Treatment
Osteotomy of the Knee
Osteotomy literally means "cutting of the bone." In a knee osteotomy, either the tibia (shinbone) or femur (thighbone) is cut and then reshaped to relieve pressure on one compartment of the knee joint.
Knee osteotomy is used when a patient has early-stage osteoarthritis that has damaged just one side of the knee joint. By shifting weight off of the damaged side of the joint, an osteotomy can relieve pain and significantly improve function in an arthritic knee.
Description
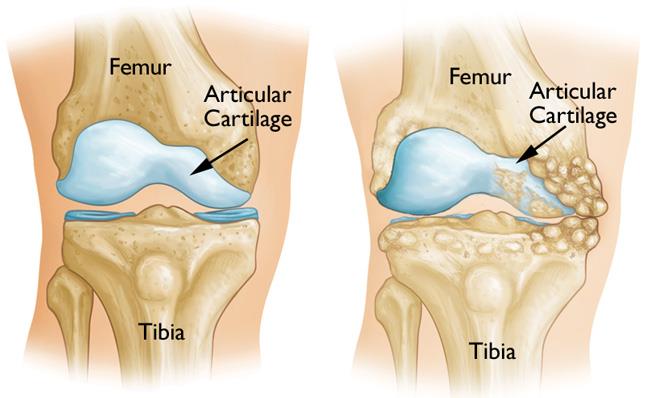
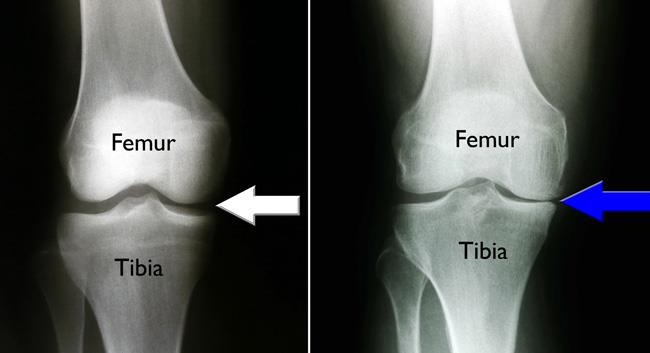
Osteoarthritis can develop when the bones of your knee and leg do not line up properly. This can put extra stress on either the inner (medial) or outer (lateral) side of your knee. Over time, this extra pressure can wear away the smooth articular cartilage that protects the bones, causing pain and stiffness in your knee.
Advantages and Disadvantages
Knee osteotomy has three goals:
- To transfer weight from the arthritic part of the knee to a healthier area
- To correct poor knee alignment
- To prolong the life span of the knee joint
Advantages of the procedure include the following:
- By preserving your own knee anatomy, a successful osteotomy may delay the need for a joint replacement for several years.
- There are no restrictions on physical activities after an osteotomy has healed — you will be able to participate in your favorite activities, even high-impact exercise.
Osteotomy does, however, have some disadvantages:
- Pain relief is not as predictable after osteotomy compared with a partial or total knee replacement.
- Recovery from osteotomy is typically longer and more difficult because you may not be able to bear weight on your operated knee right away. The osteotomy needs time to heal, which takes approximately 6 weeks.
- In some cases, having had an osteotomy can make later total knee replacement surgery more challenging.
Because results from partial knee replacement and total knee replacement have been so successful, knee osteotomy has become less common. Nevertheless, it remains an option for many patients.
Procedure
Most osteotomies for knee arthritis are done on the tibia (shinbone) to correct a bowlegged alignment that is putting too much stress on the inner (medial) compartment of the knee.
Tibial osteotomy was first performed in Europe in the late 1950s and brought to the United States in the 1960s. This procedure is sometimes called a high tibial osteotomy (HTO).
This procedure can be performed in two different ways:
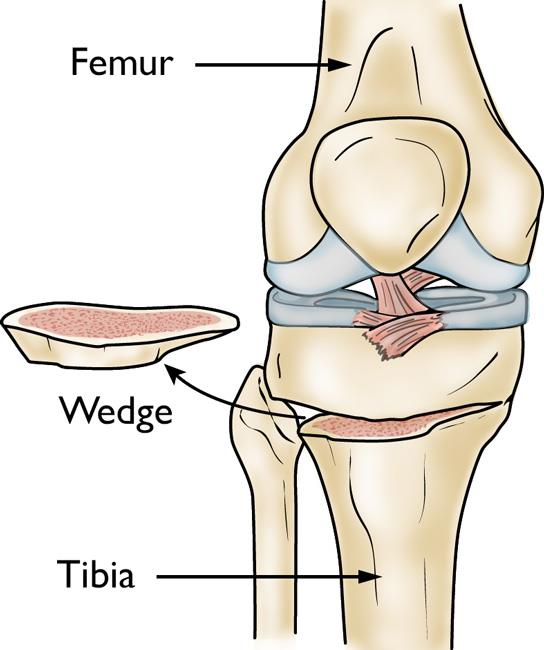
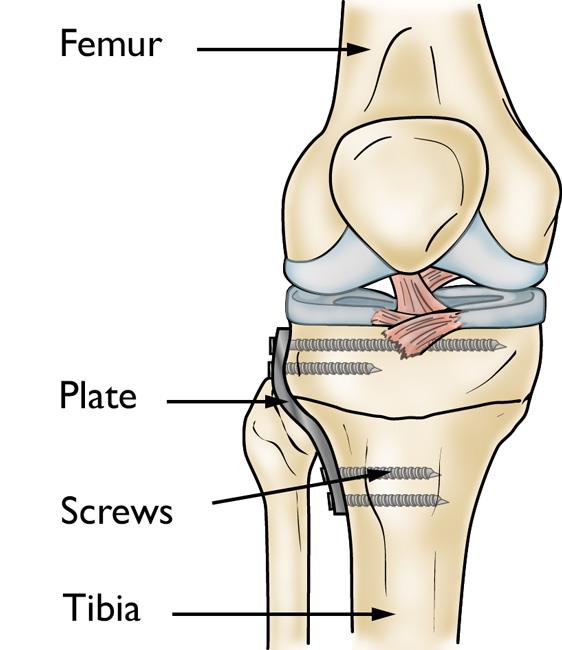
- A wedge of bone graft or synthetic bone is placed on the medial side of the tibia and secured with a plate and screws.
- A wedge of bone is removed from the outer (lateral) side of the tibia.
When the surgeon opens the medial wedge or closes the lateral wedge, it straightens the leg. This brings the bones on the healthy side of the knee closer together and creates more space between the bones on the damaged, arthritic side. As a result, the knee can carry weight more evenly, easing pressure on the painful side.
Osteotomies of the thighbone (femur) are done using the same technique. They are usually done to correct a knock-kneed alignment.
Your orthopaedic surgeon will discuss with you the technique they are going to use for your procedure.
Candidates for Knee Osteotomy
Knee osteotomy is most effective for thin, active patients who are under the age of 60. Good candidates have:
- Pain on only one side of the knee
- No pain under the kneecap.
- Knee pain that is brought on mostly by activity, or by standing for a long period of time.
Candidates should be able to fully straighten the knee and bend it at least 90° prior to surgery.
Patients with rheumatoid arthritis are not good candidates for an osteotomy. Your orthopaedic surgeon will help you determine whether a knee osteotomy is suited for you.
Your Surgery
Before Surgery
You will likely be admitted to the hospital on the day of surgery.
Before your procedure, a doctor from the anesthesia department will evaluate you. They will review your medical history and discuss anesthesia choices with you. Anesthesia can be either general (you are put to sleep) or spinal (you are awake, but your body is numb from the waist down).
Your surgeon will also see you before surgery and sign your knee with a marker to verify the surgical site.
Surgical Procedure
A knee osteotomy operation typically lasts between 1 and 2 hours.
- Your surgeon will make an incision at the front of your knee, starting below your kneecap.
- They will plan out the correct size of the wedge using guide wires.
- With an oscillating saw, your surgeon will cut along the guide wires, and then either place or remove a wedge of bone, depending on the technique used.
- Your surgeon will insert a plate and screws to hold the bones in place until the osteotomy heals.
After the surgery, you will be taken to the recovery room where you will be closely monitored as you recover from the anesthesia.
Complications
As with any surgical procedure, there are risks involved with osteotomy. Your surgeon will discuss each of the risks with you and will take specific measures to help avoid potential complications.
Although the risks are low, the most common complications include:
- Infection
- Blood clots
- Stiffness of the knee joint
- Injuries to vessels and nerves
- Failure of the osteotomy to heal
In some cases, a second surgery may be required, particularly if the osteotomy does not heal.
Recovery
Hospital discharge. In most cases, patients go home 1 to 2 days after an osteotomy.
Pain management. After surgery, you will feel some pain, but your surgeon and nurses will make every effort to help you feel as comfortable as possible.
Many types of pain medication are available to help control pain, including opioids, nonsteroidal anti-inflammatory drugs (NSAIDs) and local anesthetics. Treating pain with medications can help you feel more comfortable, which will help your body heal faster and recover from surgery faster.
Opioids can provide excellent pain relief, however, they are a narcotic and can be addictive. It is important to use opioids only as directed by your doctor and to stop taking them as soon as your pain starts to improve.
Weightbearing. After the operation, you will most likely need to use crutches for several weeks. Your surgeon may also put your knee in a brace or cast for protection while the bone heals. Your surgeon will give you instructions about when weight bearing can begin.
Doctor visit. You will see your surgeon for a follow-up visit after surgery. X-rays will be taken so that the surgeon can check how well the osteotomy has healed. After the follow-up, your surgeon will tell you when it is safe to put weight on your leg, and when you can start rehabilitation.
Rehabilitation exercises. During rehabilitation, a physical therapist will give you exercises to help maintain range of motion in your knee and restore your strength.
You may be able to resume your full activities 3 to 6 months after surgery.
Outcome
For most patients, osteotomy is successful in relieving pain and delaying the progression of arthritis in the knee. It can allow a younger patient to lead a more active lifestyle for many years. Even though many patients will ultimately require a total knee replacement, an osteotomy can be an effective way to delay the need for a replacement
Last Reviewed
May 2022
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.