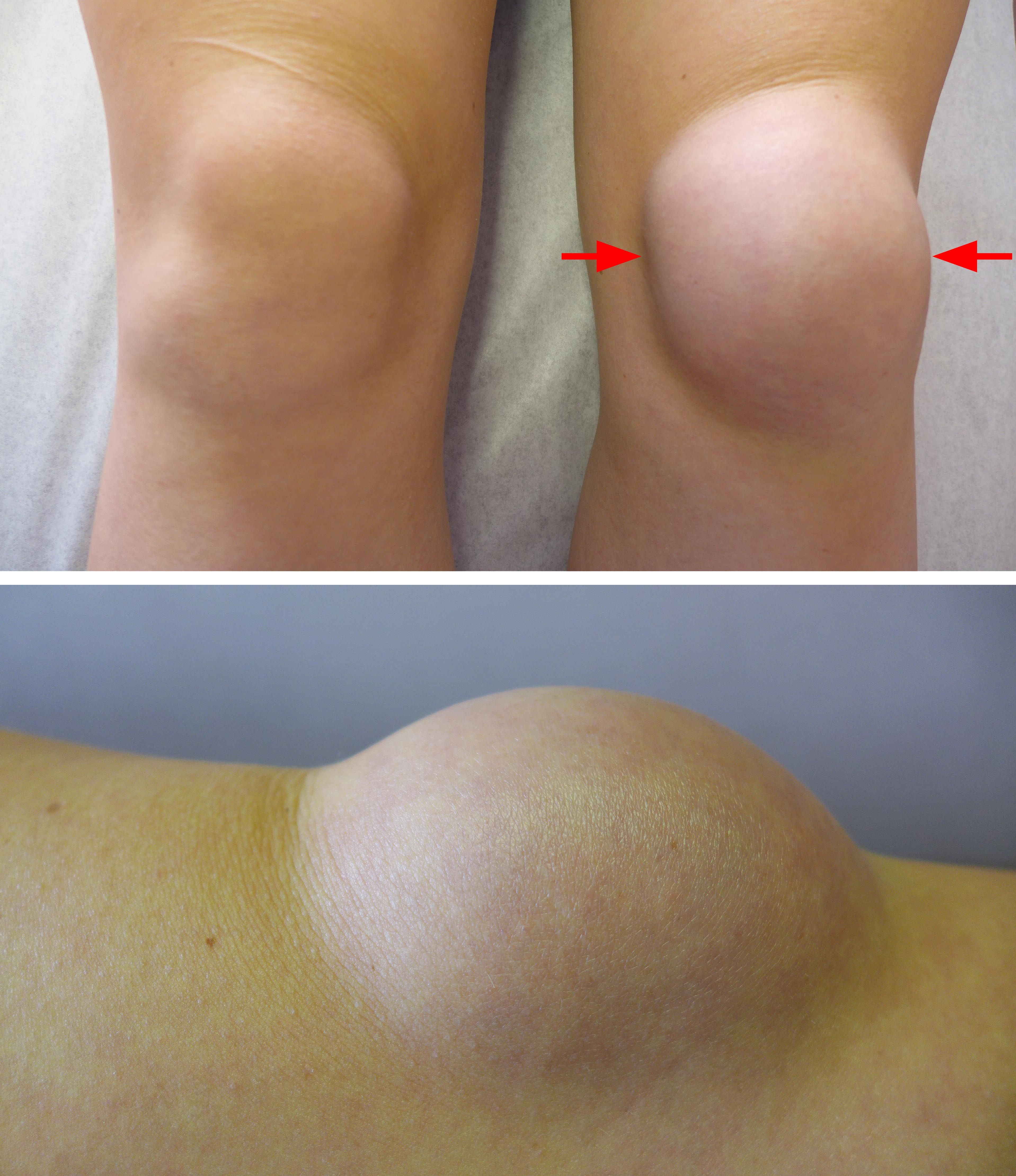
- Rapid swelling on the front of the kneecap
- Tenderness and warmth to the touch
- Bursitis caused by infection may produce fluid and redness, as well as fever and chills
Doctor Examination
Medical History and Physical Examination
Your doctor will ask you about your symptoms, such as the severity of your pain, how long you have had symptoms, and your risk factors for developing prepatellar bursitis.
Your doctor will likely ask whether you have had any signs or symptoms of infection, such as fever or chills. Prepatellar bursitis caused by an infection requires a different treatment plan.
During the physical examination, your doctor will inspect your affected knee and compare it to your healthy knee. They will examine your knee, checking for tenderness, and will also assess the range of motion in your knee and whether pain keeps you from bending it.
Tests
- X-rays. X-rays provide clear pictures of dense structures like bone. Your doctor may order X-rays to make sure there is not a fracture or other bony problem that is causing your symptoms.
- Other imaging tests. The diagnosis of bursitis is usually made on physical examination, but your doctor may order computerized tomography (CT) and/or magnetic resonance imaging (MRI) scans to check for other soft tissue injuries.
- Aspiration. If your doctor is concerned about the possibility of infection, they may use a needle to drain fluid from the bursa and send this sample to the lab for analysis.
Treatment
Nonsurgical treatment is usually effective as long as the bursa is only inflamed and not infected:
- Activity modification. Avoid the activities that worsen symptoms. Substitute another activity until the bursitis clears up. Low-impact exercise, such as cycling or using the elliptical machine, is a good option.
- Ice. Apply ice at regular intervals 3 or 4 times a day for 20 minutes at a time. Each session should reduce swelling a lot if you are also resting your knee.
- Elevation. Elevate the affected leg except when you need to walk.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). Medications such as naproxen and ibuprofen may relieve pain and control inflammation. Acetaminophen can be used as an alternative if you cannot take NSAIDs (e.g., you have an allergy or are on other medications that may interact with NSAIDs).
If the swelling and pain do not respond to these measures, your doctor may drain (aspirate) the bursa with a needle, then inject the bursa with a corticosteroid (cortisone injection). The corticosteroid is an anti-inflammatory drug that is stronger than medications that can be taken by mouth.
Infectious bursitis is initially treated with antibiotics. Surgical drainage is required if the infection does not respond to antibiotics alone.
Draining the bursa may also treat chronic swelling that causes disability, but if the swelling continues, your orthopaedic surgeon may recommend surgical removal of the bursa. After surgery, the knee should regain its flexibility in a few days, and you can resume normal activities in a few weeks.
Prevention
You can help prevent bursitis by following these simple recommendations:
- Wear kneepads if you work on your knees or participate in contact sports such as football, basketball, or wrestling.
- Rest your knees regularly by stopping to stretch your legs. You may also consider switching activities on a regular basis to avoid prolonged stress on your knees.
- Apply ice and elevate your knees after a workout.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.