Diseases & Conditions
Metastatic Bone Disease
Cancer that originates in one area of the body, such as an organ, gland, or tissue, and then spreads to bone is called metastatic bone disease (MBD). Approximately 50% of cancers that start in an organ can spread (metastasize) to the skeleton.
With improved medical treatment of many cancers — especially breast, lung, and prostate — patients are living longer.
Every cancer patient should discuss their risk of developing MBD with an oncologist. Some cancers do not readily spread to bone, while others do.
The most common cancers that spread to bone include:
- Breast
- Lung
- Thyroid
- Kidney
- Prostate
MBD may cause pain in the area of spread, and it may lead to damage and weakness in the bone. The bone may become so weak that it may fracture with low demand activities or very minimal trauma. This can make it hard to participate in even simple activities like walking or standing As a result, losing quality of life is a big concern for patients with MBD.
How much of an effect MBD has on a patient will vary and is associated with how much the cancer has spread, which bones are affected, and the severity of the bone damage. There are various treatment options, however, that can help patients manage pain and maintain their independence and activity levels.
Description
After the lung and the liver, the skeleton is the most common site of spread for cancers that begin in organs. Metastases to the lung and liver are often not detected until late in the course of disease because patients don't experience symptoms. In contrast, bone metastases are generally painful when they occur.
Cancer most commonly spreads to these sites in the skeleton:
- Spine
- Pelvis
- Ribs
- Skull
- Upper arm
- Long bones of the leg
Bone Damage
Sometimes, the tumor will lead to destruction of the bone in a particular area. This process is called osteolytic bone destruction, and it is common in cancers that have spread to bone from the lung, thyroid, kidney, and colon.
Alternatively, new bone can form in response to the cancer spread. The new bone-forming, or osteoblastic lesions, causes the bone to become weak and deformed. Osteoblastic lesions are more frequently seen in spread of prostate, bladder, and stomach cancer.
Breast cancer often behaves in a mixed osteolytic and osteoblastic manner. Osteolytic and osteoblastic metastatic bone disease occur because the different cancer cells secrete factors that interact with the naturally occurring cells in the bone and cause bone destruction, new bone formation, or both.
Effects
Because MBD weakens the affected bones, people with this disease are at risk for fractures. Broken bones caused by MBD are called pathological fractures.
Sometimes the bone has not yet broken but is so weak that a break is imminent, which is referred to as an impending pathologic fracture. Patients with impending or actual fractures may be forced to remain on bedrest for long periods of time, which can lead to possible chemical imbalances in the blood such as increased calcium levels (hypercalcemia). Talk to your doctor about options to help prevent broken bones.
Patients with cancer that has spread to the spinal bones may develop nerve damage that can lead to paralysis or loss of the use of their legs and/or arms. This will often require surgery.
Symptoms
- Pain. The most common symptom of MBD is pain. Patients may have pain in the spine, pelvis, or extremities because the bone has been weakened by the tumor.
- Fractures. Weakened bones break more easily. A fracture from a minor injury is another possible sign of MBD.
- Anemia. The most common sites of spread — spine, pelvis, ribs, skull, upper arm, and long bones of the leg — correspond to areas of bone marrow that produce high levels of red blood cells, the cells responsible for carrying oxygen to tissues in the body. Anemia (decreased red blood cell production) is, therefore, a common blood abnormality in patients with MBD.
A cancer patient who experiences any pain, especially in the back, legs, and arms, should notify their doctor immediately. Pain that occurs without heavy activity (i.e., walking or lifting an object) is particularly concerning.
Diagnosis
Medical History and Physical Examination
It is important for your doctor to understand your medical condition and your symptoms. Your doctor will ask questions about the nature of any pain you are having, your current health, and your past medical conditions. The information your doctor learns is called your medical history.
After taking your medical history, your doctor will perform a physical examination, concentrating on the painful areas.
Imaging Tests
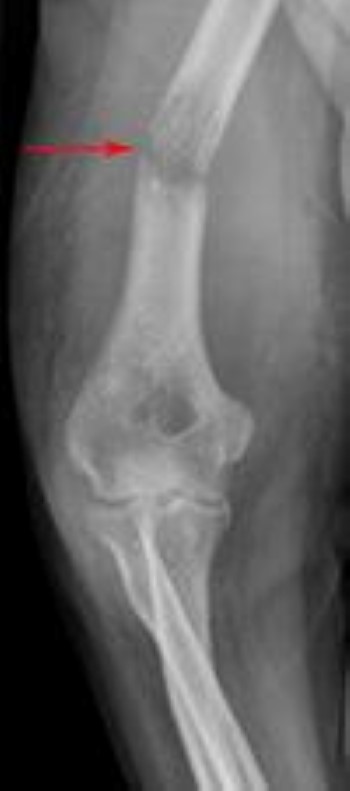
X-rays. After the interview and physical examination, your doctor will order X-rays if they suspect that you have MBD. Because some pain is referred from other areas (for example, experiencing knee pain after an injury to the hip), your doctor may order X-rays of bone beyond the areas where you are experiencing discomfort.
The X-ray examination can tell an oncologist a great deal of information about whether and how much of the bone is involved.
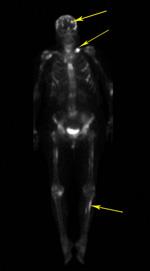
Other imaging tests. Your doctor may also order a whole body bone scan. This test is helpful in determining if other bones, in addition to the one in question, are involved with MBD. In select cases, your doctor may order a computerized tomography (CT) scan and/or magnetic resonance image (MRI), especially if the spine or pelvis may be involved.
MBD vs. Primary Bone Cancer
A diagnosis of metastatic bone disease should not be assumed unless a patient has a known primary cancer that has previously spread to bone.
If you are over the age of 45 with no personal history of cancer, and an X-ray detects a bone tumor, you should schedule a consultation with an orthopaedic oncologist (an orthopaedic surgeon who has advanced training in cancer surgery).
The orthopaedic oncologist will determine whether this bone tumor is a metastasis from an unknown primary cancer or is a primary bone cancer (sarcoma).
For example, if an area of bone has been destroyed, the possible diagnoses include metastatic bone disease or a primary bone cancer, such as myeloma or lymphoma. Cancers that begin in bone are much less common in adults over the age of 45. Other possible causes include diseases such as Paget's sarcoma, post-radiation sarcoma, hyperparathyroidism, and fractures due to osteoporosis. Additional tests will likely be needed to determine the exact diagnosis.
You may need to have a biopsy. This involves taking a piece of tissue from the tumor and looking at it under a microscope. This may be done in a clinic via a needle biopsy or, more commonly, as a small surgical procedure.
Ongoing Tests
Identifying MBD early is very important. The earlier the diagnosis, the more effectively treatments can help maintain function and quality of life.
Cancer patients should routinely be evaluated with certain tests, including:
- A complete blood count (CBC), because loss of red blood cells (anemia) is a frequent finding in metastatic bone disease or multiple myeloma.
- Blood chemistries (i.e., electrolytes, calcium, and alkaline phosphatase), as levels of certain substances may be abnormal in patients with widespread disease.
- An analysis of the urine (urinalysis) to detect blood, which may be present in patients with kidney cancer.
- Thyroid function, CEA, CA125, and prostate specific antigen (PSA) tests, which may be abnormal in patients with specific tumors.
- Serum and urine protein electrophoresis, which are important to exclude multiple myeloma.
Final Diagnosis
After the history, physical examination, X-ray, and laboratory tests are completed, your doctor will determine whether you have metastatic bone disease.
It is important to point out that many cancer patients have bone pain from certain types of chemotherapy, and that just because you have bone or joint pain, it does not mean you have MBD. Nevertheless, careful follow up is very important if you are having pain.
Treatment Options
In many cases of metastatic bone disease, the cancer has progressed to the point where multiple bony sites are involved. As a result, treatment is often focused on managing the symptoms of pain and bone weakness, and is not intended to be curative.
The most common treatment options for MBD include radiation, surgery, and medications to control pain and prevent further spread of the disease. Your doctor may also recommend surgery to stabilize bone that is weak or broken.
Patients with metastatic bone disease require a team approach to care. A medical oncologist works closely with an orthopaedic surgeon — who should be familiar with metastatic bone disease — and a radiation oncologist. Pain management specialists and social workers may also be part of your treatment team. Your medical oncologist and/or surgeon will determine which of these providers you should see for follow-up appointments.
Learn more about treatment options for metastatic bone disease for specific areas of spread.
Nonsurgical Treatment
Radiation
Radiation can be highly effective and is one of the most common therapies used to treat symptoms in patients with incurable MBD. By killing the cancer cells, radiation relieves pain, stops the tumor from growing and can prevent the bone from breaking.
Radiation can also be used to control the cancer after surgery to fix a broken bone. Research shows that radiation following surgery improves patient function and decreases the need for additional surgeries. Once a fracture occurs, however, surgery is usually performed prior to radiation.
MBD is a systemic (body-wide) problem and radiation therapy is unlikely to be curative. Before treatment, the doctor and patient should have a clear understanding of the goals of radiation therapy — whether it is to lessen symptoms and pain, or is intended to completely destroy disease in the affected bone.Therefore, the doctor must balance the potential benefits and risks of radiation for each patient.
Different cancers respond differently to radiation. Several types of radiation therapy are available.
Local field radiation. Local field radiation is the most common type of radiation used to treat MBD. In this procedure, radiation is directed at the metastatic tumor and the immediate adjacent tissue. Entire bone segments or multiple bones can be targeted by local field radiation, depending on how many areas are affected by the disease.
The primary goal of radiation treatment is to relieve pain with minimal side effects. Local field radiation typically results in complete pain relief in 50 to 60% of cases and partial relief in more than 80% of cases. How well MBD responds to radiation depends on many things, including cancer type (for example, breast cancer typically responds very well to radiation, while kidney cancer does not), and where the tumor is located.
Pain usually begins to subside in the first 1 to 2 weeks, but maximum relief may take several months. Therefore, your doctor will prescribe pain medication for you to take throughout the radiation treatment course.
Hemibody irradiation. This large-field radiation therapy is often used for patients with widespread metastatic disease. Rather than targeting specific bones, hemibody irradiation targets the larger areas of the upper body, midsection, or lower body.
Most metastatic cancer patients have multiple tumors. Hemibody irradiation is used to supplement local field radiation and may reduce the progression of widespread disease. It is used less frequently than local field radiation.
Radioisotope therapy. An alternative to hemibody irradiation, radioisotope therapy involves injecting a radioactive medicine (radiopharmaceutical) into a vein. The areas of metastatic bone disease absorb the radiopharmaceutical, which then kills the tumor cells. Compared to hemibody irradiation, radioisotope therapy is easier to give patients, and is also easier for patients to tolerate.
Medication Treatment
Medication treatment options for patients with MBD include:
- Chemotherapy. This treatment uses combinations of various drugs to destroy cancer cells. Because these drugs affect the entire system, healthy cells can also be damaged, including white blood cells and platelets. Chemotherapy is done in cycles with rest periods in between to let the blood cell count recover.
- Endocrine therapy. Also called hormone therapy, this drug treatment is used for types of cancer that are affected by hormones. Hormones are chemicals that are produced by glands in the body. In certain types of cancer, hormones can help cancer cells grow and spread, or they can destroy cancer cells and prevent them from growing. Treatment involves either increasing the levels of hormones or blocking hormone production. It is very common to receive endocrine therapy for breast and prostate cancers.
- Bisphosphonates. These drugs help prevent bone damage caused by tumors.They work by interfering with osteoclasts, the cells that are involved in the breakdown of bone. Bisphosphonates are also used to treat bone pain and elevated calcium levels in the blood (which can cause a variety of uncomfortable and dangerous health problems). Bisphosphonates can also help prevent future fractures.
Surgical Treatment
Surgery for MBD is used to treat or prevent broken bones. The goals are to relieve pain, reduce the need for pain medication, restore skeletal strength, and regain the ability to do daily activities.
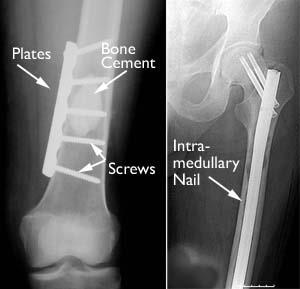
A broken or weakened bone must be carefully fixed in position and supported until it is strong enough to bear weight. During surgery, the tumor may be removed and the bone is stabilized with fixation devices, such as wires, plates, rods, pins, nails, and screws. Often, bone cement is placed into the defect created by the tumor to give added strength.
Research shows that patients who have surgery to prevent a break do much better than those who require surgery after a break occurs.
- They have shorter hospitalizations.
- They are more likely to be discharged to home (vs. being discharged to a skilled nursing or inpatient rehabilitation facility).
- They return more quickly to previous activities.
- They have improved survival and fewer surgical complications.
Surgery to reinforce the bones at risk for fracture also allows the medical oncologist and surgeon to coordinate surgical treatment and systemic therapy.
The decision to proceed with surgery is complex and individualized to each patient. Orthopaedic surgeons will consider several factors in determining whether a bone is at risk for breaking. These include whether the site is painful, the size of the tumor, and how the bone looks in an X-ray.
Potential Complications
Because patients with metastatic bone disease are generally less healthy than the average patient undergoing orthopaedic surgery and the surgery is more involved, there is an increase in the routine risks of surgery, including infection, bleeding, blood clots, and nerve damage.
Accordingly, the patient, family, surgeon, and oncologist must make a very careful, informed, cooperative decision about whether to proceed with surgery.
Conclusion
Advances in surgical techniques, radiation therapies, and medical therapies have significantly improved the quality of life for people suffering from cancer that has spread to the skeleton from its site of origin.
Treatment options for MBD are based on how much the cancer has spread, which bones are affected, and the severity of the bone damage. For more information on treatment options for MBD in specific areas of the skeleton (such as the upper arm or pelvis): Metastatic Bone Disease: Treatment Options for Specific Areas of Spread
To assist doctors in the treatment of metastatic carcinoma and myeloma of the femur, the American Academy of Orthopaedic Surgeons has conducted research to provide some useful guidelines. These are recommendations only and may not apply to every case. For more information: Treatment of Metastatic Carcinoma and Melanoma - Clinical Practice Guideline | American Academy of Orthopaedic Surgeons (aaos.org)
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.