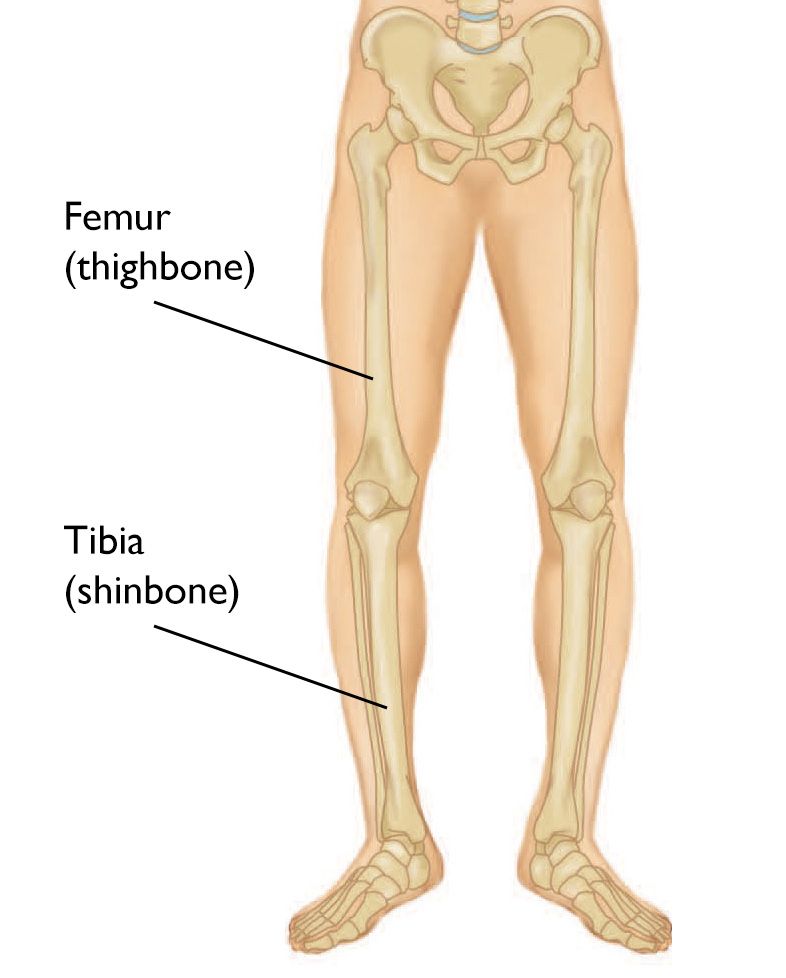
Diseases & Conditions
Malunion in the Lower Limb
When a broken bone heals in an abnormal position, it is called a malunion. There are different abnormal positions in which a bone can heal. For example, the bone may be crooked, rotated, or shorter than it was before. A combination of these deformities may also be present.
While some malunions do not impact a patient’s daily activities and do not need treatment, those that occur in the lower limb often result in significant functional impairment. A malunion in this area can cause a limp, lead to pain and arthritis, and be cosmetically displeasing.
Treatment for a malunion in the lower limb often involves surgery to correct the alignment of the fractured bone and improve function in the involved leg.
Description
Bone Healing
Most fractures heal without any problems, as long as certain conditions are met:
- The bone must be held together while it heals. Some fractures can be held in position with a cast. Some fractures require surgical fixation with devices like screws, plates, rods and frames.
- The bone ends must have a good blood supply and receive enough nutrition (i.e., protein, calcium, and vitamins) to heal.
Most of the time, these conditions are met, and the bone heals in good alignment. This is called a union. If a bone does not heal, it is called a nonunion. Lastly, the bone may heal, but in an abnormal position—this is called a malunion.
Impact of Malunion in the Lower Limb
A malunion can occur in any bone. However, some malunions are better tolerated than others because they do not interfere with daily activities or limit mobility.
Malunions that involve the lower limb often require treatment, however, and may result in one or more of the following conditions in the involved leg:
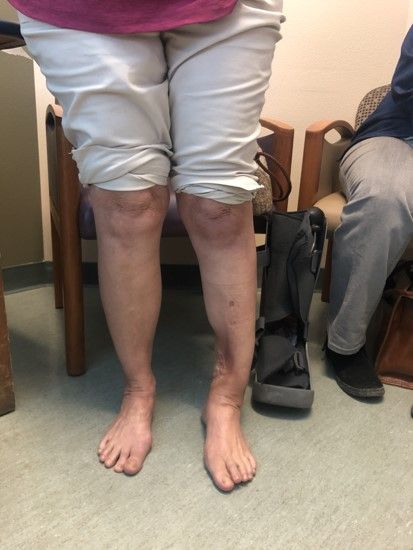
- Limb length discrepancy. The leg is shorter or longer than the other leg.
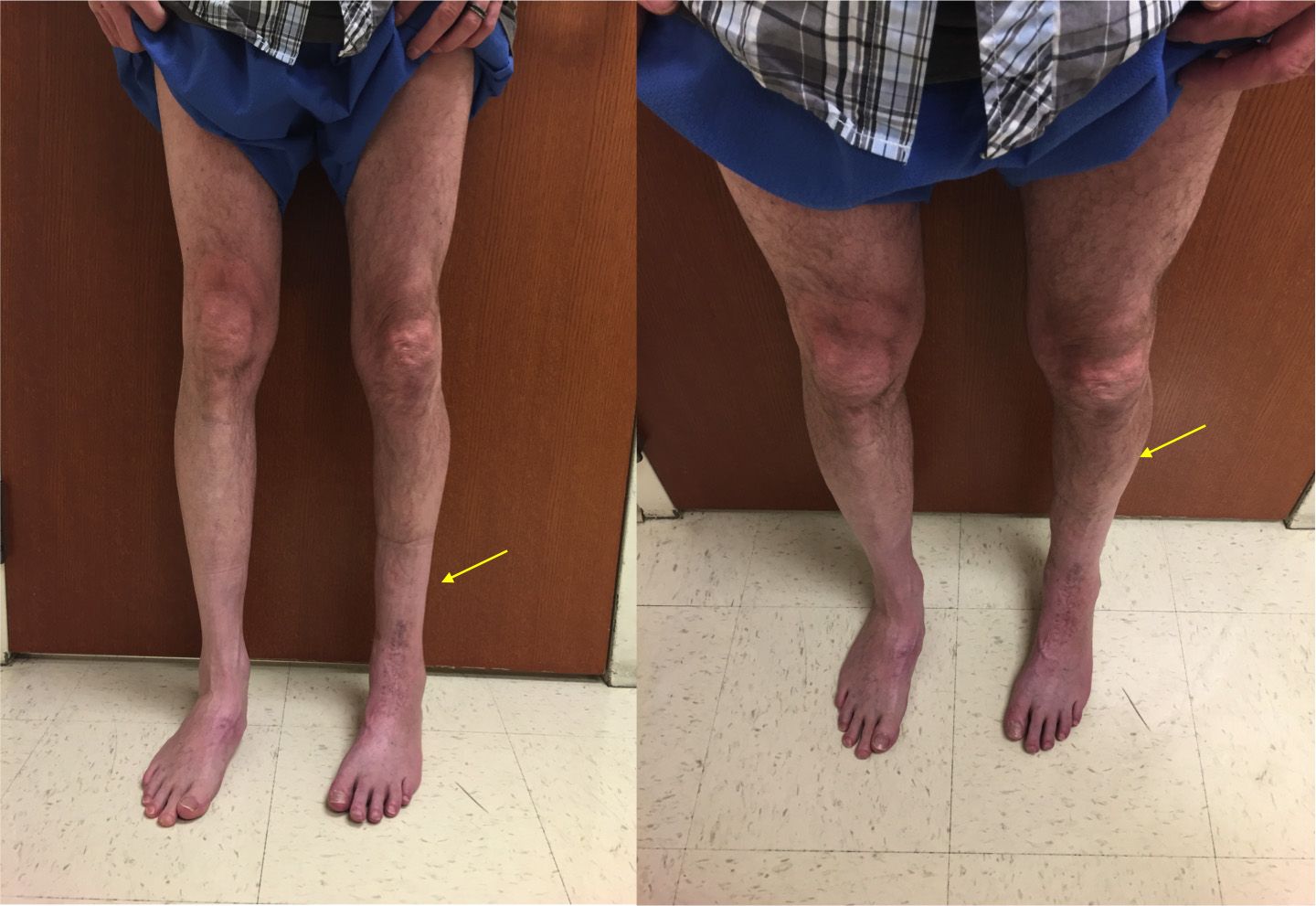
- A crooked limb:
- Bowed leg. The knee angles out when the leg is straightened.
- Knock knee. The knee angles in when the leg is straightened.
- Flexion contracture. The inability to fully straighten or extend the leg.
- Rotational abnormality. The foot is turned inward or outward.
Cause
Even with appropriate treatment, some fractures are more likely to result in a malunion. Comminuted fractures—in which the bone shatters into many pieces—are difficult to put back together and are more likely to heal in an unacceptable alignment.
Malunion can also occur if a broken bone shifts during the healing process. This is more likely to occur in fractures treated with casting but can also occur after surgical fixation.
Symptoms
Malunion symptoms are most obvious after the fracture is healed, but some can be observed early on. Symptoms vary, depending on which bone is affected and the severity and position of the malunion.
For example, if a broken thighbone heals with a malunion, it may cause you to limp or to walk with your foot internally or externally rotated. You also may have hip, knee, or ankle pain, even though these areas were not necessarily injured. This is because a malunion can alter your walking mechanics in such a way that your other joints take on too much of your body weight.
Doctor Examination
Physical Examination
Your doctor will ask you to describe your symptoms and will carefully examine the area that was previously broken. He or she will want to know how you broke the bone and what type of treatment you have had in the past. Your doctor will also check range of motion in the joints around the suspected malunion. Symmetry is important, so he or she will also examine your “normal” side for comparison.
Gait analysis. During the physical examination, your doctor will closely observe your gait (the way you walk). A malunion in the lower limb will frequently alter your gait, causing you to limp or to point your feet inward or outward.
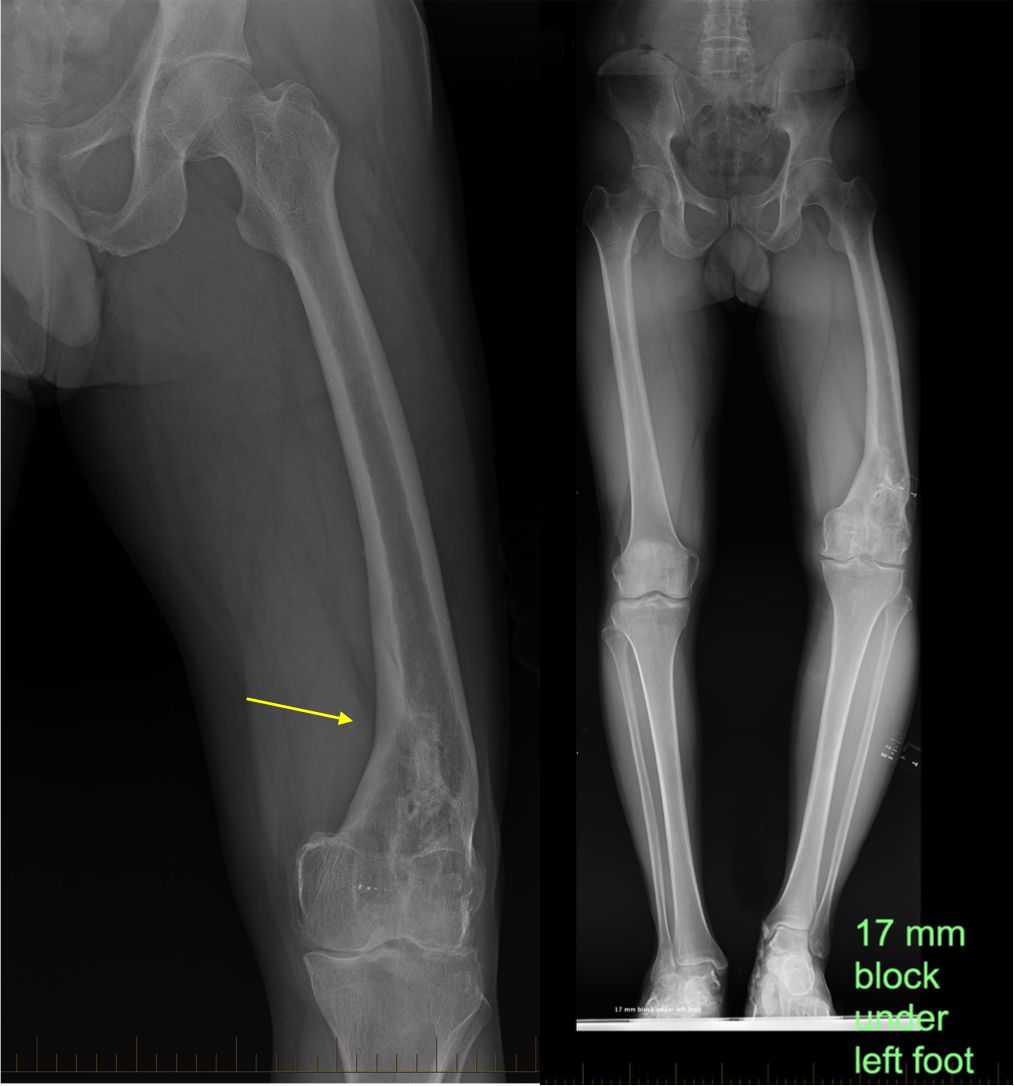
Measuring a leg length discrepancy. If the malunion has resulted in the involved leg being shorter or longer than the other leg, your doctor will measure the leg length discrepancy. To do this, he or she may place a series of wooden blocks under the shorter leg until your hips are level, then measure the blocks to determine the difference.
Imaging Studies
X-rays. X-rays provide images of dense structures, such as bone. Your doctor will order x-rays to learn more about the nature of the malunion and to get a more precise measurement of a leg length discrepancy.
Scanograms. This is a special type of x-ray that uses a series of three images and a ruler to measure the length of the bones in the legs. Your doctor may order a scanogram instead of, or in addition to, a traditional x-ray.
Computerized tomography (CT) scans. CT scans provide cross-sectional images of bones. Your doctor may order a CT scan to learn more about a rotational deformity and will use to one to help plan your treatment.
Treatment
Treatment for a malunion in the lower limb depends on a number of factors, including:
- The patient’s symptoms
- The involved bone
- The severity of the condition
- Whether the malunion impacts mobility and daily functioning
Nonsurgical Treatment
If the malunion is not painful and does not cause impaired functioning, your doctor may recommend simple nonsurgical treatments.
Shoe lift. If there is a smaller leg length discrepancy, wearing a shoe lift fitted to the inside or outside of your shoe can often improve the ability to walk and help relieve back pain. Shoe lifts are inexpensive and can be removed easily if they are not effective.
Bracing. In some cases, bracing can provide additional support and improve the ability to walk by pulling the involved leg into a straighter position.
Surgical Treatment
If you and your doctor decide that correcting the malunion can sufficiently improve your pain, discomfort, and mobility, then surgery may be recommended.
Osteotomy. This is the procedure most often used to correct a malunion. In an osteotomy, the involved bone is cut or rebroken at or near the site of the original fracture, then restored to its correct anatomical alignment. Depending on the location and severity of the fracture, the bone may be held in position while it heals with either internal or external fixation:
- Internal fixation. The doctor attaches plates and screws to the outside of the bone or places a rod down the center of the bone.
- External fixation. A metal frame is positioned on the outside of the leg and attached to the bone with pins and wires.
Together, you and your doctor will determine the best option for you.
Distraction osteogenesis. If the malunion involves shortening of the bone and a significant leg length discrepancy, your doctor may talk with you about the possibility of lengthening the limb using internal lengthening rods or an external frame. This procedure, called distraction osteogenesis, will equalize limb length over time and eliminate the limp caused by a short leg.
Pain management. After surgery, you will feel some pain, but your surgeon and nurses will make every effort to help you feel as comfortable as possible.
Many types of pain medication are available to help control pain, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs) and local anesthetics. Treating pain with medications can help you feel more comfortable, which will help your body heal faster and recover from surgery faster.
Opioids can provide excellent pain relief, however, they are a narcotic and can be addictive. It is important to use opioids only as directed by your doctor. You should stop taking these medications as soon as your pain starts to improve.
Complications. There are risks associated with any type of surgery. These include:
- Infection
- Bleeding
- Problems with wound healing
- Pain
- Blood clots
- Damage to blood vessels or nerves
- Reaction to anesthesia
Before your surgery, your doctor will discuss each of the risks with you and will take specific measures to avoid complications.
Recovery
After surgery, your leg may need to be immobilized in a cast or splint for a period of time. Depending on the specific procedure performed, you may also need to avoid weight bearing while your bones heal and get strong. Physical therapy will help you regain muscle strength, range of motion and walking ability and is often required for several weeks.
During follow-up visits with your doctor, you will have x-rays to check the healing process and alignment of the bone.
For more information about treatment for malunions, please visit the Limb Lengthening and Reconstruction Society.
The Limb Lengthening and Reconstruction Society strives to maintain the highest competency in the field of musculoskeletal deficiencies and reconstruction, including limb length and extremity defects, long bone and growth deformity, limb salvage, trauma and complex limb reconstruction.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.