Diseases & Conditions
Sprained Ankle
Ankle sprains are common injuries that occur among people of all ages and at all activity levels; in fact, they are the number one reason for missed participation in athletics.
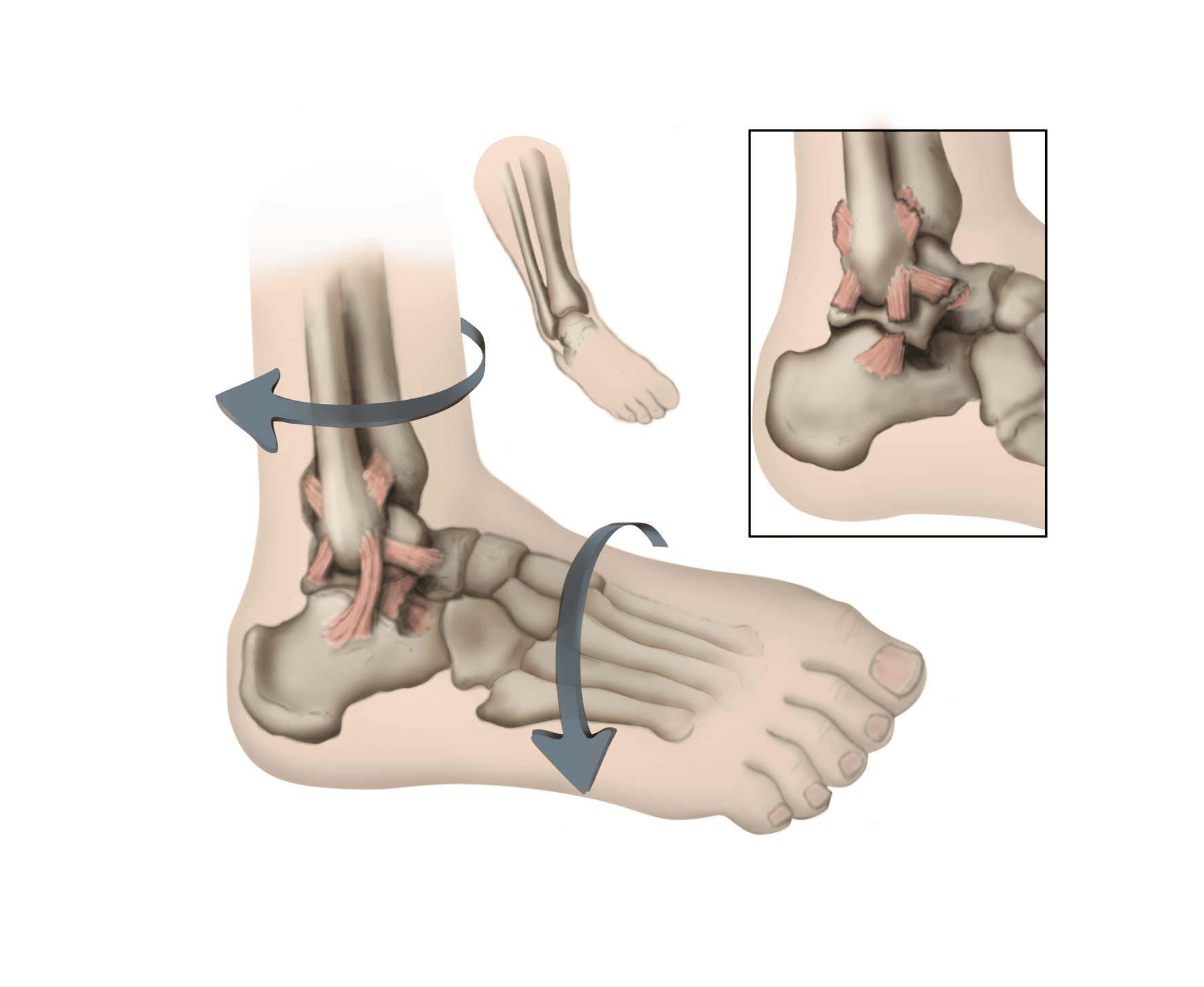
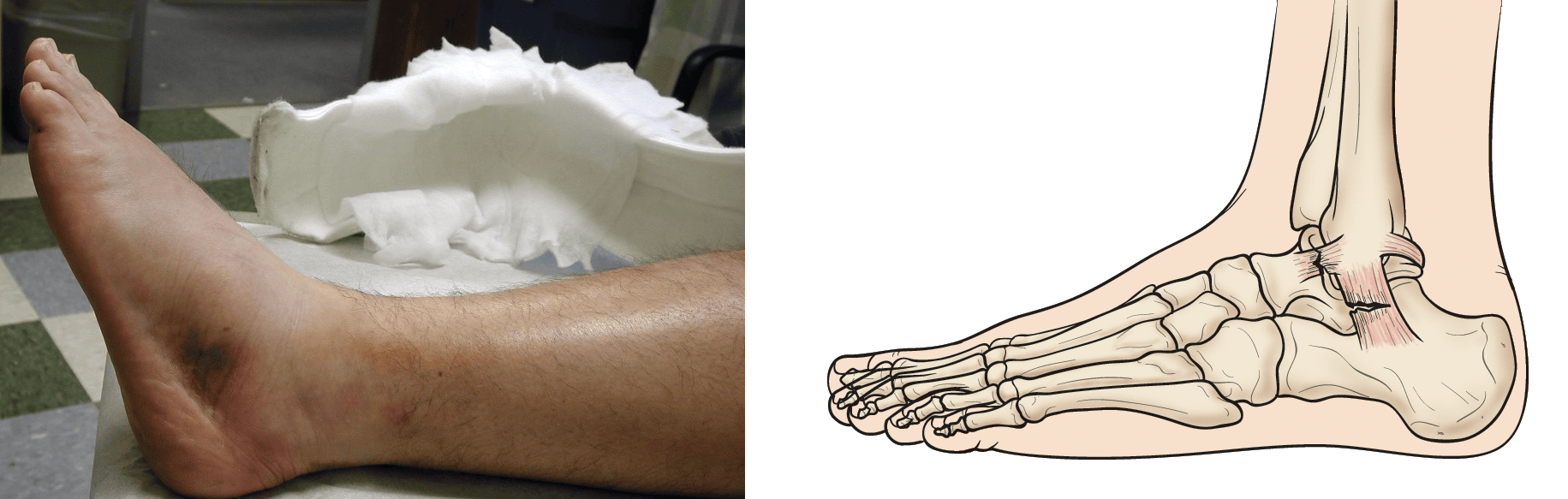
An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Often, this involves ligaments in the later side (outside) of the ankle. The severity of a sprain can vary greatly. It depends on the number of ligaments involved and how much the ligaments are torn.
Most sprains heal with conservative treatments like ice, elevation, over-the-counter medications, and simple rehabilitation exercises. However, you may need to be seen by a medical professional to make sure you do not have a severe sprain or fracture if:
- Your ankle remains swollen or painful for several weeks despite conservative treatments
- You have trouble putting weight on your ankle
If symptoms do not improve despite non-operative treatment, you may need surgery to repair or reconstruct the injured ligaments.
Without proper treatment and rehabilitation, a chronic or untreated severe sprain can weaken your ankle, making it more likely that you will injure it again. Repeated ankle sprains can lead to long-term problems, including chronic ankle pain, arthritis, and instability.
What Is an Ankle Sprain?
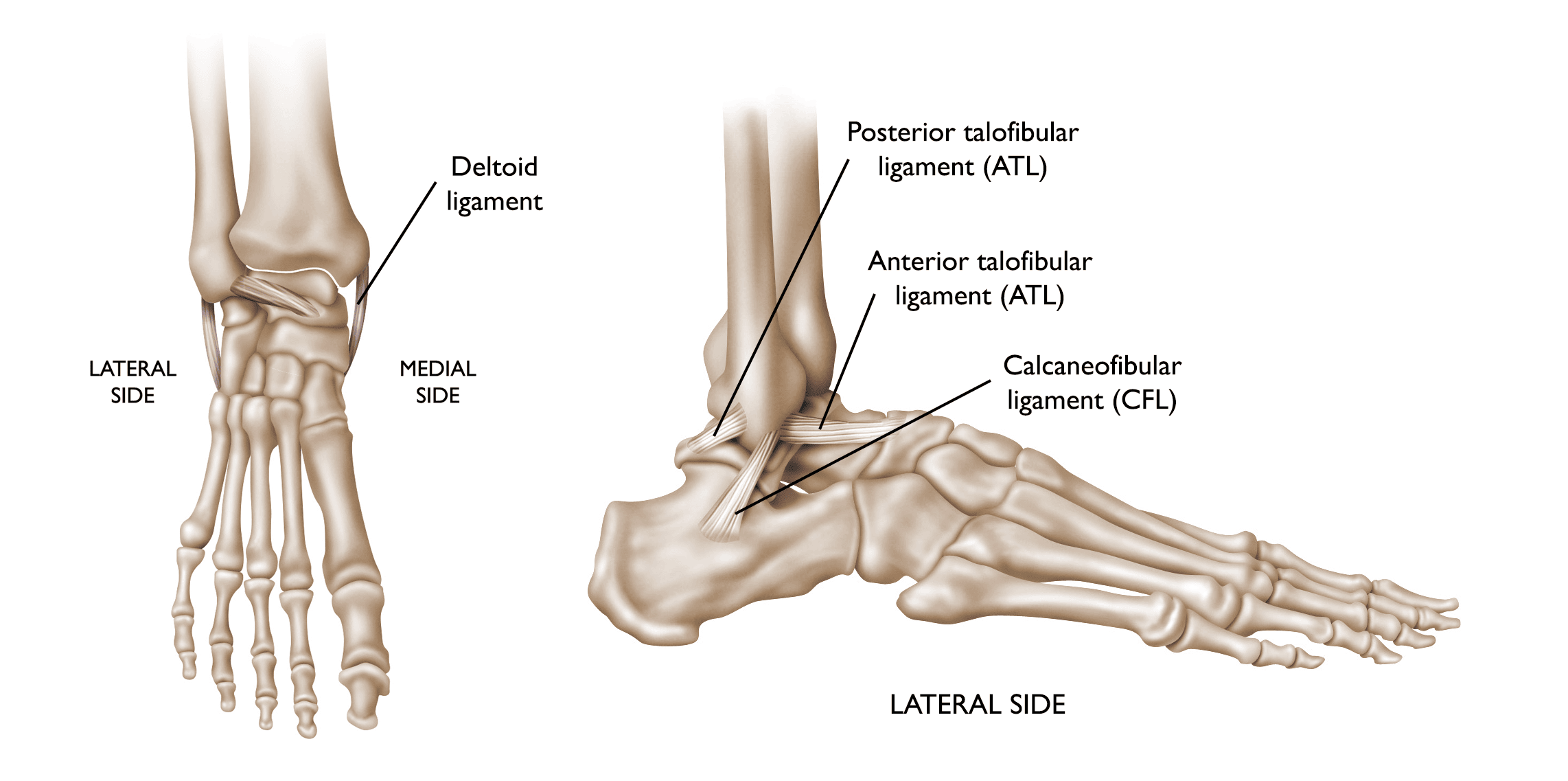
Ligaments are strong, fibrous tissues that connect bones to other bones throughout the body. There are many ligaments in the ankle that help to keep the bones in proper position and stabilize the joint. Joint stability is important for all types of activities, including standing, walking, and running.
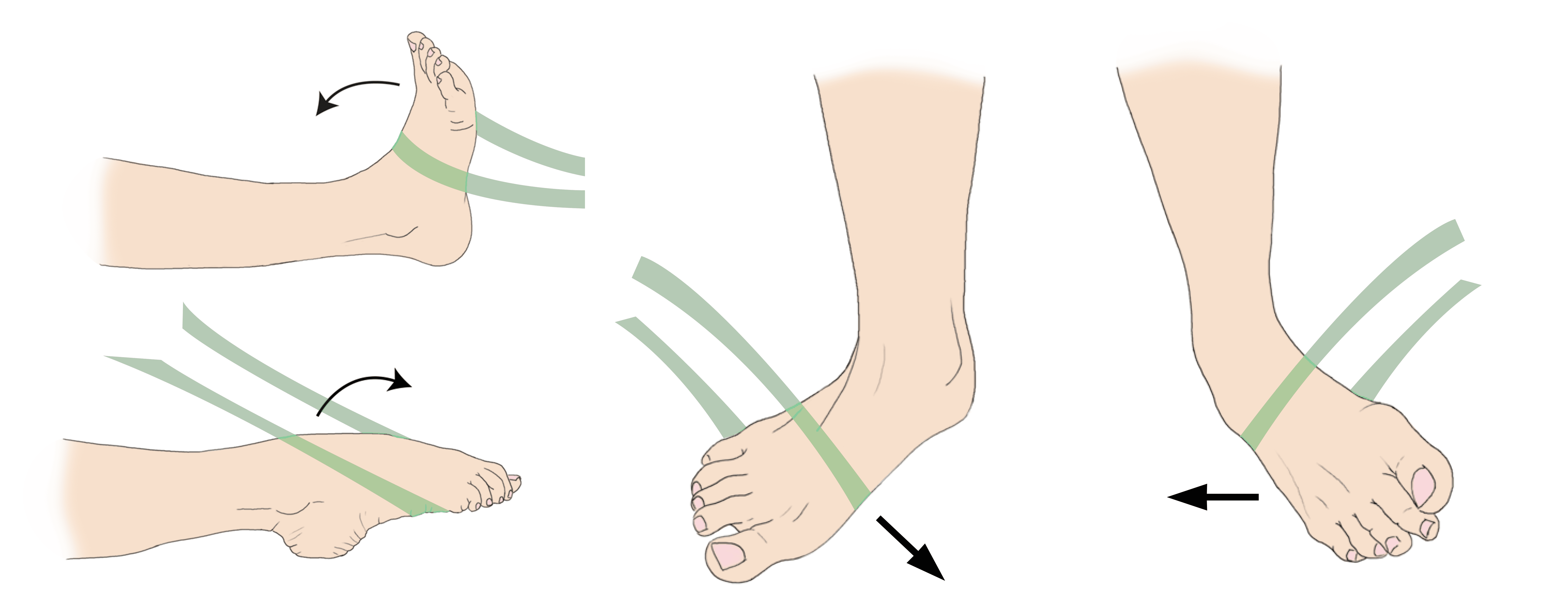
- Around 90% of ankle sprains involve an inversion injury (the foot turns inward) to the anterior talofibular (ATFL) and calcaneofibular (CFL) ligaments. The ATFL and CFL are the lateral ligaments, meaning they are on the outside of the ankle.
- The less common medial ankle sprain is caused by an eversion injury (the foot turns out) to the deltoid ligament on the inside of the ankle.
Sprains can range from tiny tears in the fibers that make up the ligament to complete tears.
If there is a complete tear of the ligaments, the ankle may become unstable after the initial injury phase passes. Over time, this instability can result in damage to the bones and cartilage, the smooth lining of the joint.
Causes of Ankle Sprains
Patients often experience a twisting injury to their foot or ankle. If there is severe tearing of the ligaments, you might also hear or feel a pop. Sprains may occur quickly and without warning during many different activities, such as:
- Walking, working, or exercising on an uneven surface
- Falling down or tripping
- Participating in high-risk sports that require cutting or jumping actions, such as trail running, basketball, tennis, football, and soccer
Risk factors for ankle sprains include:
- Poor balance
- Ligaments that are too loose or flexible
- Poor ankle alignment
- Wearing shoes that do not provide enough foot and ankle support
- Wearing shoes with slippery soles (bottoms)
- A previous ankle sprain, which increases the risk of a repeat sprain
Symptoms of an Ankle Sprain
The types and severity of symptoms for a sprained ankle vary widely depending on the degree of the injury. Symptoms may include:
- Pain, both at rest and with weightbearing or activity
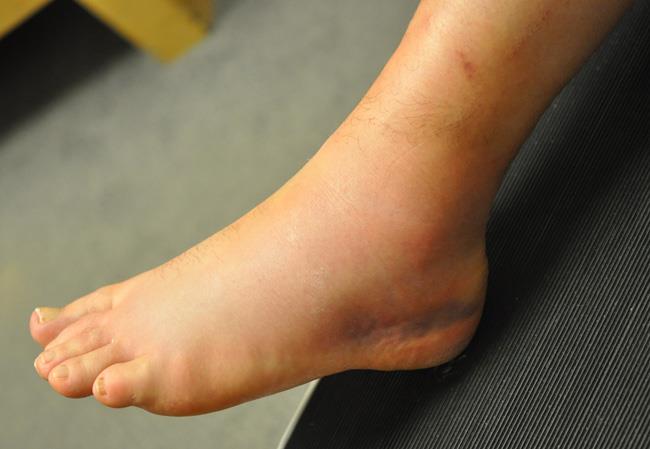
- Swelling
- Bruising
- Tenderness to touch
- Instability of the ankle, or a feeling that your ankle is giving out
Symptoms of a severe sprain are similar to those of a broken bone and require prompt medical evaluation.
Diagnosing an Ankle Sprain
Physical Examination
Your doctor will diagnose your ankle sprain by asking you questions about the injury and performing a careful examination of your foot and ankle. Due to the swelling and inflammation, this physical exam may be painful and often includes:
- Observation. Your doctor will look at the injured ankle and compare it to your other ankle. Often, the sprained ankle is swollen and bruised over the injured ligaments.
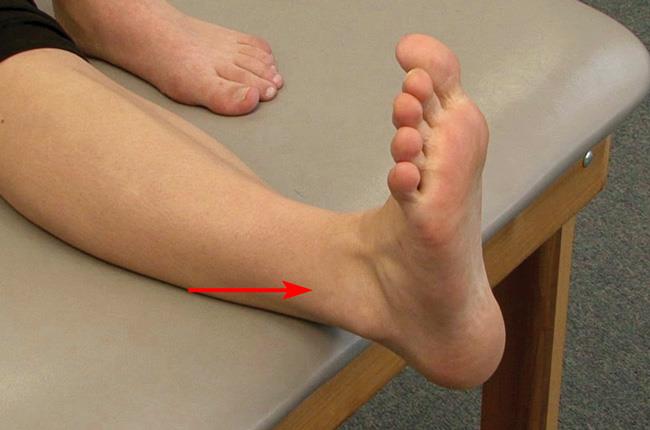
- Palpation. Tenderness is often limited to the area directly over the injured ligaments. Your doctor will gently press around the ankle to determine which ligaments are injured.
- Range of motion testing. The doctor may move your ankle in different directions; however, it may be difficult to move a stiff, swollen ankle.
- Stability testing. Your doctor may manipulate or pull your ankle in several directions in a controlled manner to check the stability of the ankle joint.
Your doctor may be able to tell how serious your ankle sprain is based on the amount of swelling, pain, bruising, and stability. If you have difficulty bearing weight, or tenderness in the bones of the foot and ankle, you may need more tests to rule out a fracture.
Imaging Tests
An ankle sprain is largely a clinical diagnosis based on how the injury happened, symptoms, and examination by a medical professional. Occasionally, a doctor will order imaging tests, such as X-rays and magnetic resonance imaging (MRI) scans, to rule out a fracture or other injury to the nearby tendons and cartilage.
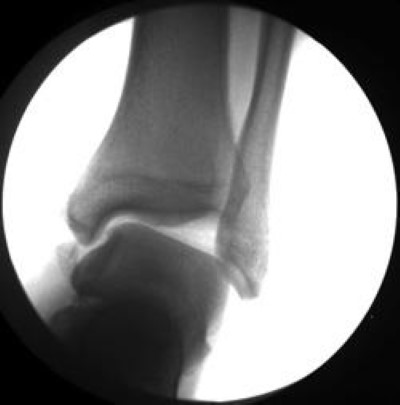
X-rays. X-rays provide images of dense structures, such as bone. Depending on your symptoms and examination, your doctor may order X-rays to evaluate the bones in your ankle and foot. Severe ankle sprains can have a similar degree of pain, bruising, and swelling as a fracture. This makes it hard to tell the difference between the two injuries.
Stress X-rays. In addition to plain X-rays, your doctor may also order stress X-rays. These images are taken while the ankle is being pushed in different directions in a controlled manner. Stress X-rays help to show whether the ankle is unstable because of injured ligaments.
Magnetic resonance imaging (MRI) scan. An MRI scan is not required to diagnose ankle sprains. However, your doctor may order an MRI:
- To evaluate other structures, such as ligaments, cartilage and tendons, around the ankle; X-rays will not show damage to these soft structures
- If you show signs of a high ankle sprain — an injury to the ligaments and structures connecting the bones of the lower leg (tibia and fibula)
- If your symptoms continue beyond 6 to 8 weeks after the injury despite conservative treatment
Classification of Ankle Sprains
After the examination, your doctor will determine the grade of your sprain to help develop a treatment plan. Sprains are graded based on how much damage there is to the ligaments.
Grade 1
- Slight stretching and microscopic tearing of the ligament fibers
- Mild tenderness, bruising, and swelling around the ankle
- Typically, no pain with weightbearing
- No instability on examination
Grade 2
- Partial tearing of the ligament
- Moderate tenderness, bruising, and swelling around the ankle
- Mild pain with weightbearing
- Slight instability, or ligament looseness, on examination compared to the uninjured ankle
Grade 3
- Complete tear of the ligament
- Significant tenderness, bruising, and swelling around the ankle
- Severe pain with weightbearing
- A lot of instability on examination
Treatment for Ankle Sprains
Nonsurgical Treatment
Nearly all isolated low ankle sprains can be treated without surgery. Even a complete ligament tear (Grade 3) will heal without surgical repair if it is immobilized (kept from moving) and rehabilitated appropriately.
A three-phase program guides treatment for all ankle sprains — from mild to severe:
Phase 1
- Includes a short period of immobilization, rest, and ice to reduce the swelling.
- Early weightbearing as tolerated is typically recommended during this phase.
- For a Grade 2 sprain, a removable plastic device, such as a walking boot or aircast brace, can provide support.
- Grade 3 sprains may require a short leg cast or cast-brace for 10 to 14 days.
- In most cases, swelling and pain will last 2 to 3 days. Walking may be difficult during this time, and your doctor may recommend that you use crutches as needed.
Phase 2
- Typically starts early and includes functional rehabilitation that focuses on:
- Range of motion exercises
- Isometric strengthening (contracting your muscles without moving the joints)
- Proprioception (balance) retraining exercises
- It is important to end ankle immobilization during this phase to avoid stiffness.
Phase 3
- Includes more advanced strengthening and proprioception exercises and the gradual return to pre-injury activities. This begins with activities that do not require turning or twisting the ankle. It is followed later by activities that require sharp, sudden turns (cutting activities), such as tennis, basketball, or football.
- Early return to sporting and work activities may require ankle taping or bracing.
This three-phase treatment program may take just 2 weeks to complete for minor sprains, or up to 6 to 12 weeks for more severe injuries.
Home Treatments for Ankle Sprains
For milder sprains, your doctor may recommend simple home treatment.
The rest, ice, compression, elevation, or RICE, protocol. Follow the RICE protocol as soon as possible after your injury:
- Rest your ankle by not walking on it or returning to sport.
- Apply ice immediately to keep the swelling down. Ice can be used for 20 to 30 minutes, 3 or 4 times daily. Do not apply ice directly to your skin. Instead, put the ice in an icepack or wrap it in a towel. Be sure to keep an eye on your skin when icing.
- Compression dressings, bandages, or ace-wraps will immobilize and support your injured ankle. Compression may also help with swelling. You can also wear compression garments as long as you are able to tolerate them.
- Elevate your ankle above the level of your heart as often as possible during the first 48 hours. Elevation also helps control and reduce the swelling.
Medication. Nonsteroidal anti-inflammatory drugs (NSAIDs) such as ibuprofen and naproxen can help control pain and swelling. Because they improve function by both reducing swelling and controlling pain, they are a better option for mild sprains than narcotic pain medicines.
If you cannot take NSAIDs, you can use acetaminophen (e.g., Tylenol) for pain relief.
Physical therapy. Rehabilitation exercises during phase 2 and 3 of recovery are used to improve flexibility, strength, and proprioception (balance).
- Early motion. To prevent stiffness, your doctor or physical therapist will provide you with exercises that involve range-of-motion or controlled movements of your ankle without resistance. Use of supportive stretching bands may also help with range of motion exercises.
- Strengthening exercises. Once the swelling and pain have improved, your doctor or physical therapist will start you on exercises to strengthen the dynamic stabilizers (muscles and tendons) in the front and back of your leg and ankle. Water exercises may be used if weightbearing strengthening exercises, such as toe-raising, are too painful. Exercises with resistance will be added as tolerated.
- Proprioception (balance) training. Poor balance often leads to repeat sprains and ankle instability. A good example of a balance exercise is standing on the affected foot with the opposite foot raised and your eyes closed. Balance boards are often used in this stage of rehabilitation.
- Endurance and agility exercises. Once you are pain-free, other exercises, such as agility drills, may be added gradually. Running in progressively smaller figure-8s is excellent for agility and calf and ankle strength. The goal is to increase strength and range of motion as your balance improves over time.
Surgery for Ankle Sprains
Surgical treatment of ankle sprains is rare.
- Surgery is reserved for injuries that do not respond to nonsurgical treatment, and for patients who continue to have ankle instability and pain after months of rehabilitation and nonsurgical treatment.
- Surgery may also be recommended for some high ankle sprains with instability of the ankle syndesmosis.
- Sometimes surgery is recommended if, in addition to a severe ankle sprain, you have other injuries (e.g., ankle cartilage injury or tendon rupture).
Types of surgery
Surgical options include:
- Arthroscopy. During arthroscopy, your doctor uses a small camera, called an arthroscope, to look inside your ankle joint. Miniature instruments are used to remove any loose pieces of bone or cartilage, or parts of the ligament that may be caught in the joint. Your surgeon may also be able to use an arthroscopic approach to repair ligaments by placing stitches through small incisions.
- Open repair/reconstruction. Your doctor may be able to repair the torn ligament with stitches or sutures by directly looking at the bone and other tissues in the ankle (an open surgical approach).
In other cases, the surgeon will reconstruct the damaged ligament by replacing it with a tissue graft. To make the graft, your surgeon will take a piece of another ligament and/or tendon from the foot and ankle area.
Recovery
Immobilization. There is typically a period of immobilization after surgery. A cast or protective boot is applied to protect the ligaments. Be sure to follow your doctor's instructions about how long to wear the protective device and how to protect the repair; early mobility or weightbearing can re-tear the repair or the reconstructed ligament.
Rehabilitation. The goal of rehabilitation after surgery is to restore strength, range of motion, and balance so you can return to pre-injury function. The length of time you can expect to spend recovering depends on the extent of injury and the type of surgery you had. Rehabilitation may take weeks to months.
Outcomes
Outcomes for ankle sprains are generally quite good. With proper treatment and rehabilitation, most patients are able to get back to their day-to-day activities after a period of time. Successful outcomes and return to activity depend on:
- The grade of the sprain.
- Whether there are other injuries. Additional injuries may impact the amount of time it takes you to heal and recover.
- The patient's commitment to rehabilitation exercises. Incomplete rehabilitation is the most common cause of chronic ankle instability after a sprain. If a patient stops doing the strengthening exercises, the injured ligament(s) will weaken and put the patient at risk for future ankle sprains.
It is important to discuss the likely outcome for your specific injury with your doctor.
Chronic Ankle Sprains
Once you have sprained your ankle, you may continue to sprain it if the ligaments do not have time to completely heal. This can happen if you return to work, sports, or other activities before your ankle heals and is rehabilitated.
It may be difficult to tell when the ligament is completely healed. Your symptoms (pain and swelling) can often guide how quickly you progress through physical therapy and regain function.
If pain continues for more than 4 to 6 weeks, you may have a chronic ankle sprain. Things that tend to make an already sprained ankle worse include:
- Stepping on uneven surfaces
- Participating in sports that require cutting actions, or rolling and twisting of the foot
Abnormal proprioception — a common complication of ankle sprains — can also lead to repeat sprains.
Reinjury may result in chronic instability, pain, and damage to the underlying cartilage and bones.
Preventing Ankle Sprains
The best way to prevent ankle sprains is to maintain good muscle strength, balance, and flexibility. The following precautions will help prevent sprains:
- Warm up thoroughly before exercise and physical activity.
- Perform strengthening exercises to enhance your ankle stability.
- Pay careful attention when walking, running, or working on an uneven surface.
- Choose footwear with appropriate support for your activity.
Reference
1. Trojian TH, McKeag DB. Single leg balance test to identify risk of ankle sprains. Br J Sports Med. 2006 Jul;40(7):610-3; discussion 613.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.