Diseases & Conditions
Paget's Disease of Bone
Paget's disease of bone is a chronic disease of the skeleton that leads to abnormally shaped, weak, brittle bones. It most often affects older people, occurring in approximately 2 to 3% of the population over the age of 55.
- Many patients with Paget's disease have no symptoms and are unaware they have the disease until X-rays are taken for some other reason.
- When bone pain and other symptoms are present, they can be related to the disease itself or to complications that arise from the disease — such as arthritis, bone deformity, and fractures.
In most cases, treatment for Paget's disease involves taking medications to help slow or stop the progress of the disease. Patients who have complications may need surgery to realign deformed bones or to help fractures heal.
Description
Paget's disease can affect any bone in the body. It appears most often in the spine, pelvis, long bones of the limbs, and skull. It can be present in just one bone or in several bones. It can affect the entire bone or just part of it.
Bone Remodeling
In healthy bone, a process called remodeling removes old pieces of bone and replaces them with new, fresh bone. This takes place every day. Bone is absorbed and then re-formed in response to the normal stresses on the skeleton. More specifically:
- Cells of the bone called osteoclasts absorb bone.
- Cells of the bone called osteoblasts make new bone.
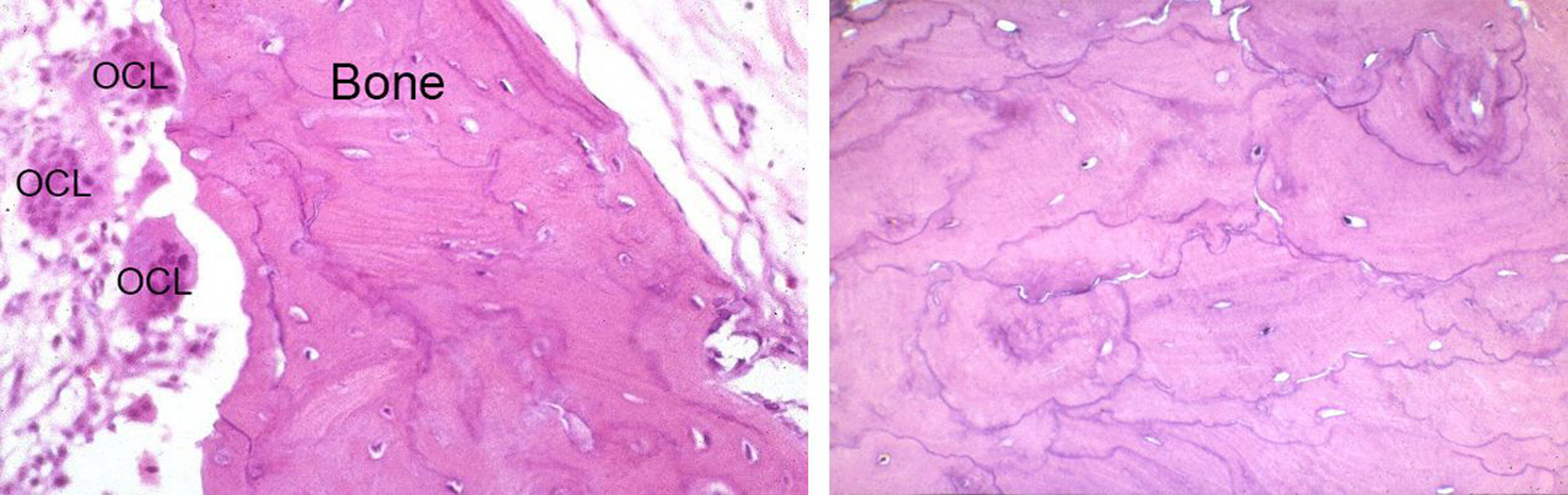
In Paget's disease, osteoclasts are more active than osteoblasts. This means that there is more bone absorption than normal. The osteoblasts try to keep up by making new bone, but they overreact and make excess bone that is abnormally large, deformed, and fits together haphazardly (in a chaotic, or irregular, way).
Normal bone has a tight overlapping structure, like a well-constructed brick wall. Bone affected by Paget's disease has an irregular mosaic pattern, as though the bricks were just dumped in place. The end result is bones that are large and dense, but weak and brittle. The bone is prone to fractures, bowing, and deformities.
Cause
The cause of Paget’s disease is not known, but doctors have identified a number of risk factors that make someone more likely to develop the disease. These include:
- Genetics. Paget's disease tends to run in families. In as many as 25 to 40% of cases, another relative will also have the disease.
- Age. Paget's disease occurs only rarely in people under the age of 40. It is more common as people age.
- Ancestry. It is more common in people of Anglo-Saxon descent and those who live in certain geographic areas, such as the U.S., England, Australia, New Zealand, and Western Europe. It is not common in Scandinavia, China, Japan, or India.
- Environmental factors. Some studies suggest that certain environmental exposures may play a role in the development of Paget's disease, but this has not been proven.
While there are no known ways to prevent Paget's disease from occurring, eating a healthy diet with sufficient calcium and vitamin D, and getting regular exercise, are important components in maintaining skeletal health and joint mobility.
Symptoms
Many people with Paget's disease do not have any symptoms. The disease is often first discovered when X-rays are taken for another reason or when routine blood work indicates an elevated blood serum alkaline phosphatase level.
Pain
In patients who do have symptoms, bone pain is the most common complaint. This pain can be related to active Paget's disease or to its complications, which include:
- Fractures due to brittle bone.
- Deformity of bone, including bowing of the affected bone.
- Advanced arthritis in joints near the affected bone.
- Compression (pressure) on neighboring nerves from enlarged bones, leading to nerve pain. In severe cases, this can lead to a loss of sensation or motor function.
Other Symptoms
Symptoms can also arise from the effect of the disease on calcium levels in the blood stream. When Paget's disease is active in several bones, overactive osteoclasts may release enough calcium from the bone as they break it down to cause an elevated calcium level in the blood. This rare complication can lead to a number of symptoms, including:
- Fatigue
- Weakness
- Loss of appetite
- Abdominal pain
- Constipation
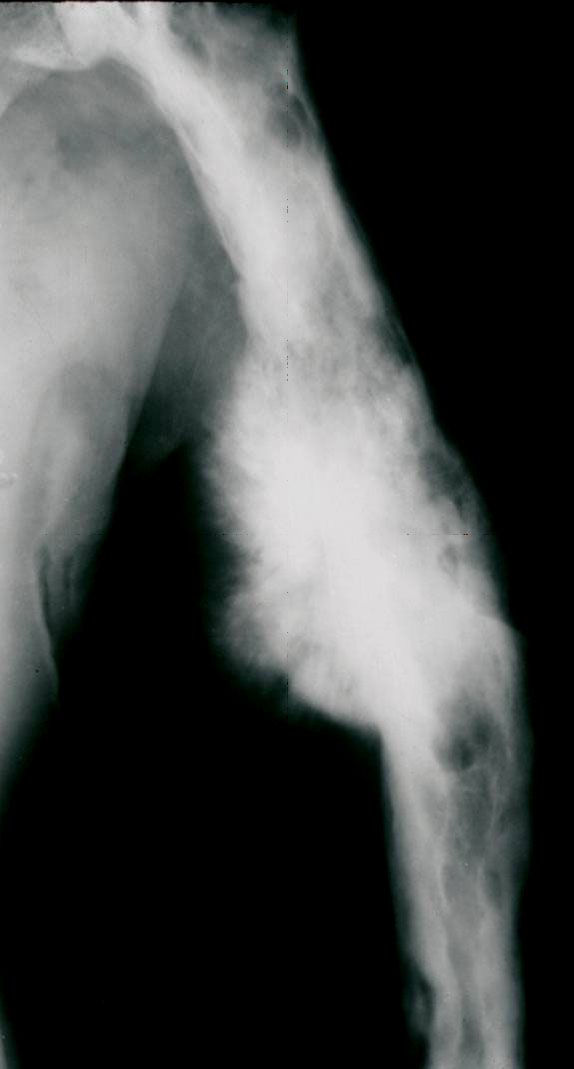
Very rarely, Paget's disease can progress to a type of bone cancer called Paget's sarcoma. When this occurs, symptoms may include severe and unrelenting pain in the area affected by Paget's disease.
Paget's sarcoma occurs in only about 1% of patients with Paget's disease. These patients are usually over the age of 70.
This type of malignant (cancerous) bone tumor is very aggressive and has a poor prognosis. None of the medical treatments for Paget's disease are known to lower the risk for the development of Paget's sarcoma.
Doctor Examination
In many cases, Paget's disease is discovered incidentally (by accident) when X-rays are taken for some other reason, like an injury. Occasionally, there can be abnormalities in routine bloodwork. If needed, your doctor will perform a physical examination and order a number of tests to confirm the diagnosis.
Tests
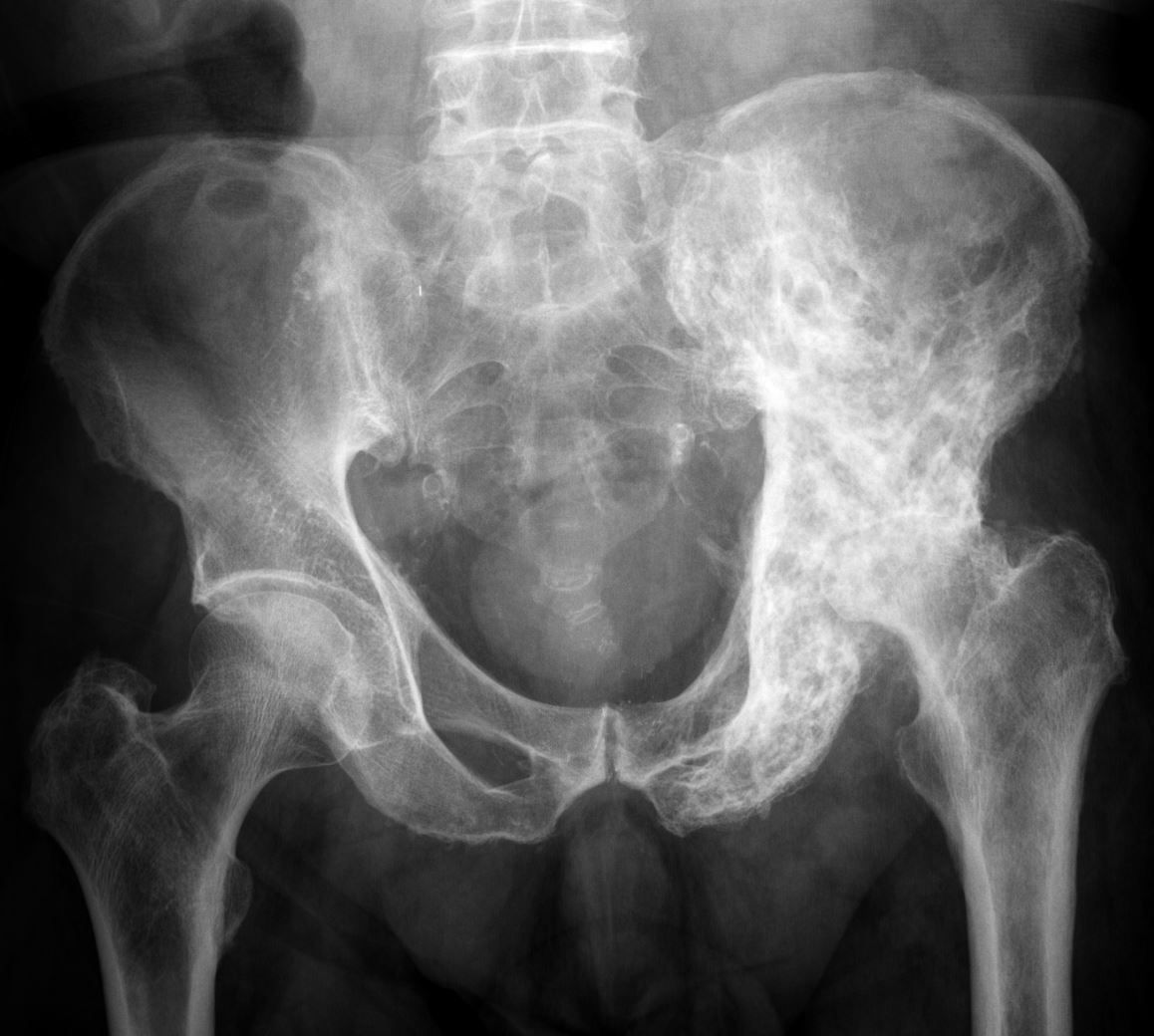
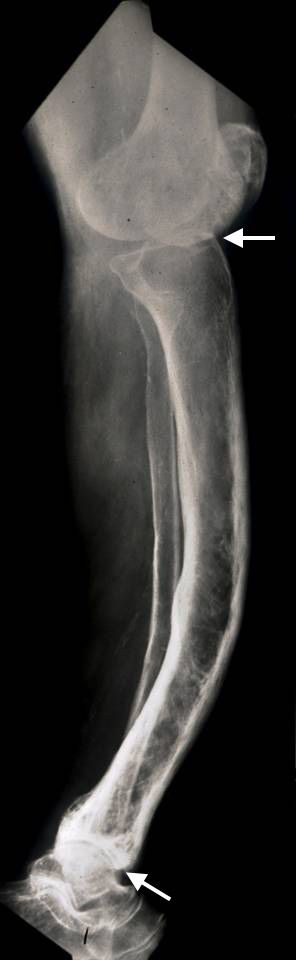
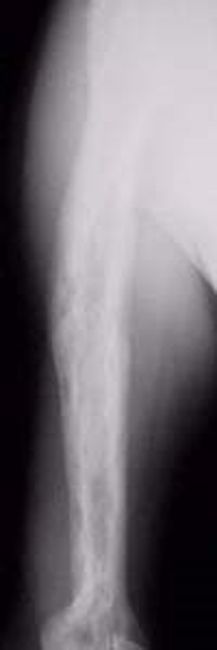
X-rays. X-rays provide images of dense structures, such as bone. Paget's disease can usually be diagnosed by looking at an X-ray. A bone affected by Paget's usually appears larger and denser than a normal bone. It may also have a deformed shape.
In the very early stages of Paget's disease, when there is just overactive absorption of bone occurring, it can look like there is a hole in the bone. Later in the disease process, this darker area can take the shape of a flame or a "V," with denser, thicker bone following behind it.
Laboratory tests. A blood test called serum alkaline phosphatase may also be used to help confirm the diagnosis. In patients with Paget's disease, alkaline phosphatase levels are usually quite elevated — a reflection of the high bone turnover rate. Usually, calcium levels are normal.
Paget's disease can also be detected with urine tests that show rapid bone turnover. These include elevated levels of urinary hydroxyproline, N-telopeptide, alpha-C-telopeptide, or deoxypyridinoline
Bone scan. A bone scan may be used to help determine which bones are affected. During this test, a very small amount of radioactive dye is injected into a vein. A special imaging device is then used to detect areas of the skeleton with an increased uptake of the radioactive material. These "hot spots" indicate areas where there is more bone turnover than normal.
Paget's disease almost always looks "hot" on a bone scan, except when the condition has been present for a long time and has burned out.
Biopsy. A biopsy is sometimes necessary to confirm the diagnosis of Paget's disease or to rule out other conditions.
In a biopsy, a small sample of the affected bone is removed and examined under a microscope. The procedure can be performed under local anesthesia with a needle or as a small open operation.
Treatment
There is no cure for Paget's disease and no way to reverse its effects on bone. Treatment focuses on relieving symptoms and preventing future complications.
Nonsurgical Treatment
If you do not have pain or other symptoms, no treatment is required. Your doctor may recommend simply monitoring your condition with regular office visits and X-rays to watch for changes in the affected bone and to ensure that complications do not develop.
If symptoms do occur, your doctor may recommend one or more nonsurgical treatments.
Rest, ice, compression, elevation (RICE): Often, simple techniques can relieve bone or joint pain, such as resting the affected limb, using an ice pack (20 minutes on, 20 minutes off), applying an ace bandage or other compressive wrap, and elevating the limb. Some patients find a heating pad or topical creams (e.g., diclofenac gel, IcyHot, Biofreeze) can be helpful.
Assistive devices. If your pelvis or leg is affected by the disease, using a cane can help relieve pain by decreasing the forces going through the bone. Using a cane can also help prevent falls, so there is less risk of fracture in the bone — a common complication of Paget's disease.
Wearing a brace can help relieve pain by preventing malalignment of the affected bones.
Physical therapy. Your doctor might recommend a course of physical therapy to improve your strength and range of motion.
Nonsteroidal anti-inflammatory drugs (NSAIDs). Anti-inflammatory medications like ibuprofen, naproxen, and aspirin can help relieve mild bone pain that arises from Paget's disease or from arthritis that may be associated with the disease.
Bisphosphonate medications. When bone pain is more significant, medications called bisphosphonates are the treatment of choice. These drugs block osteoclasts and can be very effective in treating Paget's disease.
There are several types of bisphosphonates. Some are taken by mouth (orally) and others are given as an injection (intravenously). Your doctor will talk to you about which type is best for you and how long you will need to take it.
During treatment with bisphosphonates, your doctor will perform blood tests periodically to check your alkaline phosphatase level. A falling alkaline phosphatase level and improvement in bone pain are indications that treatment is working.
Surgical Treatment
In some cases, surgery may be needed to treat the complications of Paget's disease, including:
- Fractures (broken bones)
- Malalignment or deformity of bone
- Severe arthritis
The surgical procedures used to treat fractures, malalignment, or arthritis in patients with Paget's disease are similar to those used to treat similar conditions in people with normal bone.
These procedures may include:
- Internal fixation. This procedure can be used to treat fractures in bone affected by the disease. In internal fixation, bone fragments are first repositioned into their normal alignment, then held in place with screws, wires, pins, or metal plates attached to the outside of the bone.
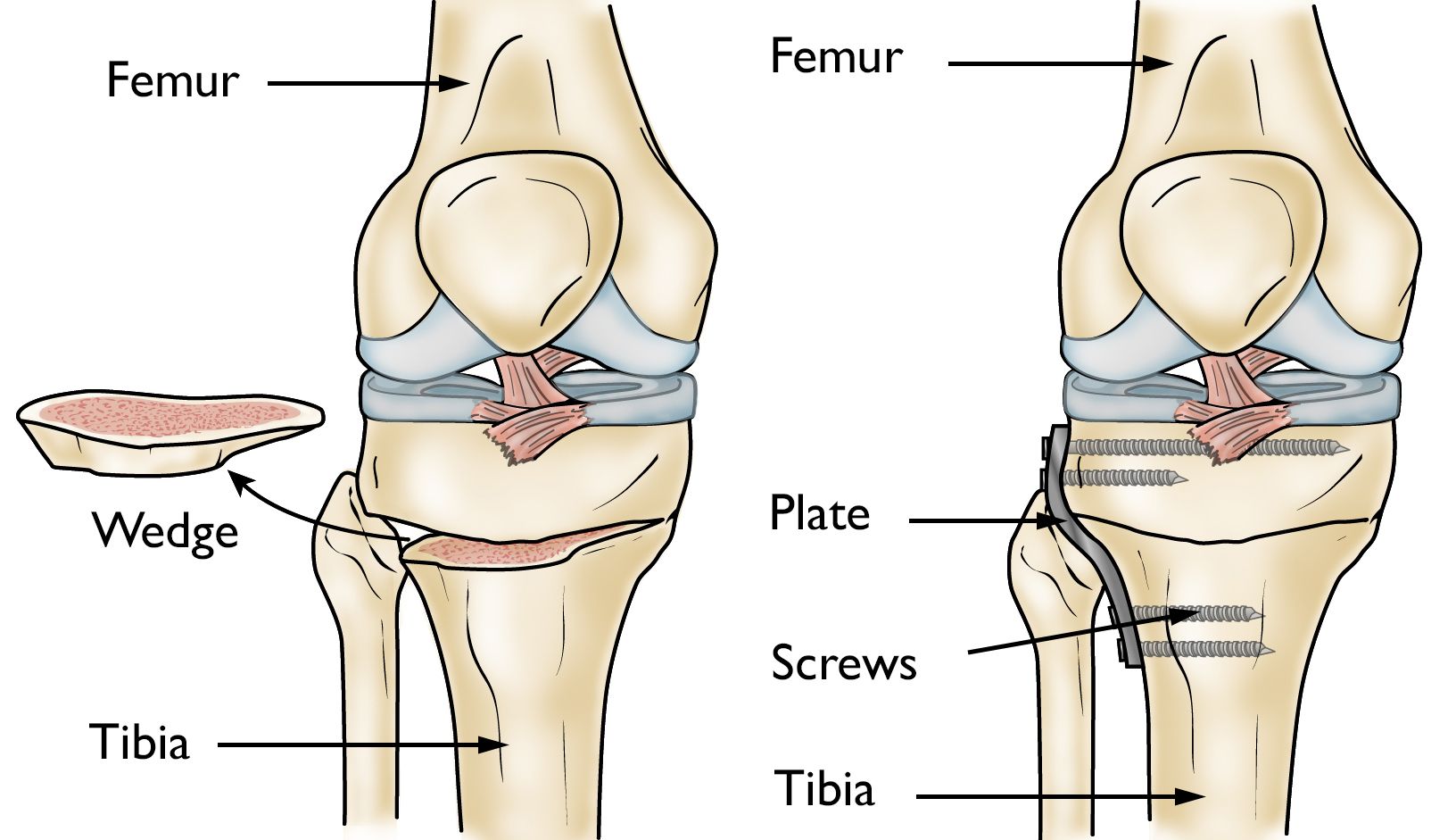
- Osteotomy. Though rarely offered as an option for Paget's disease, an osteotomy can help relieve pain and restore alignment to weight-bearing joints that are affected by Paget's disease, especially the knee and hip. During the procedure, the surgeon removes a wedge of bone near the damaged joint in order to shift weight onto a healthier part of the joint.
- Total joint replacement. In this procedure, parts of an arthritic or damaged joint are removed and replaced with a metal, plastic or ceramic device called a prosthesis. The prosthesis is designed to replicate the movement of a normal, healthy joint.
Surgery may also be needed if an enlarged bone begins to compress (put pressure on) nerves, especially in the spine or skull. In the rare case of Paget's sarcoma, surgery is almost always used to try to remove the tumor entirely. Chemotherapy and radiation therapy may also be used.
Because Paget's disease increases the blood supply to bones, your doctor may recommend taking bisphosphonates for a period of time before surgery to help reduce potential blood loss.
Bones affected by Paget's disease may take longer to heal than normal bones. A longer period of rehabilitation may also be necessary.
Outcomes
If treatment begins before major changes in bone occur, most patients with Paget's disease are able to live a normal, active life. When complications develop, surgical treatment is usually effective in relieving pain and improving function.
Research on the Horizon
Scientists are currently investigating the genes that may be involved in Paget's disease. This work could enable doctors to predict who may be at risk for the disease and lead to new therapies to treat it.
The more details doctors can uncover about why the disease occurs, the better able they will be to develop treatments specific to Paget's disease. Eventually, doctors hope to reverse the effects on the bone, instead of just slowing them.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.