Diseases & Conditions
Boutonnière Deformity
A boutonnière deformity can affect the index, middle, ring, and little fingers. It is often the result of an injury to the tendon that straightens the middle joint (the proximal interphalangeal, or PIP joint) of the finger. This can occur:
- Due to trauma, such as a laceration or a dislocation
- Because of damage to soft tissue caused by a rheumatologic condition such as rheumatoid arthritis
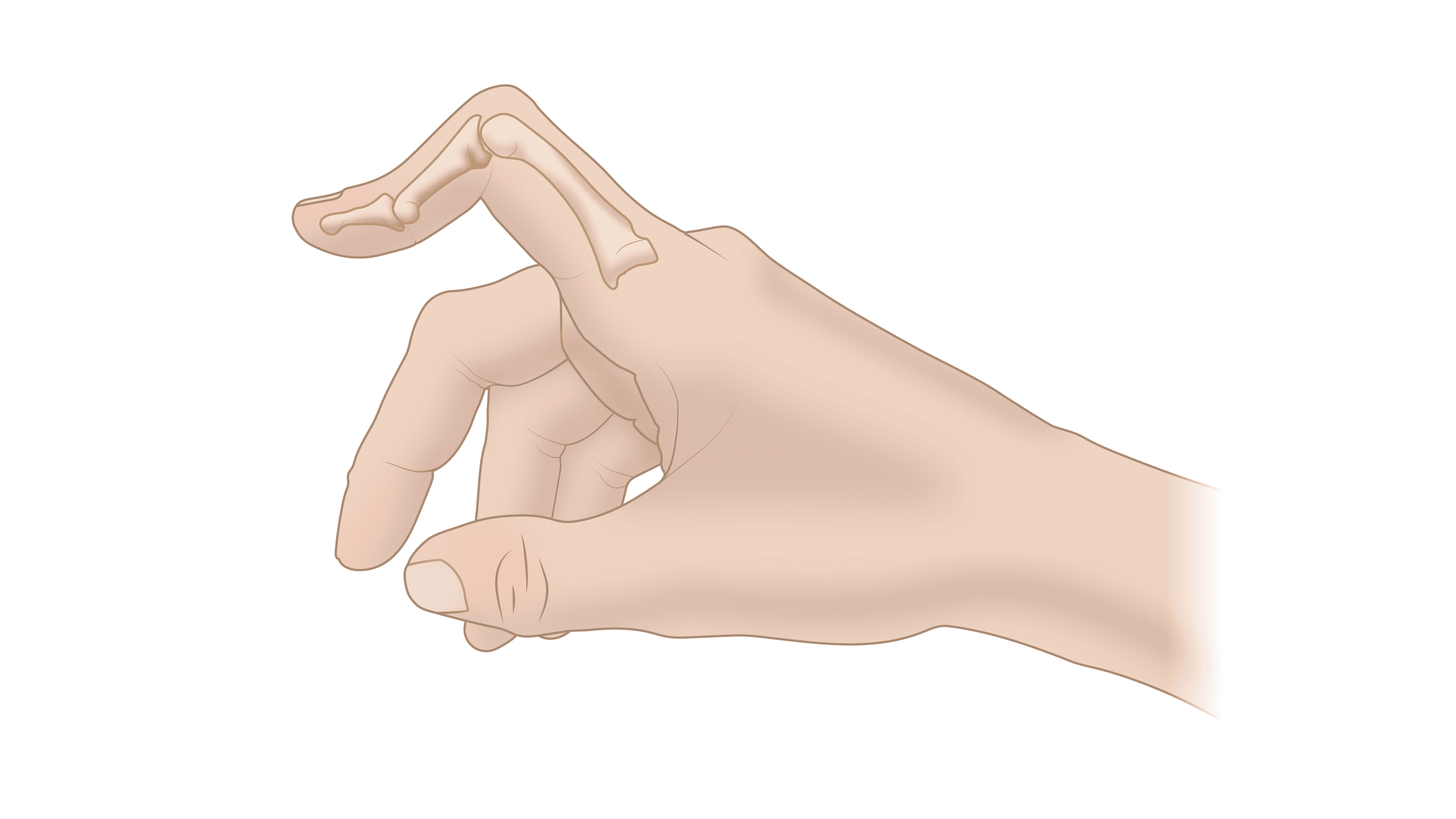
The result is that the middle joint (PIP joint) of the injured finger will not straighten and remains flexed, while the fingertip bends back (hyperextends).
- When treated promptly, traumatic boutonnière deformities can be reversed.
- Chronic boutonnière deformities and those caused by rheumatologic disease can worsen and eventually result in a permanent deformity and impaired functioning of the affected finger.
Anatomy
There are several tendons in your fingers that work together to bend and straighten the finger. These tendons run along the bottom, side, and top of the finger.
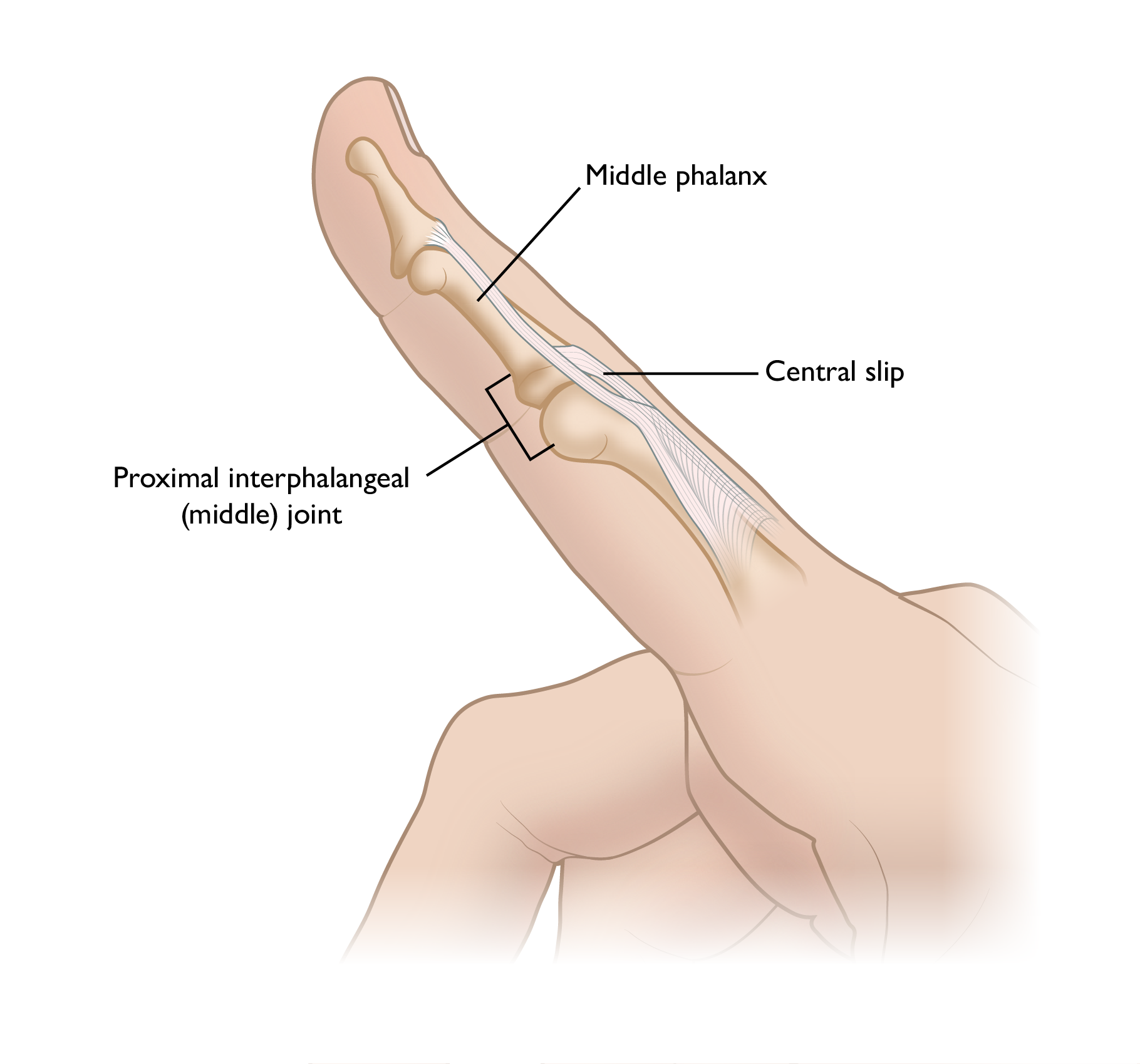
A major portion of the tendon on the top of the finger (the central slip) attaches to the middle bone of the finger (the middle phalanx) and acts on the finger to straighten the middle (PIP) joint.
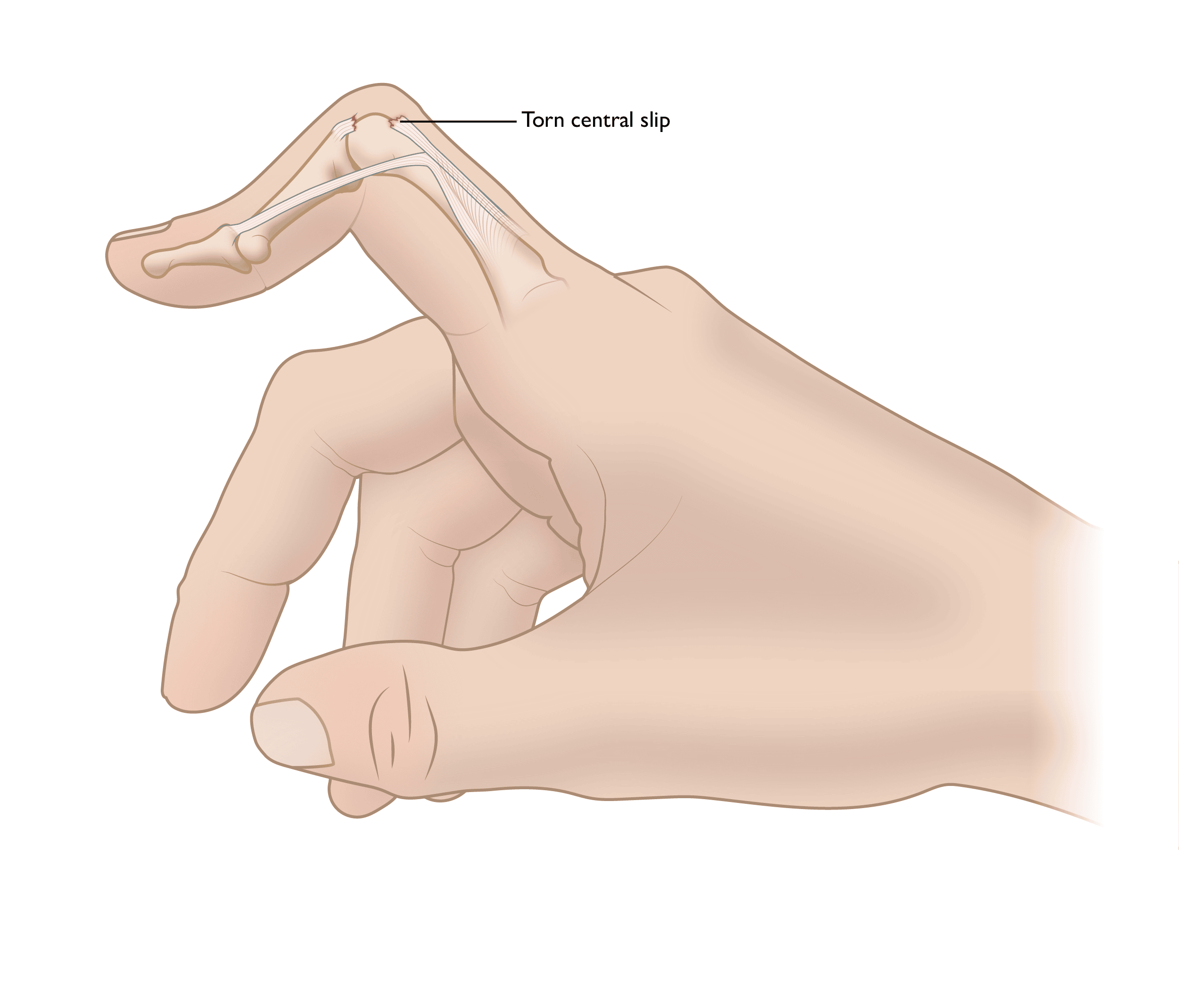
When the central slip tendon is injured or is destroyed by a rheumatologic condition:
- The finger is not able to be fully straightened, and the middle joint remains in a flexed position.
- Over time, the tendons on the side of the finger begin to slip toward the bottom of the finger, making this deformity worse.
- As a result of the imbalance in the finger, the last joint (distal interphalangeal, or DIP, joint) hyperextends.
- This then results in a boutonnière deformity of the affected finger.
Cause
Boutonnière deformity is generally caused by trauma. This could be:
- A forceful blow to the top (dorsal) side of a bent (flexed) middle joint of a finger, causing rupture of the central slip or fracture of the bone where the central slip connects to the middle bone of the finger (middle phalanx).
- A dislocation of the middle phalanx toward the bottom of the finger, causing the central slip to tear off of the bone.
Lacerations on the top of the finger can sever (cut) the central slip, causing the same effect. The tear looks like a buttonhole ("boutonnière" in French); hence, the name of the condition. In some cases, the bone can pop through the opening.
Boutonnière deformities may also be caused by arthritis, most commonly autoimmune arthritis (e.g., rheumatoid arthritis). These conditions destroy soft tissues and can weaken the central slip.
Symptoms
Signs of boutonnière deformity can develop immediately after an injury to the finger or may develop a week to 1 week to several weeks later.
- The finger at the middle (PIP) joint cannot be straightened and the fingertip cannot be bent, resulting in the distinctive deformity.
- Swelling and pain occur over the top of the PIP joint.
Doctor Examination
Because a boutonnière deformity is one of several injuries that result from a "jammed finger," you should consult a doctor for an appropriate diagnosis and treatment.
Your doctor will:
- Examine the fingers and hand.
- Ask you to straighten the affected finger and bend the fingertip.
- Possibly order X-rays may be recommended to detect any broken bones attached to the central slip of tendon.
- Possibly perform the Elson Test, which specifically detects central slip insufficiency. The test is performed by bending the PIP joint of the affected finger to 90°, then asking you to try to straighten it out against resistance. While doing this, the doctor will wiggle the tip of the finger to see if it moves easily. If it does not, this is a sign of a central slip injury, which means risk of a boutonnière deformity.
Treatment
Boutonnière deformity caused by a traumatic injury must be treated early to help you retain the full range of motion in the finger.
Nonsurgical Treatment
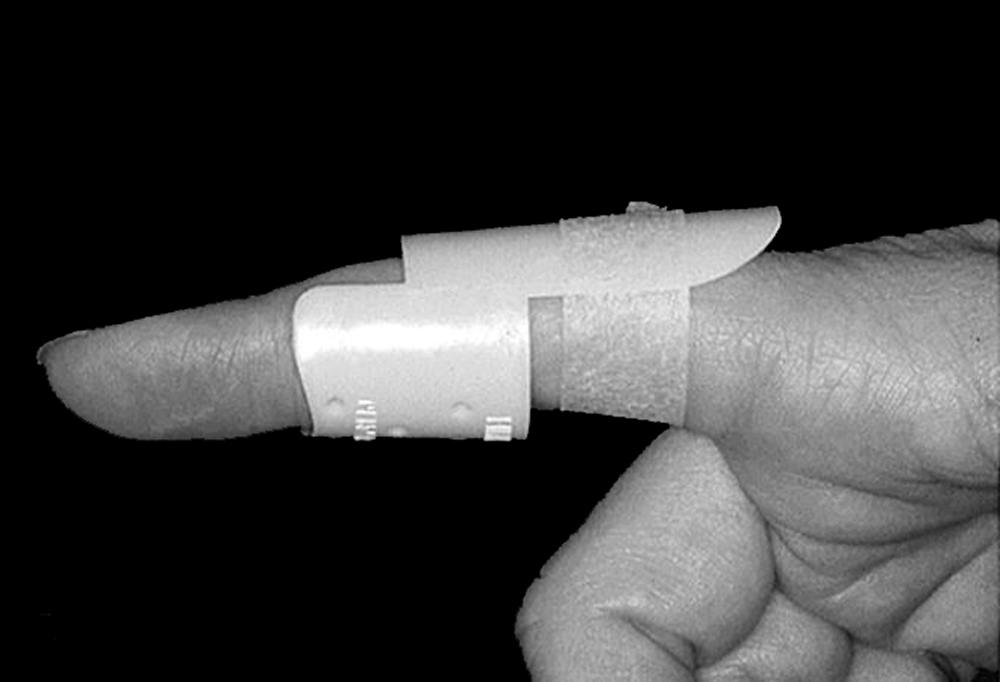
Nonsurgical treatment is usually preferred, and may include:- Splints. A splint will be applied to the finger at the middle joint to straighten it. This keeps the ends of the tendon from separating as it heals. It also allows the end joint of the finger to bend.
- While in the splint, it is important to work on bending the very tip of the finger to help keep the tendons of the finger gliding in the correct position.
- It is equally important to wear the splint continuously (nonstop) for the recommended length of time — usually 6 to 8 weeks. Allowing the finger to accidentally bend at the middle joint — while the finger is out of the splint — during the treatment period can reverse the progress you have made.
- After this period of immobilization ends, you may still have to wear the splint at night.
- Exercises. Your physician may recommend stretching exercises to improve the strength and flexibility in the fingers. While your finger is in the splint, exercises will focus on the DIP joint (the last joint of the finger), which must be bent throughout the day.
- Protection. If you participate in sports, you may have to wear protective splinting or taping for several weeks after the splint is removed.
People with boutonnière deformity caused by arthritis may be treated with oral medications or corticosteroid injections, as well as splinting.
Surgical Treatment
While nonsurgical treatment of boutonnière deformity is preferred, surgery is an option in certain cases, such as when:
- The deformity results from rheumatoid arthritis
- The tendon is severed (cut)
- A large bone fragment is displaced from (moved out of) its normal position
- The condition does not improve with splinting
Surgery can reduce pain and improve function, but it may not be able to fully correct the condition and make the finger look normal. If the boutonnière deformity remains untreated for more than 3 weeks, it becomes much more difficult to treat.
Surgery may include:
- Putting a dislocated PIP joint back in place and placing a temporary pin across the joint to keep it straight for 6 to 8 weeks
- Repairing an avulsed central slip (one that has become detached from the middle phalanx bone) by reattaching it a to the bone with an anchor
- Stitching together a lacerated (cut) central slip
- Fixing a broken of piece of the middle phalanx with the central slip attached to it using pins or plates/screws
- Creating a new central slip, using one of the tendon slips that flexes the PIP joint as a graft
- Releasing (disconnecting) the terminal tendon of the affected finger where it connects to last bone of the finger (distal phalanx) to help relief hyperextension of the DIP joint
Outcomes
Outcomes for management of boutonnière deformity vary depending on the treatment, time to treatment, and each person's unique anatomy and injury.
Early treatment works better, so if you believe you may have a finger injury, it is important to promptly schedule an appointment with a hand surgeon.
- Traumatic injuries treated either nonsurgically or surgically within 3 weeks of injury tend to do quite well.
- Chronic injuries and chronic deformities caused by rheumatologic conditions can be much harder to treat and have unpredictable outcomes.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.