Diseases & Conditions
Pelvic Fractures
The pelvis is the ring of bones located at the base of the spine. Fractures of the pelvis are uncommon — they make up only about 3% of all fractures in adults.
Most pelvic fractures are caused by trauma, typically a high-energy event, such as a motor vehicle collision. Because the pelvic bones are near major blood vessels and organs, pelvic fractures may cause extensive bleeding and other injuries that require urgent treatment.
In some cases, a lower-impact event — such as a minor fall — may be enough to cause a pelvic fracture in an older person who has weaker bones, like those with osteoporosis.
Treatment for a pelvic fracture depends on how serious the injury is. While lower-energy fractures can often be managed with conservative (nonsurgical) treatments, patients with high-energy pelvic fractures may need surgery to reconstruct the pelvis and restore stability so they can get back to their daily activities.
Anatomy of the Hip
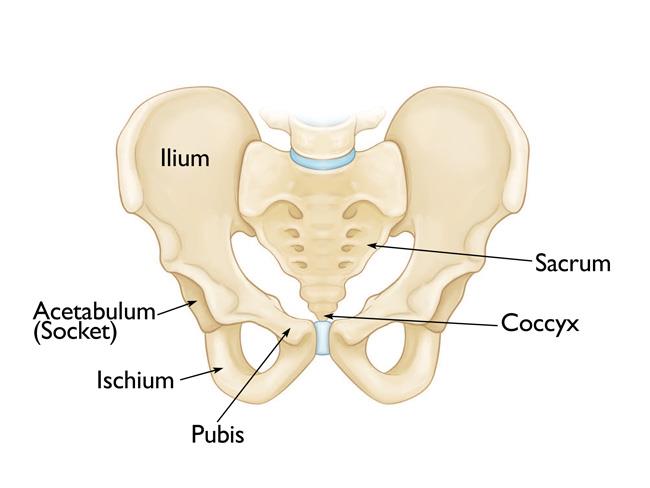
The pelvis is a ring of bones located at the lower end of the trunk — between the spine and the legs. The pelvic bones include:
- The sacrum (the large triangular bone at the base of the spine)
- The coccyx (tailbone)
- The hip bones (ilium, acetabulum, ischium, and pubis)
Each hip bone contains three bones — the ilium, ischium, and pubis — that are separate during childhood but fuse (join) together as we grow older. These three bones meet to form the acetabulum — the hollow cup that serves as the socket for the ball-and-socket hip joint.
Bands of strong connective tissues called ligaments join the pelvis to the sacrum, creating a bowl-like cavity below the rib cage.
Major nerves, blood vessels, and parts of the bowel, bladder, and reproductive organs all pass through the pelvic ring. The pelvis protects these important structures from injury. It also serves as an anchor for the muscles of the hip, thigh, and abdomen.
Types of Pelvic Fractures
Because the pelvis is a ring-like structure, when you fracture one part of the structure, there is often a fracture or damage to ligaments at another point in the structure. There are several common pelvic fracture patterns. The specific pattern of the fracture depends on the direction in which it was broken and the amount of force that caused the injury.
In addition to being described by the specific fracture pattern, pelvic fractures are often described as "stable" or "unstable," based on how much damage has occurred to the structural integrity of the pelvic ring.
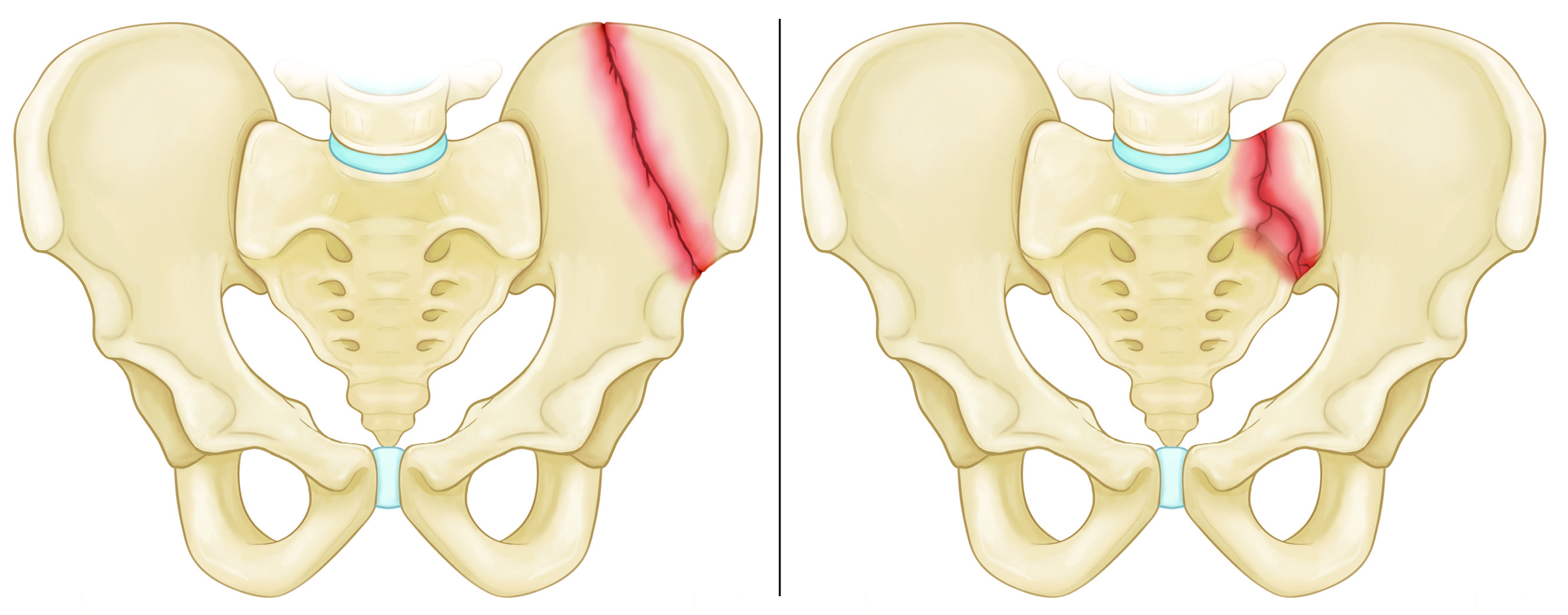
Stable fracture. In this type of fracture, there is often only one break in the pelvic ring, and the broken ends of the bones line up adequately. Low-energy fractures are often stable fractures.
Stable pelvic fracture patterns include:
- Iliac wing fracture
- Sacrum fracture (incomplete)
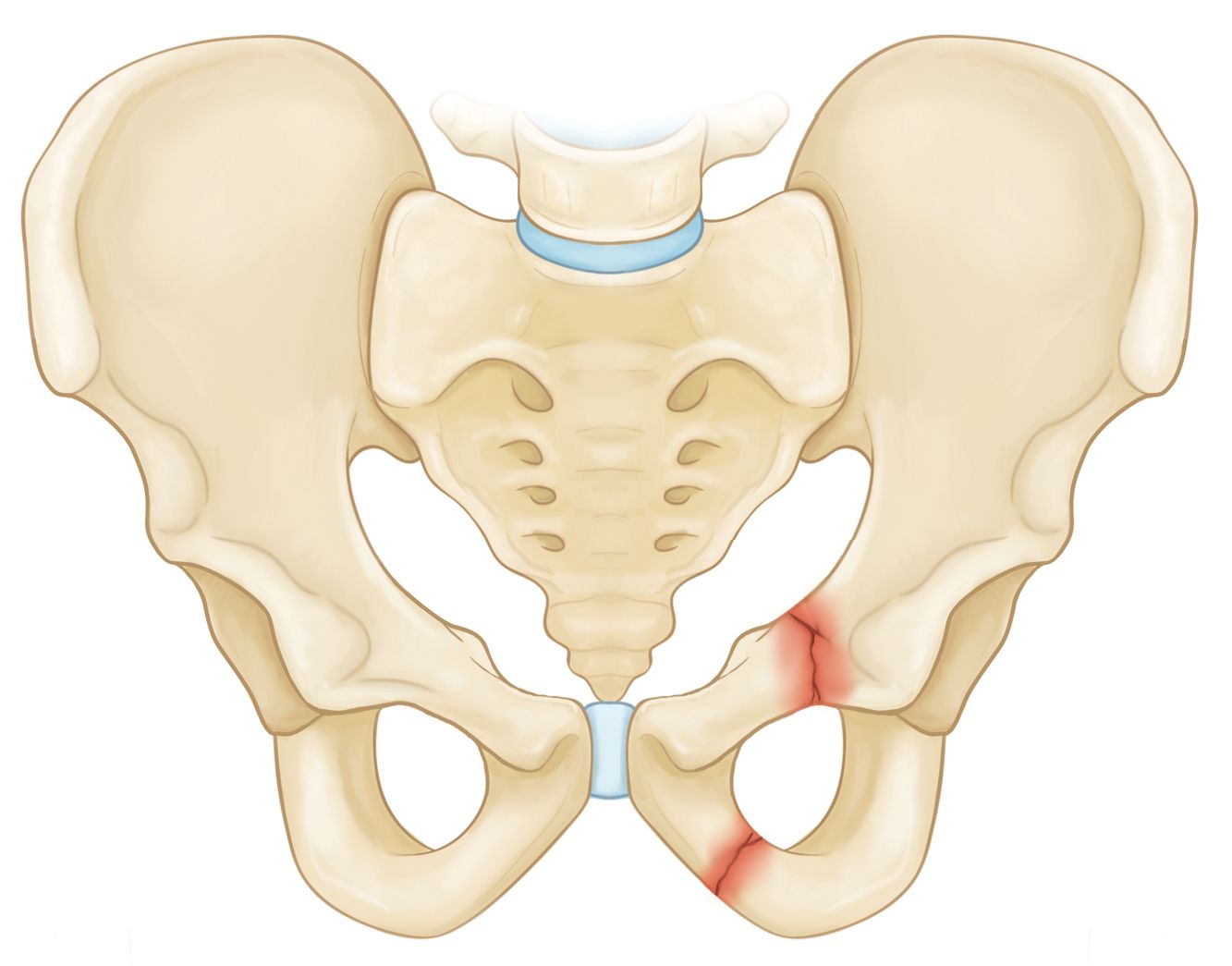
- Superior pubic ramus fracture
- Inferior pubic ramus fracture
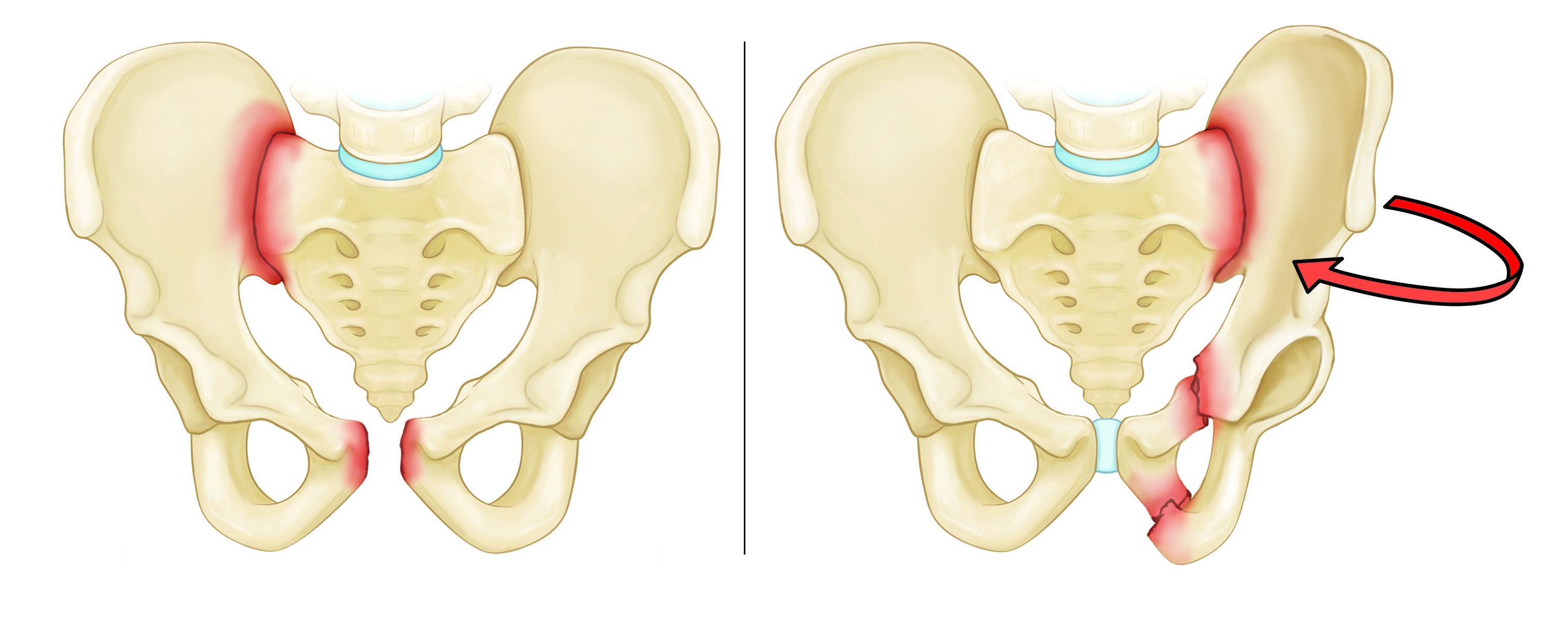
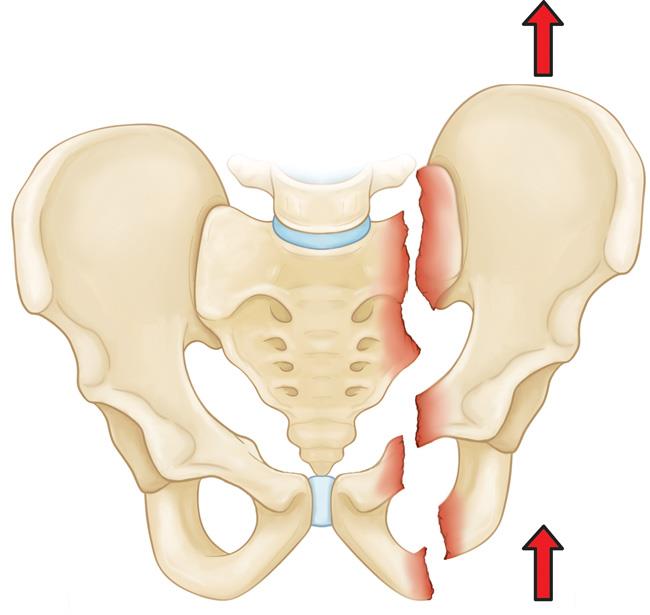
Unstable fracture. In this type of fracture, there are usually two or more breaks in the pelvic ring. Also, the ends of the broken bones do not line up correctly, which is called displacement. This type of fracture is more likely to occur due to a high-energy event.
Unstable pelvic fracture patterns include:
- Anterior-posterior compression fracture
- Lateral compression fracture
- Vertical shear fracture
Both stable and unstable pelvic fractures can also be divided into:
- Closed fractures, in which the skin is not broken.
- Open fractures, in which the bone fragments stick out through the skin. These are serious injuries with a high mortality (death) rate. The reason open fractures are so serious is that once the skin is broken, infection in both the wound and the bone can occur. Immediate treatment is needed to prevent infection.
Causes of Pelvic Fractures
High-Energy Trauma
A pelvic fracture may result from a high-energy force, such as that generated during:
- A car or motorcycle collision
- A crush accident
- A fall from a significant height (such as a ladder or rooftop)
Depending on the direction and amount of the force, these injuries can be life-threatening and require surgical treatment.
Bone Insufficiency
A pelvic fracture may also occur due to weak or insufficient bone. This is most common in older people whose bones have become weakened by osteoporosis.
In people with osteoporosis, even a fall from a standing height or during a routine activity — such as getting out of the bathtub or walking down stairs — can result in a pelvic fracture.
These injuries are usually stable fractures of an individual pelvic bone that do not damage the structural integrity of the pelvic ring. However, the fractures can be unstable or very painful, and surgery may be recommended.
Other Causes of Pelvic Fractures
Less commonly, a fracture may occur when a piece of the ischium bone tears away from the site where the hamstring muscles attach to the bone. This type of fracture is called an avulsion fracture, and it is most common in young athletes who are still growing. An avulsion fracture does not usually make the pelvis unstable or injure internal organs.
Symptoms of a Pelvic Fracture
A fractured pelvis is almost always painful. Moving the hip or trying to walk will make the pain worse. Often, the patient will try to keep their hip or knee bent in a specific position to avoid worsening the pain.
Some patients may also have swelling or bruising in the hip area.
Doctor Examination
Emergency Stabilization of Pelvic Fractures
Patients with high-energy fractures will almost always go or be brought to an emergency room for initial treatment.
These patients may also have injuries to the head, chest, abdomen, or legs. If their injuries cause significant blood loss, it could lead to shock — a life-threatening condition that can lead to organ failure.
The care of patients with high-energy pelvic fractures requires a team approach with input from a number of specialists. In some cases, doctors must address airway, breathing, and circulatory (blood flow) problems before treating the pelvic fracture and other injuries.
Physical Examination
Your doctor will:
- Carefully examine your pelvis, hips, and legs
- Check for nerve injury by seeing whether you can move your ankles and toes and feel sensation on the bottoms of your feet
- Carefully examine the rest of your body to see if you have any other injuries
Imaging Tests
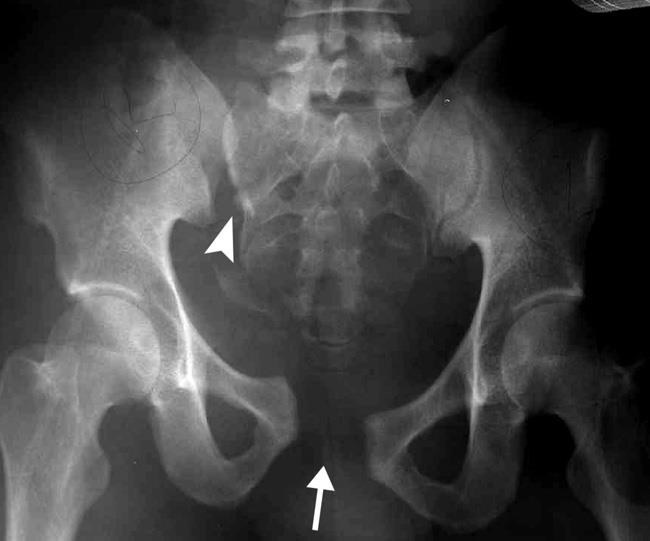
X-rays. X-rays provide images of bones. All pelvic fractures require X-rays — usually from several different angles — to help the doctor see how much the bones are have moved out of place.
Computed tomography (CT) scans. Because this type of injury is complex, a CT scan is commonly ordered for pelvic fractures. A CT scan will provide a detailed, cross-sectional image of the pelvis. This information will help your doctor:
- Better determine the specific pattern and extent of your injury
- Look for other injuries
- Plan for surgery if surgery is needed
Magnetic resonance imaging (MRI) scans: In rare cases, your doctor may order an MRI scan to check for fractures that cannot be seen on an X-ray or CT scan.
Treatment of Pelvic Fractures
Treatment is based on several factors, including:
- The specific pattern of the fracture
- How much the bones are displaced (have moved out of place)
- Your overall condition and whether you suffered other injuries at the same time as the pelvic fracture
Nonsurgical Treatment
Your doctor may recommend nonsurgical treatment for stable fractures in which the bones are nondisplaced or minimally displaced.
Nonsurgical treatments may include:
Walking aids. To avoid bearing weight on your leg, your doctor may recommend that you use crutches or a walker for up to 3 months — or until your bones are fully healed. If you have injuries above both legs, you may need to use a wheelchair for a period of time so that you can avoid bearing weight on either leg.
Medications. Your doctor may prescribe medication to relieve pain, as well as an anti-coagulant, or blood thinner, to reduce the risk of blood clots forming in the veins of your legs and pelvis.
Surgical Treatment
Patients with unstable pelvic fractures may require one or more surgical procedures.
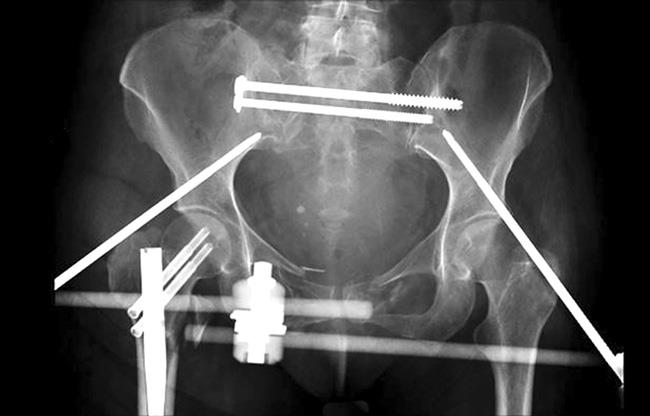
External fixation. Your doctor may use external fixation to stabilize your pelvic area. In this operation, the surgeon inserts metal pins or screws into the bones through small incisions in the skin and muscle. The pins and screws stick out of the skin on both sides of the pelvis where they are attached to carbon fiber bars outside the skin. The external fixator acts as a stabilizing frame to hold the broken bones in proper position.
In some cases, an external fixator is used to stabilize the bones until healing is complete. Once healing is satisfactory, the fixator is then removed. In patients who cannot tolerate a lengthy, more complicated procedure, an external fixator may be used as a temporary treatment until another procedure can be performed.
Skeletal traction. Skeletal traction is a pulley system of weights and counterweights that helps realign the pieces of bone. Skeletal traction is often used immediately after an injury and removed after surgery. Sometimes, acetabular fractures can be treated with skeletal traction alone. This is rare, however, and will be a decision you and your doctor make together.
During skeletal traction, metal pins are placed in the thighbone or shinbone to help position the leg. Weights attached to the pins gently pull on the leg, keeping the broken bone fragments in as normal a position as possible. For many patients, skeletal traction also provides some pain relief.
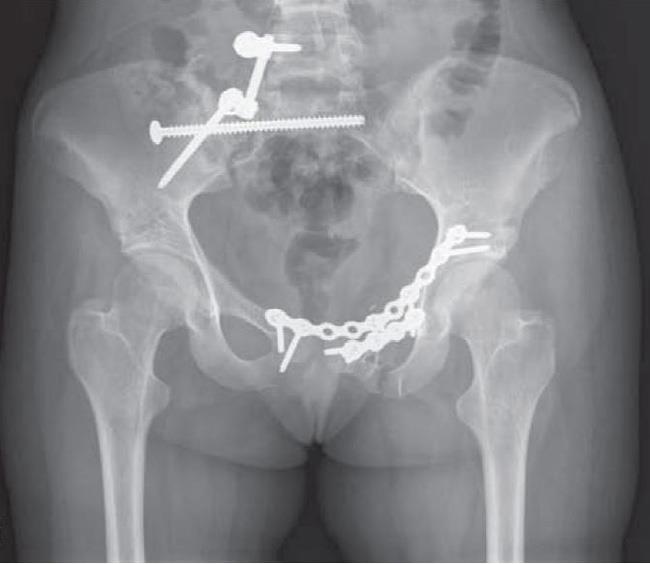
Open reduction and internal fixation. During this operation, the displaced bone fragments are first repositioned (reduced) into their normal alignment. They are then held together with screws or metal plates attached to the outer surface of the bone.
Complications
There are risks with any surgical procedure. Before your surgery, your doctor will discuss each of these risks with you and will take specific steps to help avoid potential complications.
Possible complications include:
- Wound healing problems, including infection
- Damage to nerves or blood vessels
- Blood clots
- Pulmonary embolism — a blood clot in the lungs
- Nonunion (when the bones do not heal)
- Malunion (when the bones heal in an abnormal position)
- Leg length inequality (one leg is shorter than the other); this can happen if the pelvic ring heals in an abnormal position on one side compared to the other
Recovery
Pain Management
After surgery, you will feel some pain. This is a natural part of the healing process. Your doctor will work to reduce your pain, which can help you recover from surgery faster.
Medications are often prescribed for short-term pain relief after surgery. Many types of medicines are available to help manage pain, including opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and local anesthetics. Your doctor may use a combination of these medications to improve pain relief, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery, their use has risks and complications. These medications can be addictive and potentially dangerous. It is therefore important to use opioids only as directed by your doctor, to use as little as possible for as short a time as possible, and to stop taking them as soon as your pain starts to improve. Tell your doctor if your pain has not begun to improve within a few days after surgery.
Early Movement
In most cases, your doctor will encourage early movement. Most patients begin walking — with weightbearing restrictions — and doing foot and leg exercises as soon as possible after surgery.
Physical Therapy
Specific exercises will help you regain flexibility and restore range of motion in your hip. Other exercises will help you build strength and endurance so that you are better able to perform your daily activities.
Blood Clot Prevention
Although early movement is encouraged, your mobility after surgery will still be somewhat limited. For this reason, your doctor may prescribe an anticoagulant, or blood thinner, to help prevent blood clots from forming in the deep veins of your pelvis and legs.
Weightbearing
Your doctor may recommend that you use crutches or a walker for 6 to 8 weeks or longer, depending on the severity of the injury and how it is healing.
Full weightbearing is usually allowed by 3 months — or when your bones are fully healed. You may need to use a cane or walking aid for a longer period of time.
Learn more: How to Use Crutches, Canes, and Walkers
Outcomes for Pelvic Fractures
Stable pelvic fractures tend to heal well.
Unstable pelvic fractures sustained during high-energy incidents, such as motor vehicle accidents, may result in serious complications, including severe bleeding, internal organ damage, and infection. If these injuries are addressed successfully, the fracture usually heals well.
You may walk with a limp for several months if there was damage to the muscles around your pelvis. These muscles may take up to 1 year to become strong again.
Future problems, such as pain, reduced mobility, incontinence, and sexual dysfunction, may result from nerve and organ damage related to the pelvic fracture.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.