Diseases & Conditions
Shoulder Separation
This article was written and/or reviewed by a member of American Shoulder and Elbow Surgeons (ASES).
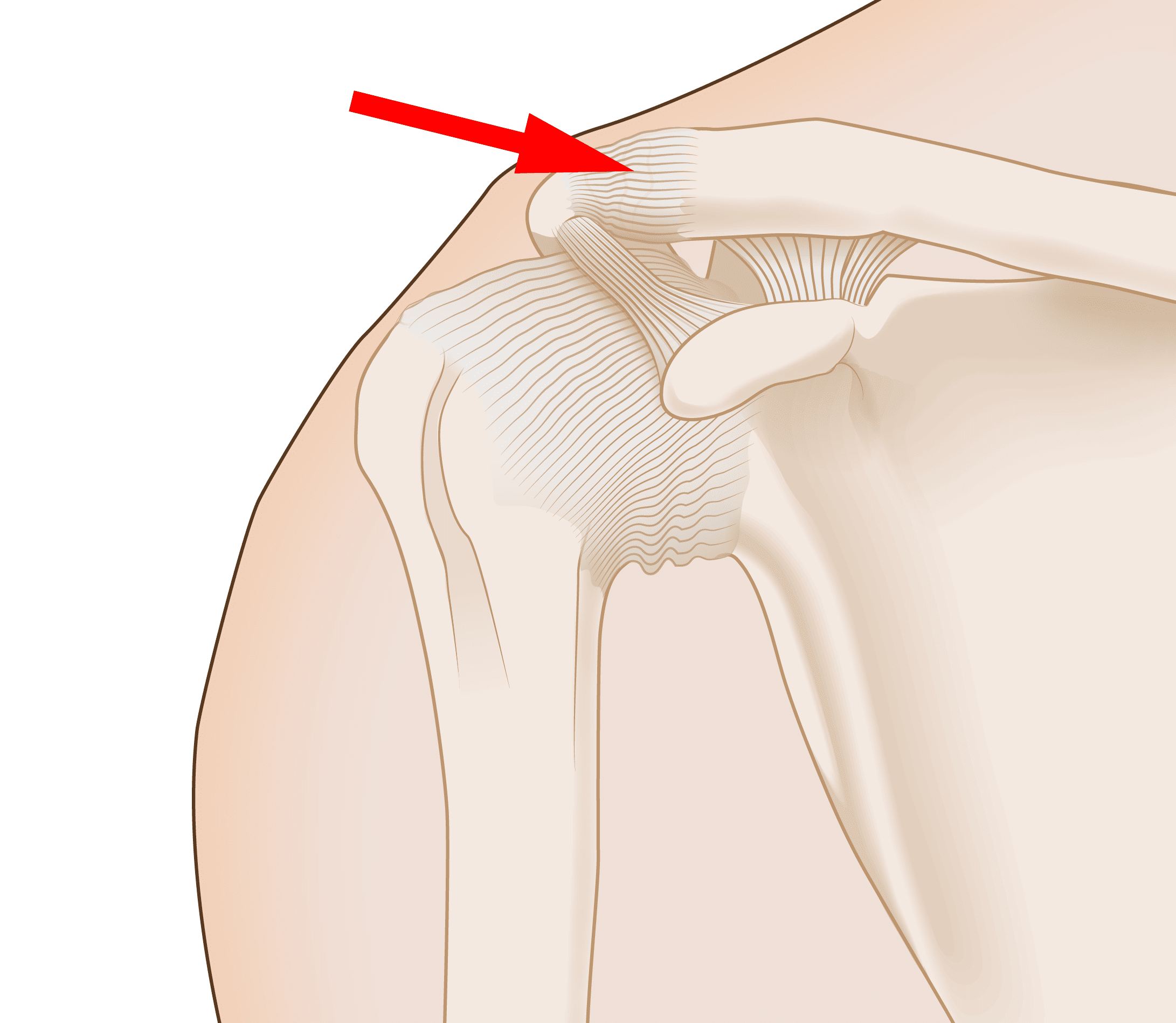
A shoulder separation is not an injury to the shoulder's main ball-and-socket joint. The injury actually involves the acromioclavicular joint (also called the AC joint). The AC joint is where the clavicle (collarbone) meets the highest point of the shoulder blade (acromion).
Cause
The most common cause of a separation of the AC joint is a fall directly onto the shoulder. The fall injures the ligaments that surround and stabilize the AC joint.
If the force is severe enough, the ligaments attaching to the underside of the clavicle are torn. These are called the coracoclavicular (CC) ligaments. This tearing causes the separation of the collarbone and the shoulder blade. The scapula (shoulder blade) moves downward from the weight of the arm, creating a bump or bulge above the shoulder.
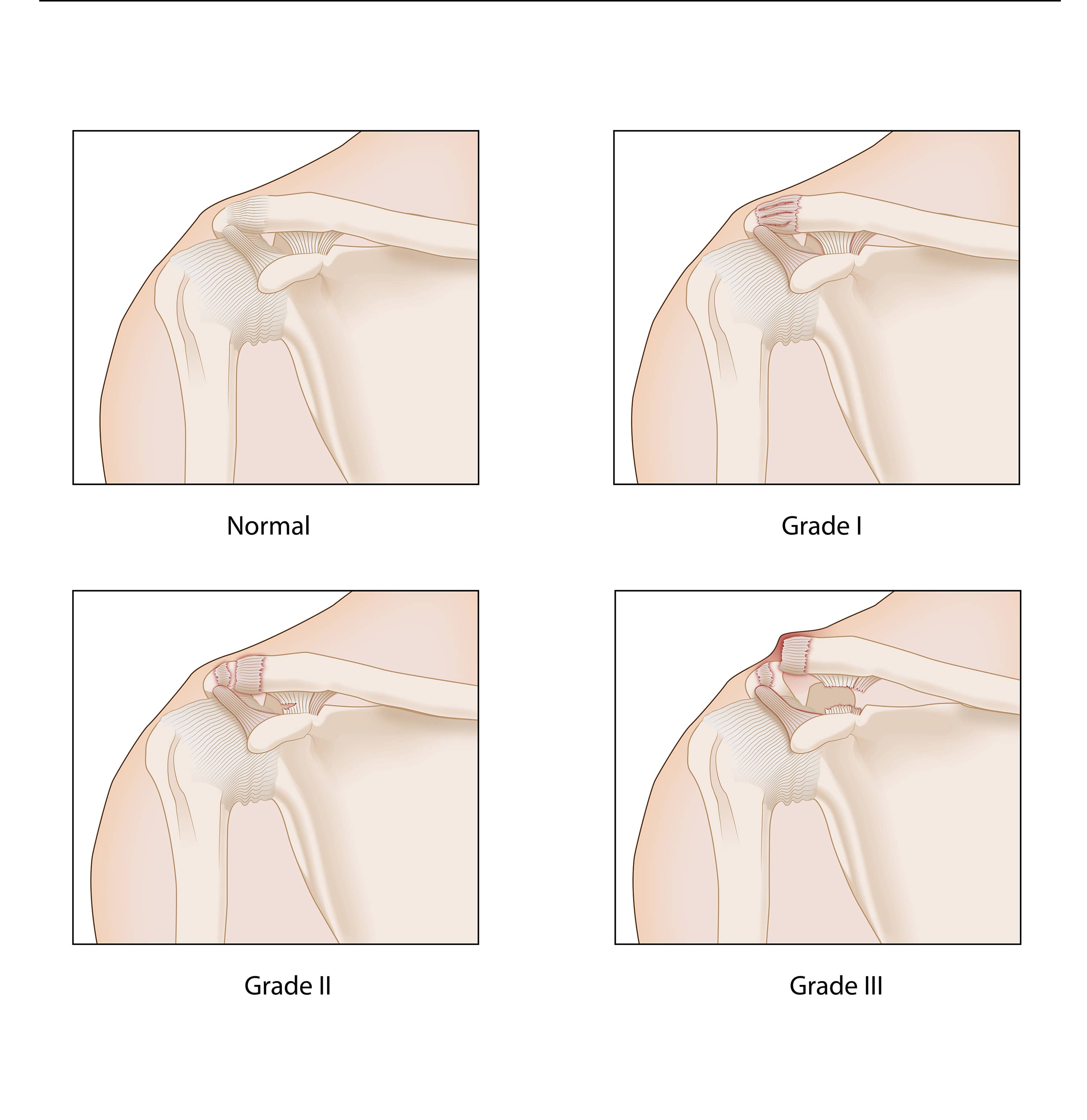
The injury can range from a mild sprain without a bump to a complete disruption with a very large bump. Good pain-free function often returns even with a very large bump.
- Grade I: A mild shoulder separation involves a sprain of the AC ligaments that does not move the collarbone and looks normal on X-rays.
- Grade II: A more serious injury tears the AC ligaments and sprains or slightly tears the CC ligament, putting the collarbone out of alignment to some extent with a smaller bump.
- Grade III: A more severe shoulder separation completely tears both the AC and CC ligaments and puts the AC joint noticeably out of position, with a larger bump.
- Grade IV: In this injury, the clavicle displaces backward, which is called a posterior displacement.
- Grade V: This injury involves upward (superior) displacement of the clavicle by more than 100%.
- Grade VI: This rare injury involves downward (inferior lateral) displacement of the clavicle.
This article discusses Grade I, II, and III injuries.
Doctor Examination
The injury is easy to identify when it causes deformity.
When there is less deformity, the location of pain and X-rays help the doctor make the diagnosis. Sometimes having the patient hold a weight in the hand can increase the deformity, which makes the injury more obvious on X-rays.
Treatment
Nonsurgical Treatment
Nonsurgical treatments, such as a sling, cold packs, and medications can effectively help manage the pain in almost all patients. Rarely, a doctor may use more complicated supports to help lessen AC joint motion and pain.
Most people with this injury — even professional athletes — return to normal function with nonsurgical treatments, even if there is a persistent, significant deformity/bump. Some people have continued pain around the AC joint, even with only a mild deformity. This may be due to:
- Abnormal contact between the bone ends when the joint is in motion
- Development of arthritis
- Injury to the cartilage between the clavicle and acromion
It is often worthwhile to wait and see if reasonable function returns without surgical treatment. Most patients, even with very severe injuries, are often managed effectively without surgery. In fact, recent studies on AC joint injuries have shown that nonsurgical management may be better than surgical management in most types of AC joint injuries.
Surgical Treatment
Surgery can be considered if pain persists or the deformity is severe.
- A surgeon might recommend trimming back the end of the collarbone so it does not rub against the shoulder blade bone (acromion).
- When there is significant deformity, reconstructing the ligaments that attach to the underside of the collarbone is helpful. This type of surgery works well even if it is done long after the problem began.
These operations can be done arthroscopically or open, with a plate or without. If a plate is used to assist with the surgery, it is usually removed after healing of the shoulder separation.
Whether treated nonsurgically or with surgery, the shoulder will require rehabilitation to restore and rebuild motion, strength, and flexibility.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.