Diseases & Conditions
Shoulder Trauma (Fractures and Dislocations)
Trauma to the shoulder is common. Injuries range from a separated shoulder resulting from a fall onto the shoulder to fractures of the shoulder blade (scapula) or collarbone (clavicle) caused by a high-speed motor vehicle collision.
Anatomy
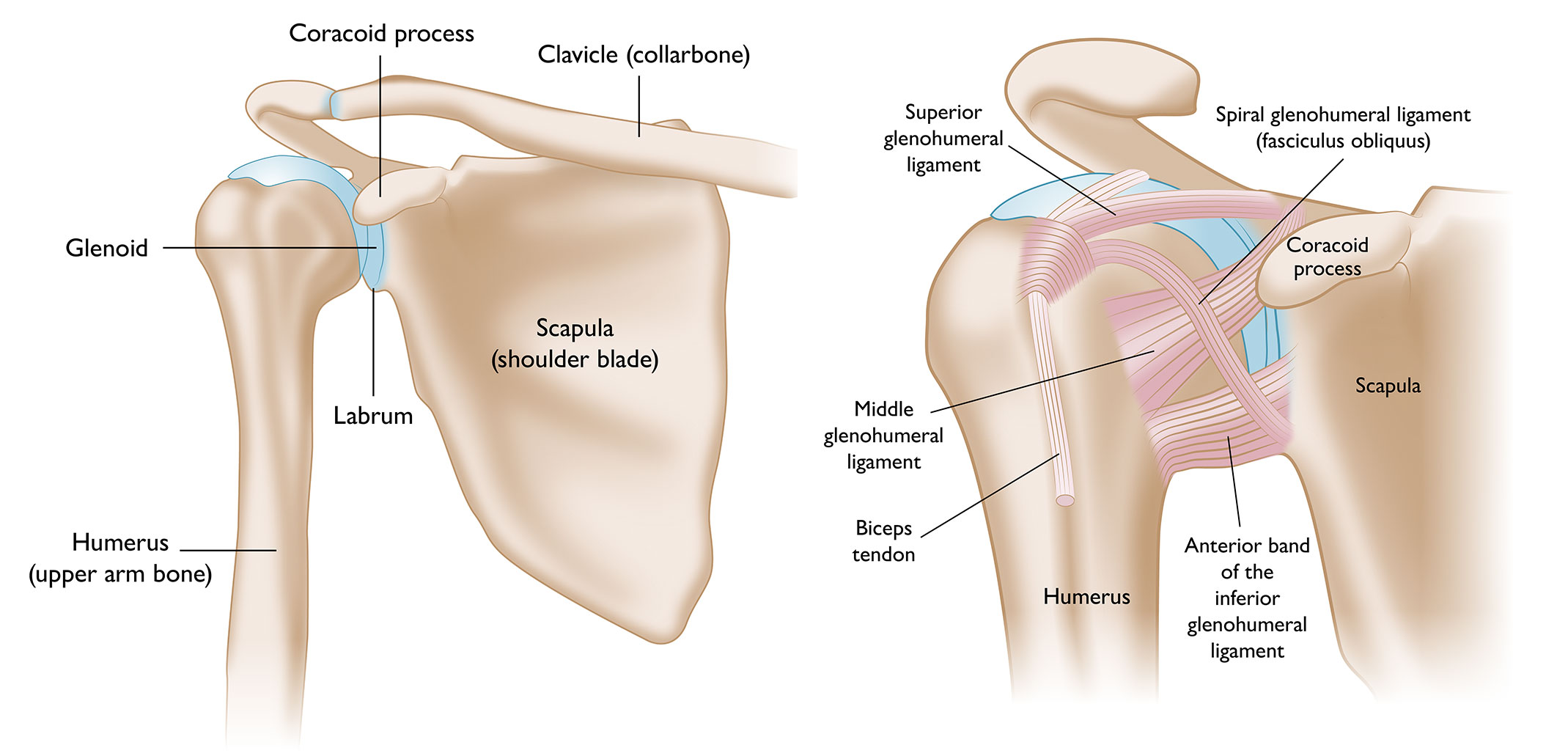
The shoulder is made up of three bones:
- The humerus (arm bone)
- The scapula (shoulder blade)
- The clavicle (collar bone)
These bones are joined together by soft tissues (ligaments, tendons, muscles, and joint capsule) to form a platform for the arm to work.
The shoulder is made up of three joints:
- The glenohumeral joint
- The acromioclavicular joint
- The sternoclavicular joint
The shoulder also has one articulation (place where it joins with another structure in the body), which is the relationship between the scapula (shoulder blade) and the chest wall.
The main joint of the shoulder is the glenohumeral joint. This joint is made up of a ball (the humeral head) on a golf-tee-shaped joint (the glenoid of the scapula).
The bones of the shoulder are covered by several layers of soft tissues:
- The top layer is the deltoid muscle, a muscle just beneath the skin, which gives the shoulder a rounded appearance. The deltoid muscle helps to bring the arm overhead.
- Directly beneath the deltoid muscle is sub-deltoid bursa, a fluid-filled sac, similar to a water balloon.
- The next layer deep (below the subdeltoid bursa) is the rotator cuff, which is a set of four tendons that help assist with shoulder motion.
Description
There are many types of shoulder injuries:
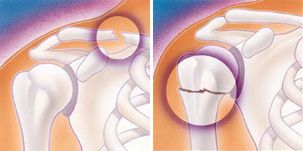
- Fractures are broken bones. Fractures commonly involve the clavicle (collarbone), proximal humerus (top of the upper arm bone), and scapula (shoulder blade).
- Dislocations occur when the bones on opposite sides of a joint do not line up. Dislocations can involve any of three different joints.
- A dislocation of the acromioclavicular joint (collar bone joint) is called a "separated shoulder."
- A dislocation of the sternoclavicular joint interrupts the connection between the clavicle and the breastbone (sternum).
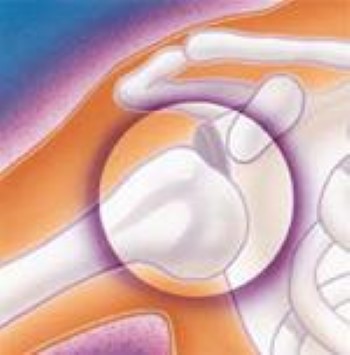
- The glenohumeral joint (the ball and socket joint of the shoulder) can be dislocated toward the front (anteriorly) or toward the back (posteriorly).
- Soft-tissue injuries are tears of the ligaments, tendons, muscles, and joint capsule of the shoulder, such as rotator cuff tears and labral tears.
This article will focus on fractures and dislocations.
Cause
Fractures
Fractures of the clavicle or the proximal humerus can be caused by a direct blow to the area from a fall, collision, or motor vehicle collision.
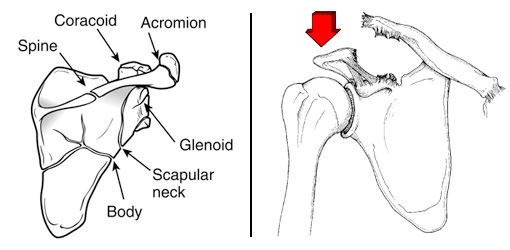
Because the scapula is protected by the chest and surrounding muscles, it is not easily fractured. Therefore, fractures of the scapula are usually caused by high-energy trauma, such as a high-speed motor vehicle collision. Scapula fractures often occur with simultaneous (at the same time) injuries to the chest.
Shoulder Dislocation
- Anterior (toward the front) dislocations of the shoulder are caused by the arm being forcefully twisted outward (external rotation) when the arm is above the level of the shoulder. These injuries can occur from many different causes, including a fall or a direct blow to the shoulder.
- Posterior (toward the back) dislocations of the shoulder are much less common than anterior dislocations of the shoulder. Posterior dislocations often occur from seizures or electric shocks when the muscles of the front of the shoulder contract and forcefully tighten.
Shoulder Separation
Dislocations of the acromioclavicular joint can be caused by a fall onto the shoulder or from lifting heavy objects. The term "shoulder separation" is a bit misleading, as the joint injured in this condition is not the true shoulder joint.
Symptoms
Symptoms of fractures about the shoulder are related to the specific type of fracture.
General Symptoms
- Pain
- Swelling and bruising
- Inability to move the shoulder
- A grinding sensation (crepitus) when the shoulder is moved
- Deformity — "It does not look right"
Specific Symptoms: Clavicle Fracture
- Swelling and bruising about the middle of the collarbone area
- An area that may have a bump, which is actually the prominent (bulging) ends of the fracture under the skin
- Limited shoulder range of motion, although not as much as with fractures of the proximal humerus
Specific Symptoms: Proximal Humerus Fracture
- A severely swollen shoulder
- Very limited movement of the shoulder
- Severe pain
- Bruising around the top of the arm
Specific Symptoms: Scapular Fracture
- Pain
- Swelling
- Severe bruising about the shoulder blade
Specific Symptoms: Shoulder Separation (Acromioclavicular Joint Separation)
- Pain over the top of the shoulder
- A prominence or bump about the top of the shoulder
- The sensation of something sticking up on the shoulder
Specific Symptoms: Shoulder Dislocation (Glenohumeral Joint Dislocation)
- A prominence, or bump, about the front of the shoulder
- Inability to move the arm
- An arm rotated outward
- The sensation of a "dead arm"
Doctor Examination
Most fractures are diagnosed with X-rays of the area and by physical examination. Sometimes, additional imaging techniques, such as a computed tomography (CT) scan and/or magnetic resonance imaging (MRI) scan, are necessary.
Treatment
Clavicle Fractures
Clavicle fractures have traditionally been treated without surgery.
Surgery is necessary when the fracture has broken through the skin, or the bone is severely out of place. More recently, there is some evidence that surgical repair of certain types of clavicle fractures can be beneficial.
Surgery typically involves fixation of the fracture with plates and screws or rods inside the bone. Discuss the risks and benefits of this operation with your surgeon.
Proximal Humerus Fractures
Most fractures of the proximal humerus can be treated without surgery if the bone fragments are not severely out of position (displaced). If surgery is necessary, it usually involves:
- Fixation of the fracture fragments with plates, screws, or pins; or
- Shoulder replacement
Scapula Fractures
Most fractures of the scapula can be treated without surgery. Treatment involves immobilization with a sling or shoulder immobilizer, icing, and pain medications. The patient will be examined for additional injuries.
In rare cases, scapula fractures may best be treated with surgery. These tend to be cases where:
- There are fracture fragments involving the shoulder (ball and socket) joint; or
- There is an additional severe fracture of the clavicle
Surgery involves realignment of the bones and fixation of the fracture fragments with plates and screws.
Shoulder Separations (Acromioclavicular Joint)
Treatment of shoulder separations is based on the severity of the injury as well as the direction of the separation and the physical requirements of the patient.
Less severe shoulder separations are usually treated without surgery.
Severe separations in an upward direction or dislocations in the backward or downward directions often require surgery. Surgery involves repair or reconstruction of the ligaments.
Professional athletes and manual laborers are often treated with surgery, but the results can be unpredictable depending on the specific injury and activity demands after the operation.
Shoulder Dislocations (Glenohumeral Joint)
The initial treatment of a shoulder dislocation involves reducing the dislocation ("putting it back in the socket"). This usually involves treatment in the emergency room.
The patient is given some mild sedation and pain medicine, usually through an intravenous (IV) line. Often, the physician will move the shoulder until the joint is realigned. Realignment is confirmed on an X-ray, and the shoulder is then placed in a sling or special brace.
Additional treatment, which is done at a later date, is based on:
- The patient's age
- Evidence of persistent (ongoing) problems with the shoulder going out of place
- The underlying associated soft-tissue injury (either to the rotator cuff or the capsulolabral complex)
Patients who are 25 years of age or younger generally require surgery. Persistent instability (dislocations) of the shoulder usually requires surgery. Surgery involves repair of the torn soft tissues.
Recovery
Life after a shoulder fracture, separation, or dislocation can be greatly affected for several weeks or even months. Most shoulder injuries, whether they are treated surgically or nonsurgically, require a period of immobilization followed by rehabilitation.
If the injury was not severe, there is fairly rapid improvement and return of function after the first 4 to 6 weeks. But pain, strength, and range of motion often continue to improve even up to 12 months after the injury.
Shoulder exercises, usually as part of a supervised physical therapy program, are usually necessary. Exercises decrease stiffness, improve range of motion, and help the patient regain muscle strength.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.