Diseases & Conditions
Morton's Neuroma
If you sometimes feel that you are "walking on a marble" and you have long-lasting pain in the ball of your foot (forefoot), you may have a condition called Morton's neuroma.
A neuroma traditionally refers to a benign (non-cancerous) tumor of nerve tissues. However, despite its name, Morton's neuroma is not a true tumor. Instead, Morton's neuroma is a thickening of the tissue surrounding one or more small nerves leading to the toes. This thickening can lead to pain, tingling, or discomfort in the forefoot that may limit your ability to do certain activities.
Anatomy of the Forefoot
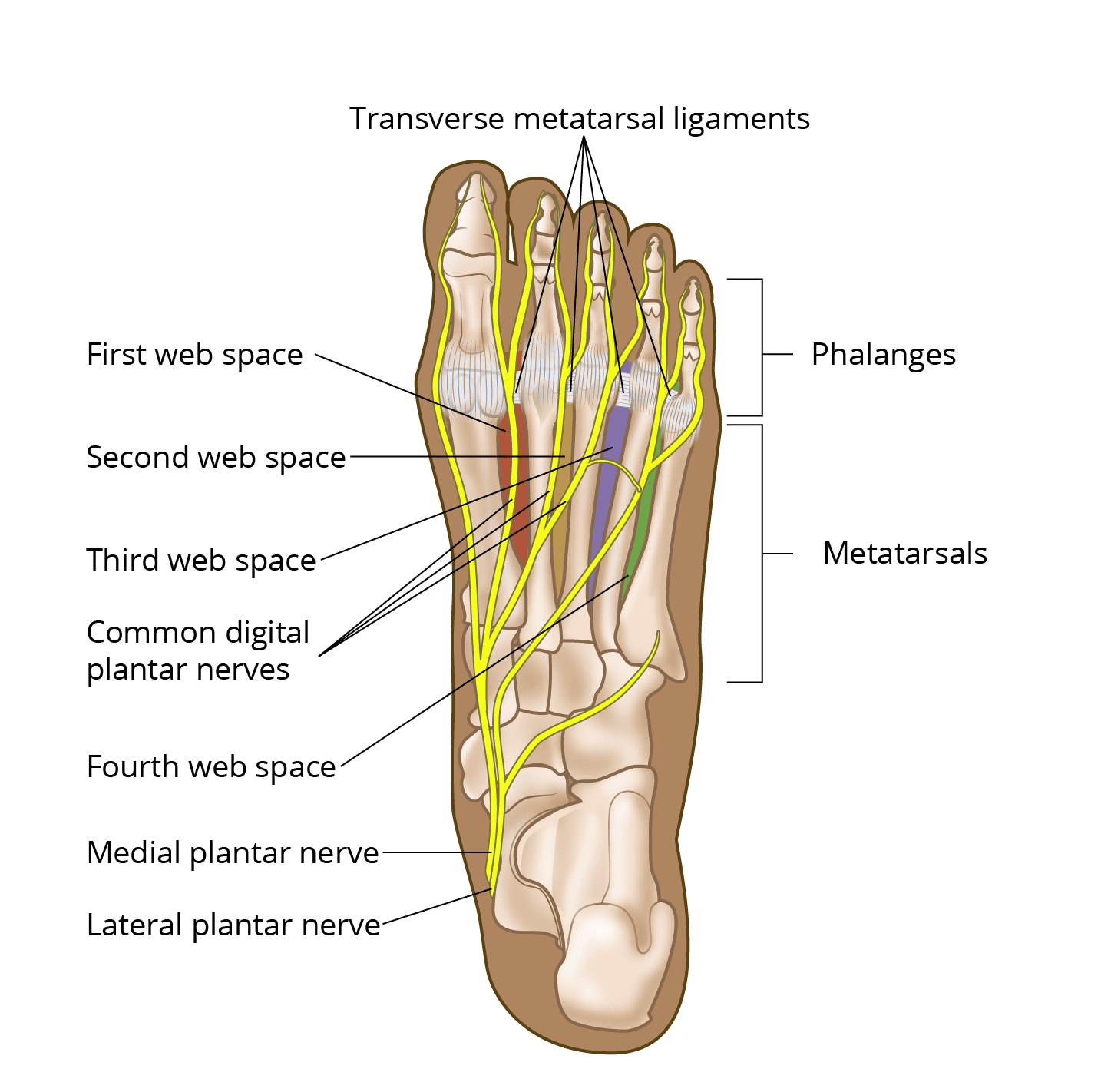
- The forefoot has 14 phalanges (toe bones) and five metatarsals (bones that connect the forefoot to the midfoot).
- The areas between the bases of the metatarsals, known as web spaces, are part of the forefoot. There are four web spaces:
- The first web space is located between the big toe and second toe.
- The second web space is located between the second and third toes.
- The third web space is located between the third and fourth toes.
- The fourth web space is located between the fourth and fifth (little) toes.
- The nerves that give sensation (feeling) to part of your toes are called the medial and lateral plantar nerves. These nerves travel along the bottom (plantar) part of your foot and branch out as they approach the toes.
- The nerve branches in the forefoot at the level of the web space are called common digital plantar nerves.
- In the web space, the rounded ends of the metatarsal bones are connected to each other by ligaments called transverse metatarsal ligaments. The common digital plantar nerves on the bottom of your foot pass underneath these ligaments in the web space.
Description
Although this condition is often called a Morton's neuroma, your physician or other sources may also refer to this condition as an interdigital neuroma, Morton metatarsalgia, interdigital neuritis, or a plantar neuroma (aka, degenerative compression neuropathy).
Morton's neuromas are around 8 times more common in women than men. They typically affect people between the ages of 30 and 60, though they can occur outside of this age range as well.
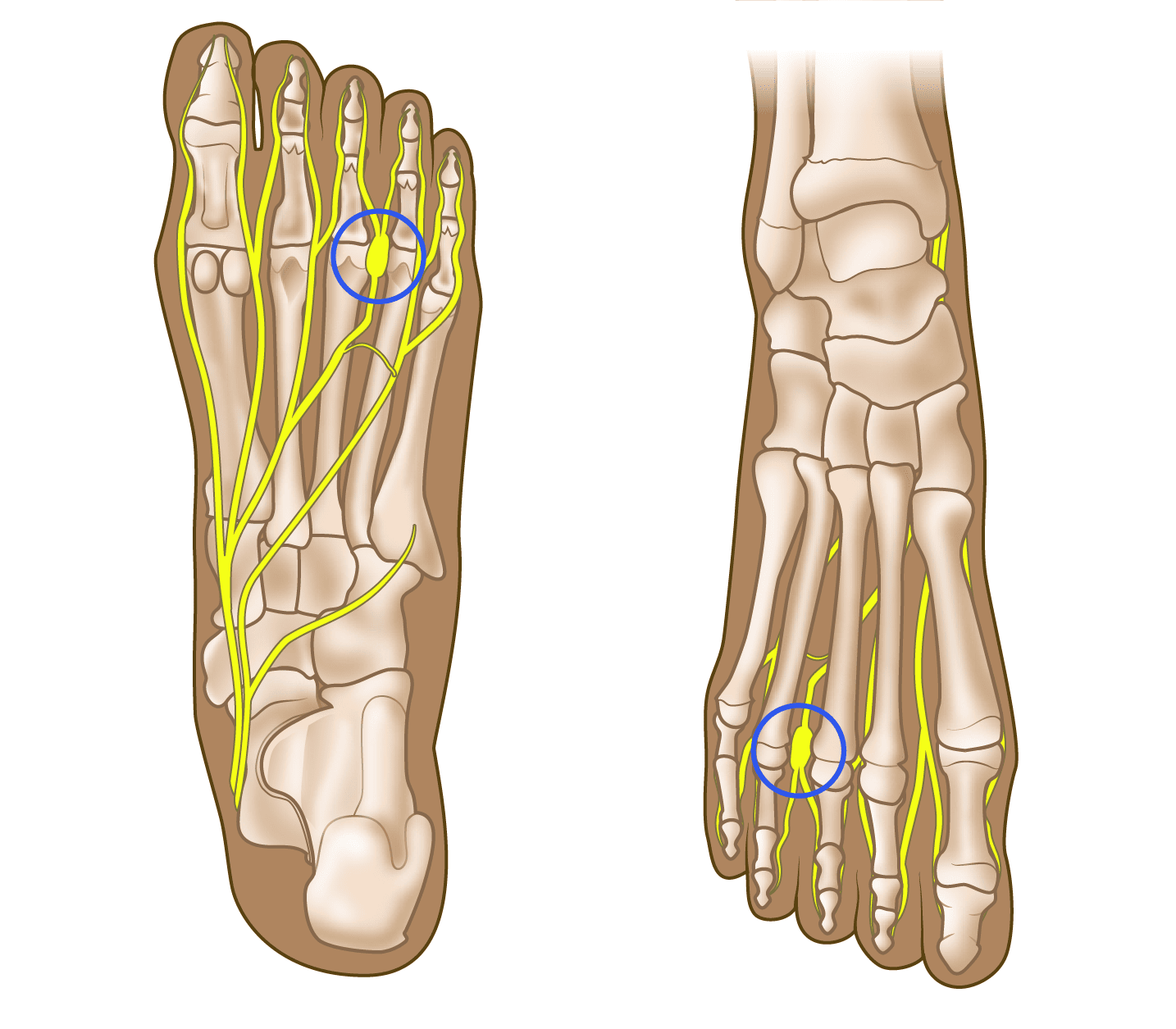
- Morton's neuroma most often develops in the area between the third and fourth toes — known as the third web space — usually in response to irritation, trauma, or extreme pressure.
- A Morton's neuroma can also develop in the second web space between the base of the second and third toes, though this happens less often.
The most common symptom is pain or discomfort in the ball of the foot (the area between the arches and toes on the bottom of the foot).
Cause of a Morton's Neuroma
The exact cause of a Morton's neuroma is not known, but current research suggests it is likely the result of entrapment (i.e., compression or squeezing) of the common digital plantar nerves. Compression of the nerve in the web space may trigger swelling and cause abnormal tissue to form in and around this nerve.
Symptoms of a Morton's Neuroma
Normally, there are no outwardly visible signs of a Morton's neuroma, such as a lump or skin discoloration.
These are the most common symptoms:
- You will experience persistent burning or sharp pain in the ball of the foot that may radiate (spread out) into the toes, especially during weightbearing activities like running or walking. Night pain is rare.
- Patients frequently describe the sensation of having a pebble or marble under their forefoot as they walk.
- Pain is typically in the third web space, but it can sometimes occur in the second web space.
- There may be numbness or an unpleasant tingling in the toes.
- Pain may worsen during activities that involve pushing off the forefoot, such as running. Sprinters with a Morton's neuroma may feel pain as they push off from the starting block.
- Problems with shoewear are common.
- High-heeled shoes, which put the foot in a similar position to the sprinter’s push-off, can aggravate the condition.
- Tight, narrow shoes also aggravate this condition by compressing the toe bones and pinching the nerve.
You should see an orthopaedic surgeon if you have continued pain, tingling, or discomfort in your forefoot.
Diagnosing a Morton's Neuroma
Medical History and Physical Examination
Your doctor will talk to you about your general health and medical history, including the location, nature, severity, and duration of your symptoms. It is important to also tell your doctor about specific activities that result in pain, as well as things that provide relief (e.g., rest, changing shoes, medication).
Your doctor will then perform a physical exam, including:
- Evaluating the skin of the foot and ankle for signs of excessive pressure points (areas that are painful to the touch).
- Checking the position of the toes and foot for common deformities that may also cause pain in the forefoot.
- Putting pressure on the spaces between the toes to try to pinpoint the specific site of the pain.
- Assessing range of motion of the toe joints, as well as other joints, to see if there is irritation that may suggest arthritis or joint inflammation as a cause of the pain.
- Possibly squeezing your foot to check for a click between your toes — called a "Mulder's click" — that is sometimes present with a Morton's neuroma.
- Applying direct pressure on the web space, usually with compression of the forefoot. This test is known as the web-space compression test, which often re-cretes the pain you experience from a Morton's neuroma.
- Injecting the affected web space with a local anesthetic. Not only can this technique relieve pain, but it can also confirm a Morton's neuroma diagnosis if the symptoms immediately go away.
Imaging Tests
X-rays may be required to rule out a stress fracture or arthritis of the joints that join the toes to the foot.
Ultrasound is the preferred method to check for abnormalities related to Morton's neuroma. An ultrasound can also be used to guide therapeutic injections for this condition.
Advanced imaging, such as an MRI, is usually not needed but may be considered in certain cases.
Nonsurgical Treatment for Morton's Neuroma
Initial management of a Morton’s neuroma typically involves one or more of the following:
- Changes in footwear. Avoid high heels and tight, narrow shoes; choose wider shoes (i.e., a wide toe box) with lower heels and a soft sole. This enables the bones to spread out and may reduce pressure on the nerve, giving it time to heal.
- Orthotics. Custom shoe inserts and metatarsal pads/bars can be added to your shoes. Redistributing pressure across the forefoot and separating the metatarsal bones reduces the pressure on the neuroma. This can help relieve irritation.
- Nonsteroidal anti-inflammatory drugs (NSAIDs). Medications such as ibuprofen or naproxen can be used to reduce inflammation associated with Morton's neuroma.
- Cortisone injection. One or more injections of a corticosteroid (steroid) medication can reduce the swelling and inflammation of the nerve, providing some relief. These injections may be done in the orthopaedic clinic, or you may be referred to a specialist who will perform the injection under the guidance of ultrasound.
- Nerve-targeting procedures. In some cases, minimally invasive treatments may be used to reduce pain by disrupting nerve signaling:
- Alcohol (ethanol) injections chemically ablate the nerve to reduce pain signals.
- Radiofrequency ablation uses heat to create a controlled lesion in the nerve to reduce pain signals.
- Cryoablation uses cold to temporarily disrupt nerve function. Long-term outcomes are still being studied.
- Alternative therapies (as add-ons to other treatments). Second-line treatments such as extracorporeal shockwave therapy and other non-steroid injections like platelet-rich plasma therapy could be considered. There is limited research showing that there may be a benefit from these treatments when they are used as add-ons to other treatments.
Studies have shown that many people can achieve long-term relief with a combination of shoe wear modifications, orthotics, anti-inflammatory medications (e.g., ibuprofen or naproxen), and/or corticosteroid injections.
Surgical Treatment for Morton's Neuroma
Despite the general effectiveness of conservative treatments for Morton's neuroma, some patients may continue to have symptoms. If your symptoms do not improve within 3 to 6 months, or if they come back, your surgeon may recommend surgery.
There are several surgical techniques to treat Morton's neuromas, and they have been shown to produce similar success.
To access the nerve, your surgeon can make an incision on either the top or bottom of the foot over the web space. After accessing the nerve, your surgeon may choose to do either:
- Decompression: Release tissue around the nerve to decompress it. This method potentially preserves sensation but has slightly less predictable outcomes than neurectomy. The use of this approach has become more popular among surgeons, since it spares the nerve and therefore limits sensation issues after surgery.
- Neurectomy: Remove the diseased portion of the nerve. This method can yield high pain relief but has risks. Risks after neurectomy include permanent numbness and a new neuroma formation called a stump neuroma.
There is an increasing trend of surgeons using a minimally invasive dorsal (top of the foot) approach that involves a smaller incision. This minimally invasive approach could lead to less disruption of soft tissues in the foot and often a faster recovery. Which approach your surgeon uses depends on many factors, and you should discuss the specifics of the procedure with your surgeon.
Recovery After Surgery for Morton's Neuroma
The recovery period after surgery for Morton's neuroma is short. Protocols differ, and you should follow the specific instructions of your operating surgeon.
- In general, you will be allowed to walk with your foot in a stiff-soled shoe, also known as a post-op shoe. However, you may be asked to put all your weight on your heel if the surgical incision was made on the bottom of your foot.
- You should avoid high-impact activities (running, jumping, etc.) and putting your foot underwater (such as in a bathtub or swimming pool) until your surgical wounds are completely healed — usually until at least 2 to 3 weeks after surgery.
Patients are commonly allowed to return to wearing normal shoes by 4 weeks after the procedure.
Surgery is often considered to be the most reliable form of treatment for a Morton's neuroma, with many studies showing an 80 to 95% long-term success rate.
Outcomes of Morton's Neuroma Treatment
- Conservative treatments, such as changes in footwear, activity modification, and the addition of orthotics, may provide some degree of relief in up to about 50% of patients.
- Corticosteroid injections provide short-term relief in about 50 to 70% of patients, though long-term relief is less common.
- Chemical nerve ablation and radiofrequency ablation also have a good success rate, with 70 to 80% of patients noting improvement after these interventions.
- Surgical intervention with neurectomy (removal of part of the nerve) or decompression of the nerve has the highest success rate, with most studies reporting an 80 to 95% success rate.
Even after successful surgical treatment, patients may experience issues.
- After a decompression, there may be persistent mechanical overload. This can lead to incomplete decompression, which may result in ongoing symptoms.
- After neurectomy, there is a possibility of permanent numbness.
- Additionally, there is a risk of forming a stump neuroma. Although the stump neuroma is not a true recurrence of Morton's neuroma, it can result in similar symptoms. As such, there is an increasing trend of choosing to use less invasive surgical approaches that preserve nerve function.
Around 5 to 20% of patients may have symptoms return and need additional treatment. Fortunately, a repeat surgery for return of Morton's neuroma symptoms has a similar success rate to the initial surgery (80 to 95%).
Summary
If you are experiencing any of the symptoms described above, you may benefit from an evaluation by an orthopaedic surgeon. Although Morton's neuromas can be quite bothersome, it is often possible to get relief. The condition typically responds well to current therapies, such as orthotics, injections, or surgery.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.