Diseases & Conditions
Cervical Radiculopathy (Pinched Nerve)
Cervical radiculopathy, commonly called a "pinched nerve," occurs when a nerve in the neck is compressed or irritated where it branches away from the spinal cord. This may cause pain that radiates into the shoulder and/or arm, as well as muscle weakness and numbness.
- Cervical radiculopathy is often caused by degenerative ("wear-and-tear") changes — such as arthritis — that occur in the spine as we age.
- In younger people, it is most often caused by a sudden injury that results in a herniated disk. In some cases, however, there is no traumatic episode associated with the start of symptoms.
In most cases, cervical radiculopathy responds well to conservative treatment, including medication and physical therapy, and does not require surgery.
Anatomy
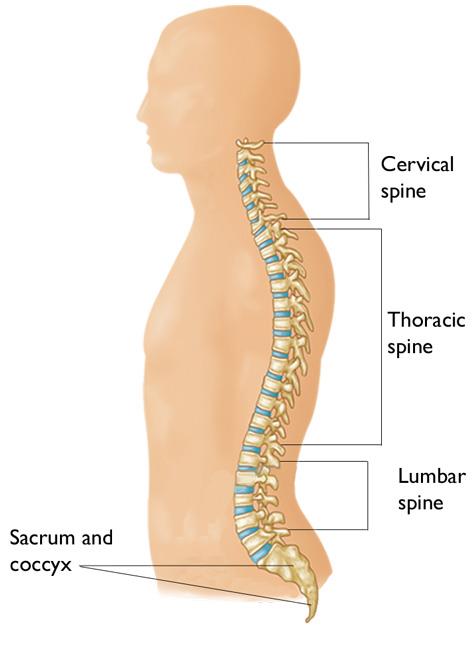
The spine is made up of 24 bones, called vertebrae, that are stacked on top of one another. These bones connect to create a canal that protects the spinal cord.
The seven small vertebrae that begin at the base of the skull and form the neck comprise (make up) the cervical spine.
Other parts of the spine include:
Spinal cord and nerves. These "electrical cables" travel through the spinal canal carrying messages between your brain and muscles. Nerve roots branch out from the spinal cord through openings (called foramen) in the sides of the spinal vertebrae.
Intervertebral disks. In between the vertebrae are flexible intervertebral disks. These act as shock absorbers when you walk or run, like the meniscus in the knee.
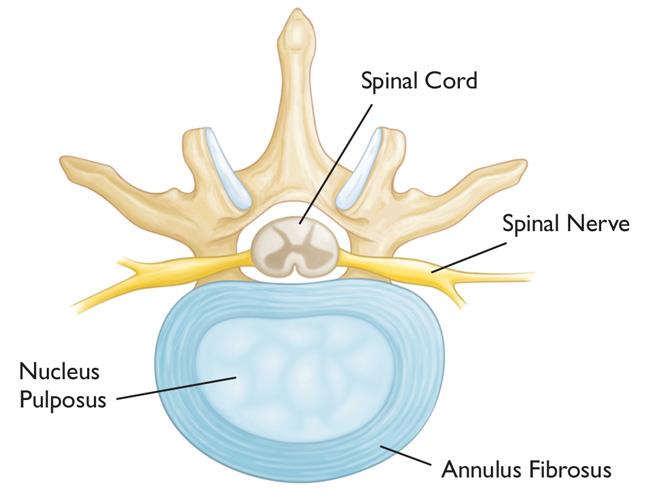
Intervertebral disks are flat and round and about 1/2-inch thick. They are made up of two components:
- Annulus fibrosus. This is the tough, flexible outer ring of the disk.
- Nucleus pulposus. This is the soft, jelly-like center of the disk.
Cause
Cervical radiculopathy most often arises from degenerative changes that occur in the spine as we age or from an injury that causes a herniated, or bulging, intervertebral disk.
Degenerative Changes
- As the disks in the spine age, they lose height and begin to bulge. They also lose water content, begin to dry out, and become stiffer. This problem causes settling, or collapse, of the disk spaces and loss of disk space height.
- As the disks lose height, the vertebrae move closer together.
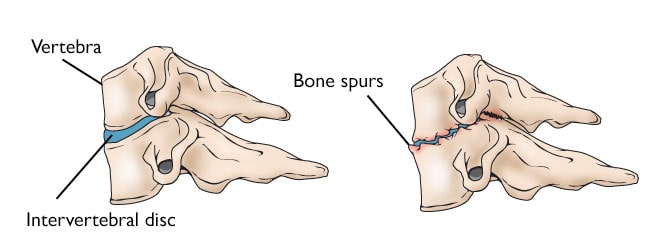
- The body responds to the collapsed disk by forming more bone — called bone spurs — around the disk to strengthen it.
- These bone spurs contribute to the stiffening of the spine. They may also narrow the foramen — the small openings on each side of the spinal column where the nerve roots exit — and pinch the nerve root.
Degenerative changes in the disks are often called arthritis or spondylosis. These changes are normal, and they occur in everyone. Nearly half of all people middle-aged and older have worn disks and pinched nerves that do not cause painful symptoms. It is not known why some people develop symptoms and others do not.
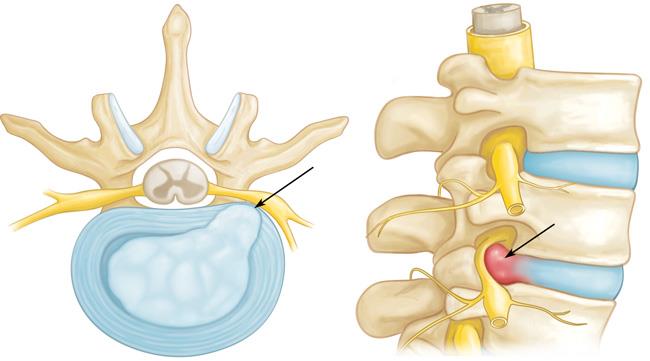
Herniated Disk
- A disk herniates when its jelly-like center (nucleus) pushes against its outer ring (annulus).
- If the disk is very worn or injured, the nucleus may squeeze all the way through.
- When the herniated disk bulges out toward the spinal canal, it puts pressure on the sensitive nerve root, causing pain and weakness in the area the nerve supplies.
A herniated disk often occurs with lifting, pulling, bending, or twisting movements.
Symptoms
In most cases, the pain of cervical radiculopathy starts at the neck and travels down the arm in the area served by the damaged nerve. This pain is usually described as burning or sharp, also known as neuropathic pain. Certain neck movements — like extending or straining the neck or turning the head — may increase the pain. Other symptoms include:
- Tingling or the feeling of "pins and needles" in the fingers or hand, also known as paresthesia
- Weakness in the muscles of the arm, shoulder, or hand
- Loss of sensation or numbness
Some patients report that pain decreases when they place their hands on top of their head (this is called abduction relief). This movement may temporarily relieve pressure on the nerve root.
Doctor Examination
Physical Examination
After discussing your medical history and general health, your doctor will:
- Ask you about your symptoms
- Examine your neck, shoulder, arms and hands — looking for muscle weakness, loss of sensation, or any change in your reflexes
- Possibly ask you to perform certain neck and arm movements to try to re-create and/or relieve your symptoms
Tests
X-rays. X-rays provide images of dense structures, such as bone. An X-ray will show the alignment of bones along your neck. It can also reveal whether there is any narrowing of the foramen and damage to the disks.
Computerized tomography (CT) scans. More detailed than a plain X-ray, a CT scan can help your doctor determine whether you have developed bone spurs near the foramen in your cervical spine.
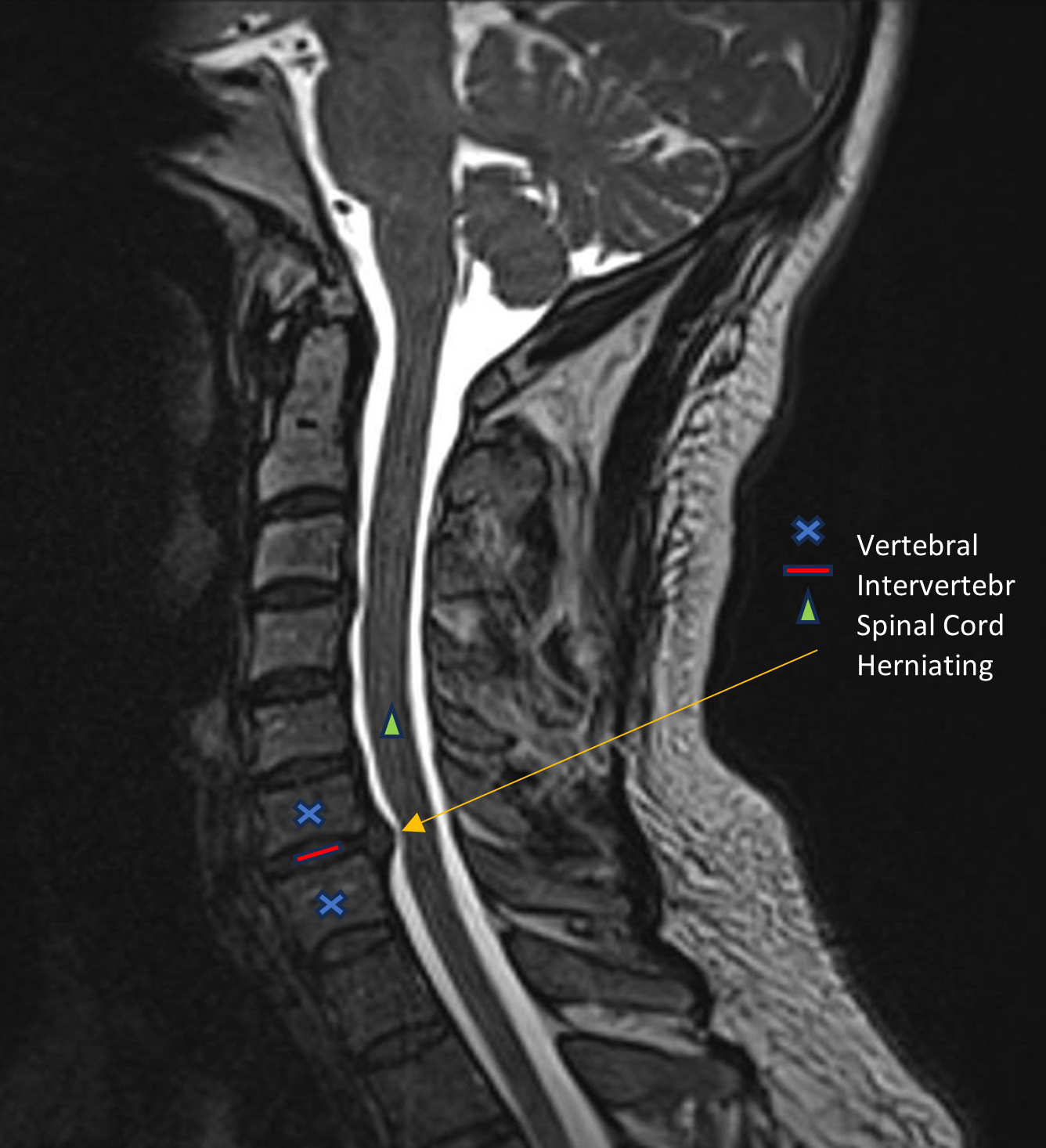
Magnetic resonance imaging (MRI) scans. MRI scans create better images of the body's soft tissues, such as muscle, fat, blood vessels, nerves, and fluids. An MRI of the neck can show if your nerve compression is caused by damage to soft tissues — such as a bulging or herniated disk. It can also help your doctor determine whether there is any damage to your spinal cord or nerve roots.
Learn more: X-Rays, CT Scans, and MRIs
Electromyography (EMG). Electromyography measures the electrical impulses of the muscles at rest and during contractions. Nerve conduction studies are often done along with EMG to determine if a nerve is functioning normally. Together, these electrodiagnostic tests can help your doctor determine whether your symptoms are caused by pressure on spinal nerve roots. Nerve roots can also be compressed elsewhere (such as around the elbow or wrist) or damaged for other reasons. These studies help distinguish between cervical radiculopathy and other common diseases.
Treatment
It is important to note that the majority of patients with cervical radiculopathy get better over time and do not need treatment. For some patients, the pain goes away relatively quickly — in days or weeks. For others, it may take longer.
It is also common for cervical radiculopathy that has improved to return at some point in the future. Even when this occurs, it usually gets better without any specific treatment.
In some cases, however, cervical radiculopathy does not improve. These patients require evaluation and treatment.
Nonsurgical Treatment
Initial treatment for cervical radiculopathy is nonsurgical. Nonsurgical treatment options include:
Soft cervical collar. This is a padded ring that wraps around the neck and is held in place with Velcro. Your doctor may advise you to wear a soft cervical collar to allow the muscles in your neck to rest and to limit neck motion. This can help decrease the pinching of the nerve roots that happens when you move your neck. A soft collar should only be worn for a short period of time, since long-term wear may decrease the strength of the muscles in your neck.
Physical therapy. Specific exercises can help relieve pain, strengthen neck muscles, and improve range of motion. In some cases, traction, or pulling in line with the spine, can be used to gently stretch the joints and muscles of the neck.
Medications. In some cases, medications can help improve your symptoms.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). NSAIDs, including aspirin, ibuprofen, and naproxen, may provide relief if your pain is caused by nerve irritation or inflammation.
- Oral corticosteroids. A short course of oral corticosteroids may help relieve pain by reducing swelling and inflammation around the nerve.
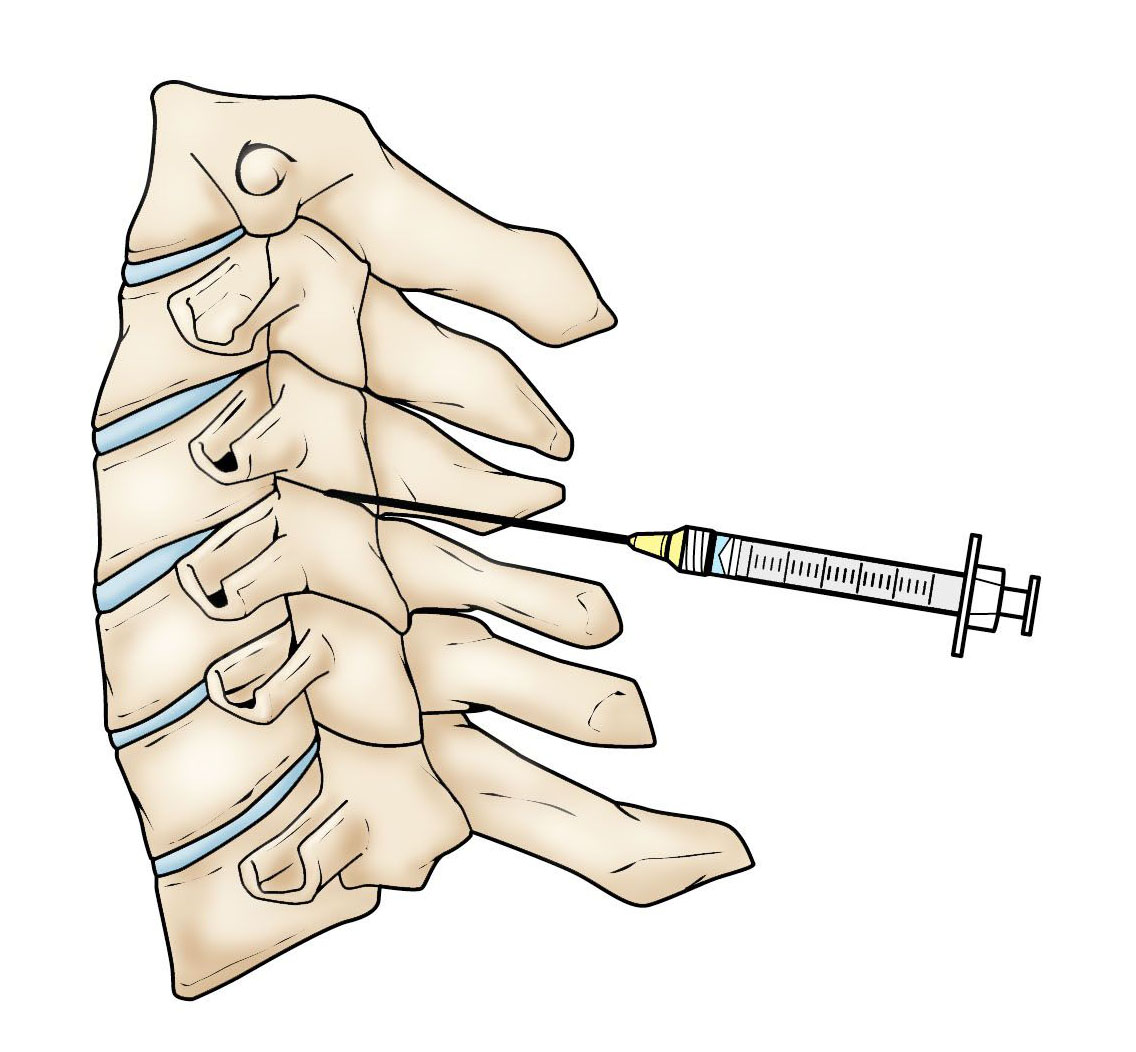
Steroid injection. In this procedure, steroids are injected near the affected nerve to reduce a specific area of inflammation. It can be placed
- Between the laminae (epidural injection)
- In the foramen (selective nerve injection)
- Into the facet joint
Although steroid injections do not relieve the structural pressure on the nerve caused by a narrow foramen or herniated disk, they may lessen the swelling and relieve the pain long enough to allow the nerve to recover.
Narcotics. These medications are reserved for patients with severe pain that is not relieved by other options. Narcotics, like opioids, are usually prescribed for a limited time only, as they have side effects and can be highly addictive. It is important to use narcotic medications only as directed by your doctor and to stop using them as soon as your pain begins to improve.
Surgical Treatment
If, after a period of time, nonsurgical treatment does not relieve your symptoms, your doctor may recommend surgery.
There are several surgical procedures to treat cervical radiculopathy. The procedure your doctor recommends will depend on many factors, including which symptoms you are experiencing and the location of the involved nerve root.
Learn more about surgery for radiculopathy: Cervical Radiculopathy: Surgical Treatment Options
Cervical Radiculopathy "Mimickers"
Sometimes, other diseases can cause similar symptoms to cervical radiculopathy. Making the correct diagnosis can be complicated. Your symptoms and your doctor's physical exam and tests are used to help your doctor determine exactly where your pain is coming from.
These are some other diseases that can cause neck or arm pain that may mimic cervical radiculopathy:
- Some shoulder conditions, including:
- AC joint arthritis
- Scapular dyskinesis
- Thoracic outlet syndrome
- SC joint arthritis
- Suprascapular nerve compression
- Heart disease
- Inflammation at the elbow
- Nerve impingement at other places outside of the spine like the elbow (ulnar nerve entrapment at the elbow, or cubital tunnel syndrome) or wrist (ulnar tunnel syndrome of the wrist; carpal tunnel syndrome)
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.