Diseases & Conditions
Bowed Legs (Genu Varum, Blount's Disease)
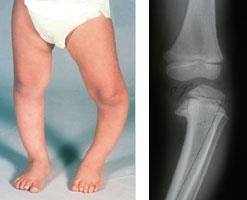
Bowed legs in a toddler are very common and a normal part of development in the majority of cases.
When a child with bowed legs stands with their feet together, there is a distinct space between the lower legs and knees. This may be a result of either one, or both, of the legs curving outward. Walking often exaggerates this bowed appearance.
In most cases, bowed legs will naturally begin to straighten as the child grows. If bowed legs have not gone away by the age of 3 years, there may be an underlying cause, such as infantile Blount's disease or rickets.
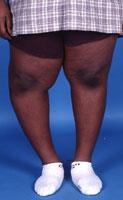
Adolescents (generally, ages 11 to 21 years) occasionally have bowed legs. This may be due to adolescent Blount's disease. In many of these cases, the child is significantly overweight.
Cause
Physiologic Genu Varum
In most children under 2 years old, bowing of the legs is simply a normal variation in leg appearance. Doctors refer to this type of bowing as physiologic genu varum.
In children with physiologic genu varum, the bowing begins to slowly improve at approximately 18 months of age and continues as the child grows. By ages 3 to 4 years, the bowing has corrected, and the legs typically have a normal appearance.
Blount's Disease
Blount's disease is a condition that can occur in toddlers and adolescents. It results from an abnormality of the growth plate in the upper part of the tibia (shinbone). Growth plates are located at the ends of a child's long bones. They help determine the length and shape of the adult bone.
In a child under the age of 2 years, it may be impossible to distinguish infantile Blount's disease from physiologic genu varum. By the age of 3 years, however, the bowing will worsen in a patient with Blount's disease, and an obvious problem can often be seen on an X-ray.
Rickets
Rickets is a bone disease in children that causes bowed legs and other bone deformities. Children with rickets do not get enough calcium, phosphorus, or Vitamin D — all of which are important for healthy growing bones.
Nutritional rickets is unusual in developed countries because many foods, including milk products, are fortified with Vitamin D.
- When nutritional rickets does occur, it is often in children who are exclusively breastfed.
- Rickets can also be caused by a genetic abnormality that does not allow Vitamin D to be absorbed correctly. This form of rickets may be inherited.
Symptoms
Bowed legs are most evident when a child stands and walks.
- The most common symptom of bowed legs is an awkward walking pattern.
- Toddlers with bowed legs usually have normal coordination and are not delayed in learning how to walk. The amount of bowing can be significant, however, and can be quite alarming to parents and family members.
- Turning in of the feet (intoeing) is also common in toddlers and frequently occurs in combination with bowed legs.
- Bowed legs do not typically cause any pain in the younger child.
- During adolescence, persistent bowing can lead to discomfort in the hips, knees, and/or ankles because of the abnormal stress that the curved legs have on these joints. In addition, parents are often concerned that the child trips too frequently, particularly if intoeing is also present.
Doctor Examination
Your child's doctor will begin your child's evaluation with a thorough physical examination.
- If your child is under 2 years of age, in good health, and has symmetrical bowing (the same amount of bowing in both legs), your doctor will most likely recommend observation, and follow-up with the doctor before the age of 3 years. In some cases, the doctor may recommend an X-ray of the lower legs. An X-ray of your child's legs in the standing position can show Blount's disease or rickets.
- If your child is older than 2 1/2 years at the first doctor's visit and has symmetrical bowing, the doctor will most likely recommend an X-ray. The likelihood of your child having infantile Blount's disease or rickets is greater at this age. If the X-ray shows signs of rickets, the doctor will order blood tests to confirm the presence of this disorder.
Treatment
Natural Progression of Disease
Physiologic genu varum almost always spontaneously — naturally — corrects itself as the child grows. This correction usually occurs by the age of 3 years.
Untreated infantile Blount's disease or untreated rickets results in progressive worsening of the bowing in later childhood and adolescence. Ultimately, these children have leg discomfort (especially the knees) due to the abnormal stresses that occur on the joints. Adolescents with Blount's disease are most likely to experience pain resulting from the bowing.
Nonsurgical Treatment
Physiologic genu varum. Although physiologic genu varum does not require active treatment, your child's doctor may want to examine your child periodically to ensure that the bowing goes away.
Blount's disease. Treatment may include bracing, surgery, or both. Toddlers may benefit from bracing, but bracing is not effective for adolescents with Blount’s disease.
Rickets. If your child has rickets, the doctor will likely refer your child to a metabolic specialist for medical management, in addition to regular orthopaedic follow-up. The effects of rickets can often be controlled with medication.
Surgical Treatment
Physiologic genu varum. In rare instances, physiologic genu varum in a toddler will not completely go away, and during adolescence, the bowing may cause the child and family to have cosmetic concerns. If the deformity is severe enough, your child may need a surgical procedure called "guided growth" to correct the remaining bowing.
Blount's disease. If bowing continues to progress (worsen) in a child with infantile Blount's disease despite the use of a brace, the child will need surgery by the age of 4 years. Surgery may stop further worsening and prevent permanent damage to the growth area of the shinbone.
Older children with bowed legs due to adolescent Blount's disease require surgery to correct the problem.
Rickets. Surgery may also be needed for children with rickets whose deformities persist despite proper management with medications.
Surgical procedures. There are different procedures to correct bowed legs, and they fall into two main types.
- Guided growth. This is the most common type of surgery performed for this condition. Using a small metal plate or staple, growth is temporarily stopped on the top of the shinbone in the healthy leg. This gives the abnormal side a chance to catch up, straightening the leg with the child's natural growth. Once the alignment is improved, the plate or staple is removed, and growth resumes.
- Tibial osteotomy. In this procedure, the shinbone is cut just below the knee and reshaped to correct the alignment. The bone is held in place while it heals with either an internal plate and screws, or an external frame that is positioned on the outside of the leg. Learn more: Osteotomy of the Knee
After surgery, a cast may be applied in certain cases to protect the bone while it heals. Your child may need crutches for a few weeks, and the doctor may recommend physical therapy exercises to restore your child's strength and range of motion. The doctor will talk to you about full recovery time and when your child can return to regular activities.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.