Diseases & Conditions
Progressive Collapsing Foot Deformity (Flatfoot)
Progressive collapsing foot deformity (PCFD), formerly known as adult acquired flatfoot (AAF), is a complex condition of the foot and ankle that results in flattening of the arch of the foot as well as other less obvious deformities. Another name for this condition is posterior tibial tendon dysfunction (PTTD).
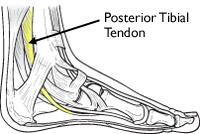
Though likely the result of a connected group of problems, flatfoot is most commonly believed to begin with dysfunction of the posterior tibial tendon, an important structure in supporting the arch of the foot. When the tendon becomes inflamed or torn, it may not be able to provide stability and support for the arch of the foot, resulting in flatfoot.
Description
As the name would suggest, progressive collapsing foot deformity represents a broad range of disorders that may start as a subtle deformity with only mild symptoms but can progress to a very painful, crippling, and poorly functioning flatfoot.
Most patients in the early stages of the disease can be treated without surgery, using orthotics and braces.
If orthotics and braces do not provide relief, surgery can be an effective way to help with the pain and improve the function of the foot. Surgical options vary widely depending on the stage of the disease and amount of deformity.
- Surgery might be as simple as removing the inflamed tissue or repairing a simple tear in the tendon.
- However, surgery is usually very complex, and most patients will still notice some limitation in activity after surgery.
Anatomy
There are multiple important structures that contribute to the normal arch of the foot, including tendons (which connect muscles to bones) and ligaments (which connect two or more bones to each other). Two of the most vital structures are:
- The posterior tibial tendon (PTT). The PTT attaches one of the calf muscles (the tibialis posterior muscle) to the bones on the inside arch of the foot. You may be able to see or feel this tendon as it runs behind the inside bump of your ankle (the medial malleolus). The main function of the tendon is to hold up the arch and support the foot when walking. It also helps you stand on your toes or turn your foot and ankle inward.
- The spring ligament connects the heel bone (calcaneus) to one of the bones on the inside of the foot (navicular). It is a very important ligament for supporting the arch of the foot.
Whether inflammation and poor function of these structures are the cause or result of flatfoot is difficult to say. It is most commonly believed that dysfunction of the PTT is one of the main issues that contributes to the development of a flatfoot.
Sometimes, there is an injury to the spring ligament before PTT function starts to worsen. If this ligament is not injured before the PCFD, it is often torn, or at least stretched, in later stages of flatfoot.
In addition to the spring ligament, there are other smaller ligaments connecting the small bones of the inside of the foot that also help support the arch. The deltoid ligament is a large, strong ligament that connects the ankle to the heel bone and the bones of the inside of the foot. As flatfoot gets worse over time, this ligament also becomes stretched and weakened, leading to an acquired flatfoot deformity that includes the ankle.
Cause
There are multiple causes of PCFD, and the cause is likely not the same in each patient. These are some potential issues that can result in PCFD:
- Midfoot arthritis or loose ligaments can lead to increased stress on the posterior tibial tendon and cause it to slowly tear.
- An acute injury, such as from a fall, can tear the PTT or cause it to become inflamed.
- The PTT can tear due to overuse. For example, people who participate in high-impact sports, such as basketball, tennis, or soccer, may have tears of the tendon from repetitive use. Non-athletes can develop similar issues in the tendon over time, especially those who often wear non-supportive footwear like sandals.
- There is likely a strong genetic component to the development of PCFD.
Regardless of the initial cause:
- As the PTT becomes inflamed and weak, it is less able to hold up the arch and support the foot while walking.
- The arch begins to collapse, or sag, putting extra stress on the other structures that support the arch, such as the spring ligament.
- As these structures also become stretched and weakened, the PTT must try to work even harder to support the arch, starting a vicious cycle.
- Eventually the tendon and ligaments may completely tear. Without the support of tendons and ligaments, bones can shift significantly, causing pain from impingement (the bone puts pressure on another structure, such as another bone) and arthritis.
Posterior tibial tendon dysfunction and flatfoot are more common in women and in people over the age of 40. Additional risk factors include obesity, diabetes, and hypertension.
Symptoms
- Pain in the arch or along the inside of the foot and ankle, where the PTT lies. There may also be swelling along the tendon if it is inflamed or torn. You may feel pain before you can see any deformity.
- Pain and weakness with activity. Some people will have trouble walking or standing for a long time. High-intensity or high-impact activities, such as running, can be very difficult. Pain may also be worse when you are wearing non-supportive footwear, like sandals. In addition to pain, you may notice weakness when attempting to "push-off" with or stand on your toes.
- Pain on the outside of the ankle. As collapse of the arch worsens, the heel bone may shift outward relative to the ankle. If the shift is severe enough, the heel bone can put pressure on the outside ankle bone (this is called "impingement").
Doctor Examination
Medical History and Physical Examination
Your doctor will take a complete medical history and ask about your symptoms.
During the foot and ankle examination, the doctor will check to see whether these signs are present:
- Swelling and pain along the posterior tibial tendon. Swelling and pain are usually found just behind and below the inside ankle bump. The arch itself may also be painful.
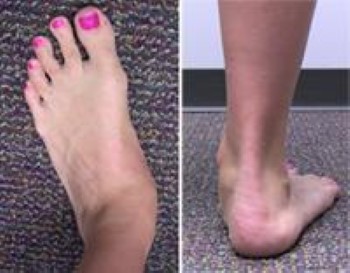
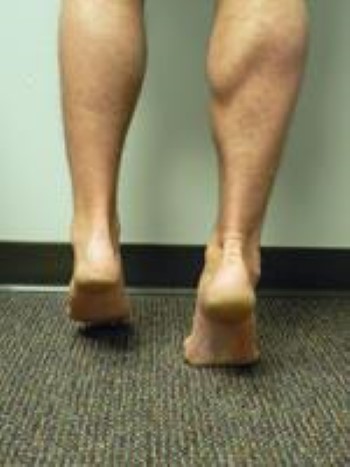
- Changes in the shape of the foot. The foot should be examined with the patient standing. A flat arch is usually the earliest and most obvious deformity. Other common deformities that develop as the condition progresses include the heel sliding outward from under the ankle and the toes turning outward relative to the foot and ankle. These changes can be seen when looking at the heel from behind the patient. In a normal foot, the heel is straight under the calf, and only the fourth and fifth toes are seen. In a flatfoot deformity, the heel may angle outwards relative to the calf and ankle, and more toes can be seen (this is called the "too many toes" sign).
- Difficulty with the "single limb heel rise" test. Being able to stand on one leg and come up on "tiptoes" requires a healthy posterior tibial tendon. When a patient cannot stand on one leg and raise the heel, the reason could be a problem with the posterior tibial tendon.
- Limited flexibility. The doctor may try to move the foot from side to side. The treatment plan for posterior tibial tendon tears varies depending on the flexibility of the foot. The treatment for a foot where there is no motion or motion is limited is different than treatment for a flexible foot.
- The range of motion of the ankle is affected. Upward motion of the ankle (dorsiflexion) can be limited in flatfoot. The limited motion is due to tightness of the calf muscles.
Imaging Tests
Other tests which may help your doctor confirm your diagnosis include:
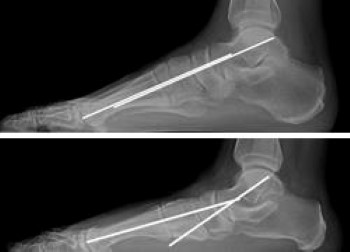
X-rays. X-rays provide detailed pictures of dense structures, like bone. They are useful to detect arthritis and other changes in alignment of the bones that may be contributing to pain and deformities. Most of the deformities present in flatfoot can be seen on plain X-rays, as long as they are taken with the patient standing (weightbearing X-rays). Then, if surgery is needed, X-rays help the doctor make measurements to determine which surgery would be most helpful.
Computerized tomography scan (CT Scan). CT scans are like 3D X-rays and therefore give the doctor an even more detailed look at the bones. The surgeon may use them to look for subtle changes that may not be obvious on X-rays, thus indicating which deformities and arthritic joints need to be corrected in surgery.
Ideally, these scans are done with the patient standing (a weightbearing CT) to evaluate how the bones look when the foot is supporting the patient's weight. However, this requires specialized equipment that is not available everywhere.
Magnetic resonance imaging (MRI). MRI scans create better images of soft tissues (like tendons and ligaments) than X-rays or CT scans do. Your doctor may order an MRI to look for inflammation or tearing of these structures or to look for other potential sources of symptoms when the diagnosis is in doubt.
Ultrasound. An ultrasound uses high-frequency sound waves that echo off of structures inside the body to create a picture of the bone and tissue. An ultrasound can be ordered to show the posterior tibial tendon, but it is usually not needed to diagnose flatfoot.
Nonsurgical Treatment
Symptoms will be relieved in most patients with appropriate nonsurgical treatment. Pain may last longer than 3 months even with early treatment. For patients who have had pain for many months, it is not uncommon for the pain to last another 6 months after treatment starts.
Rest
- Decreasing or even stopping activities that worsen the pain is the first step.
- Switching to low-impact exercise is helpful. Biking, elliptical machines, or swimming do not put a large impact load on the foot, and most patients are able to do these activities without any issues.
- Weight loss is also a very effective way to take stress off of the arch and its supporting structures.
Ice
Apply cold packs on the most painful area of the posterior tibial tendon for 20 minutes at a time, 3 or 4 times a day to keep down swelling. Do not apply ice directly to the skin. Placing ice over the tendon immediately after completing an exercise helps to decrease the inflammation around the tendon.
Nonsteroidal Anti-inflammatory Drugs (NSAIDs)
Anti-inflammatory drugs, such as ibuprofen or naproxen, reduce pain and inflammation. NSAIDs are available over the counter, or your doctor may give you a daily prescription version (for example, meloxicam). Topical anti-inflammatory medications, which you rub onto the painful area, may also help.
It is important to understand that while these medications can be very effective at decreasing inflammation and pain in the tendon or arthritic joints, they do not treat the underlying condition and will not change the shape of the foot.
Be sure to talk to your doctor about the side effects of these medications before you start taking them, especially if you have heart, kidney, or stomach problems.
Orthotics
An orthotic is a shoe insert designed to support and position the foot for more comfortable walking. It is the most common nonsurgical treatment for a flatfoot.
- An over-the-counter orthotic may be enough for patients with a mild change in the shape of the foot. There are many different orthotics on the market aimed at supporting the arch and relieving pain from flatfoot. Ask your doctor if they recommend a specific over-the-counter orthotic for your foot.
- A custom orthotic may be required if you have moderate to severe changes in the shape of the foot. The custom orthotic is more costly, but it allows the doctor to better control the position your foot.
Braces
- A simple over-the-counter lace-up ankle brace may help mild to moderate flatfoot. The brace can support the joints of the ankle and back of the foot, thus taking tension off of the tendon.
- More heavy-duty braces (Arizona brace, Richie brace) may be needed in severe flatfoot that is stiff or arthritic. These braces can be customized and are sometimes successful at helping patients with advanced deformities avoid surgery.
Immobilization
A short leg cast or walking boot may be used for 6 to 8 weeks. This allows the tendon to rest and the swelling to go down. However, a cast causes the other muscles of the leg to atrophy (decrease in strength) and thus is only used if no other nonsurgical treatment works.
Your doctor may recommend a period of immobilization — meaning you keep the foot from moving at all — in a boot or cast followed by wearing a brace once the initial pain and swelling have gone down.
Physical Therapy
Physical therapy that strengthens the tendon can help patients with mild disease of the posterior tibial tendon. Stretching the calf and Achilles tendon to improve the tightness of the ankle is also an important part of any therapy program for flatfoot.
Steroid Injection
Cortisone is a very powerful anti-inflammatory medicine that your doctor may consider injecting into painful areas.
Though very commonly used for arthritis in many joints in the body, a cortisone injection into the posterior tibial tendon is not normally done because it carries a risk of tendon rupture. Discuss this risk with your doctor before getting an injection.
Surgical Treatment
Surgery should be considered if the pain does not get better after several months of appropriate treatment. The type of surgery depends on:
- The severity of the deformity (how bad it is)
- Whether there is arthritis
- How flexible the foot is (how much it can move)
Surgical reconstruction can be extremely complex. The following is a list of the commonly used operations, but it is not all-inclusive. A combination of these procedures is often needed to address each component (part) of the PCFD.
Tenosynovectomy (Cleaning the Posterior Tibial Tendon)
This surgery is used when there is very mild disease — meaning there is pain and swelling over the tendon, but the shape of the foot has not changed significantly.
During the procedure, the surgeon will clean away and remove the inflamed tissue (synovium) around the tendon. They can also repair small tears in the tendon, if needed.
Tenosynovectomy can be performed alone or in addition to other procedures. The main risk of this surgery is that the tendon may continue to degenerate (deteriorate, or get worse), and the pain may return.
Gastrocnemius Recession or Achilles Tendon Lengthening
These operations aim to lengthen the calf muscle (gastrocnemius) or Achilles tendon and are therefore useful in patients who have tightness and limited ability to bend the ankle upward. They can help prevent flatfoot from returning but may create some weakness when pushing off and climbing stairs.
The surgeries are usually performed through a small incision on the back of the calf. Complication rates are low but can include nerve damage and muscle weakness. These surgeries are often performed along with other techniques for treating flatfoot.
Tendon Transfer
Tendon transfers can be done in a flexible flatfoot to re-create the function of the damaged posterior tibial tendon. In this procedure:
- The diseased tendon is removed and replaced with another tendon from the foot; or
- If the disease is not too significant in the posterior tibial tendon, the transferred tendon is attached to the preserved (not removed) PTT
The most commonly used tendon for this transfer procedure is the tendon that bends the little toes down, called the flexor digitorum longus (FDL). The tendon that bends the big toe down (flexor hallucis longus, or FHL) can also be used. After the transfer, the toes will still be able to move, and most patients will not notice a change in how they walk.
Although the transferred tendon can substitute for the posterior tibial tendon, the foot still is not normal. In most cases, you will need additional operations to correct the shape of the foot (see below), because if the shape of the foot is not corrected, the tendon will continue to be stressed and is likely to re-tear at some point.
Ligament Repair
The ligaments supporting the bones of the arch are often torn, or at least stretched and weakened. If the arch is flexible, the surgeon may choose to repair these ligaments (especially the spring ligament) as part of your flatfoot surgery.
- If the ligament is still mostly healthy, the surgeon can do the repair using only the natural ligament tissue.
- However, in most cases, the surgeon will have to use supportive materials to help re-create the ligament, such as strong stitches.
As with the tendon transfer procedures, the ligament will continue to stretch and tear over time if the shape of the foot is not corrected, so a ligament repair is usually just one part of a larger flatfoot surgery.
Osteotomy (Cutting and Shifting Bones)
An osteotomy can change the shape of a flexible flatfoot to recreate a more "normal" arch shape. Correcting the shape of the foot is important to take stress off of the PTT, spring ligament, and other arch-supporting structures.
- One very commonly performed osteotomy for flatfoot involves cutting the heel bone (calcaneus) and moving it from its outward position back under the center of the ankle.
- Another type of osteotomy of the calcaneus involves lengthening the outside portion of the heel to help push the toes back to center (this corrects the "too many toes" deformity).
- Other osteotomies of the foot or toes may also be required to restore the shape of the arch itself.
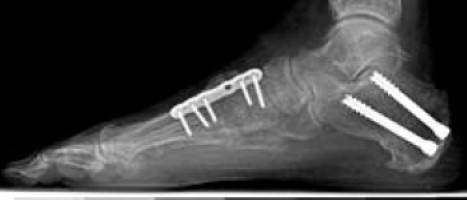
Some osteotomies require the use of bone graft to fill in gaps and help the bones heal. Screws or plates hold the cut bones in places while they heal.
Arthrodesis (Joint Fusion)
Sometimes flatfoot is stiff or there is also arthritis in key joints of the foot. In these cases, the foot will not be flexible enough to be treated successfully with bone cuts and tendon transfers.
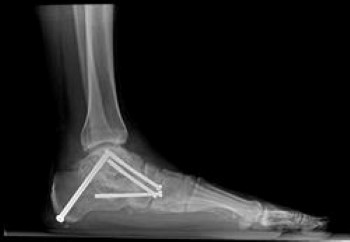
Fusion (arthrodesis) of a joint or joints can be used to realign the foot and remove arthritis.
- Fusion involves removing any cartilage in the joint and fixing the bones to each other in a corrected position.
- Over time, the two bones heal together so they become one large bone without a joint, which eliminates joint pain (arthritis).
- Screws or plates hold the bones in places while they heal.
A rigid flatfoot may require the heel bone to be realigned and fused under the ankle bone. To correct the shape of the arch itself, the bones of the inside part of the foot also may need to be fused.
Though fusing two bones eliminates motion between them, patients who typically need this surgery already have a rigid deformity with little to no motion remaining in those joints. They should see an improvement in the way they walk as well as a decrease in pain. Specifically, the pain they may experience on the outside of the ankle joint should decrease due to getting rid of the arthritis and the impingement between the heel and ankle. The up and down motion of the ankle is not greatly affected.
With any fusion, the body may fail to heal the bones together. This is called a nonunion, and it may require another operation.
Ankle Surgery for Flatfoot
In severe cases of flatfoot, the deformity can progress (move up) into the ankle joint, making the joint unstable or even arthritic.
- If the ankle joint is simply unstable but not arthritic, the surgeon may choose to repair the inside ankle ligament (deltoid ligament).
- If the ankle is arthritic or stiff, you may need a bigger operation, such as ankle replacement or ankle fusion, to correct the deformity and relieve pain.
Complications
- The most common complaint is that pain is not completely relieved. Patients may also be unhappy with the shape of their foot after surgery, thinking that the foot was supposed to look completely "normal" again. However, it is important to keep in mind that often the main goal of surgery is to prevent deformity and pain from getting worse; it may not be realistic to expect that the pain will be gone and the foot will appear "normal." Talk to your surgeon before your procedure about what you can expect after surgery.
- Nonunion (failure of the body to heal the bones together) can be a complication with both osteotomies and fusions and may require repeat surgery to get the bones to heal.
- Wound infection is another possible complication.
Diabetics and smokers are at increased risk for most of these complications.
Surgical Outcome
Most patients have good results from surgery. The main factors that determine surgical outcome are the amount of motion possible before surgery and the severity of the flatfoot. The more severe the problem, the longer the recovery time and the less likely a patient will be able to return to sports. In most patients, it takes 6 months or more before healing is complete and there is any great improvement in pain.
These are some ways you can help ensure good results from surgery:
- Follow the surgeon's instructions after surgery (most important, do not walk on the foot until the doctor says it is OK to do so).
- Take excess stress off the foot (lose weight, avoid high-impact activities).
- Wear supportive footwear.
- Reduce any risk factors for complications (e.g., quit smoking, keep diabetes controlled).
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.