Diseases & Conditions
Lipoma and Atypical Lipomatous Tumors
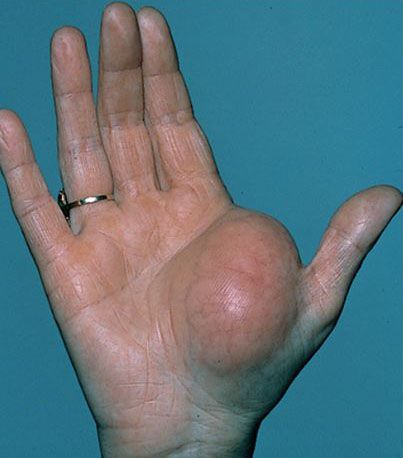
A lipoma is a benign (noncancerous) tumor made up of fat tissue. It is the most common soft tissue tumor found in adults.
- They are typically small, soft, rubbery lumps located just beneath the skin.
- They are usually painless.
- They are most often found on the upper back, shoulders, arms, buttocks, and upper thighs. Less commonly, these tumors can be found in deeper tissue of the thigh, shoulder, or calf.
- They most often appear between the ages of 40 and 60 years, although they can occur at any age.
- They occur slightly more often in men than in women.
- They do not typically change after they form, and have very little potential for becoming cancerous.
- They often require no treatment other than observation by you and your doctor. However, if a lipoma is painful or continues to grow larger, it can be removed with a surgical procedure.
It is possible to have more than one lipoma. This is called lipomatosis (many lipomas).
Atypical Lipomatous Tumors (ALT)
Atypical lipomatous tumors (ALT) are fatty tumors that can increase in size over time.
ALT is a relatively new term for large atypical fatty tumors in the extremities (arms or legs). ALTs were previously called well-differentiated liposarcoma (WDLS). This term was misleading, however; sarcomas are cancerous, and an ALT is not considered a cancer because it does not metastasize (spread to other parts of the body). WDLS still exist in the abdomen or retroperitoneum, as they typically behave more like a soft tissue sarcoma.
An ALT can be surgically removed, similar to a standard lipoma.
Types of Fatty Tumors
While all lipomas are made up of fat, there are subtypes based on the way they appear under a microscope. Some varieties include:
- Conventional lipoma (common, mature white fat)
- Hibernoma (brown fat, more commonly found in children)
- Fibrolipoma (fat plus fibrous tissue)
- Angiolipoma (fat plus a large amount of blood vessels)
- Myelolipoma (fat plus tissue that makes blood cells)
- Spindle cell lipoma (fat with cigar-shaped cells under the microscope)
- Pleomorphic lipoma (fat with cells of all different shapes and sizes)
- Intramuscular lipoma (fatty tumor that occurs within a muscle)
- Atypical lipomatous tumor (ALT) (deeper fat with a larger number of cells that can look atypical under the microscope. Doctors can use a specific genetic test called MDM2 to confirm the diagnosis.)
Cause
The cause of lipomas is not completely understood. Some subtypes (conventional lipomas, spindle cell lipomas, pleomorphic lipomas) appear to have a genetic cause and may be inherited from family members.
There has been no proven connection between the development of lipomas and any particular occupation or exposure to chemicals or radiation. Some doctors think that lipomas occur more often in inactive people.
Symptoms
- Lipomas are usually roundish masses that feel soft and rubbery.
- The lipomas just under the skin can be moved with gentle pushing.
- Lipomas do not typically hurt, although some of the subtypes can be painful, such as angiolipoma.
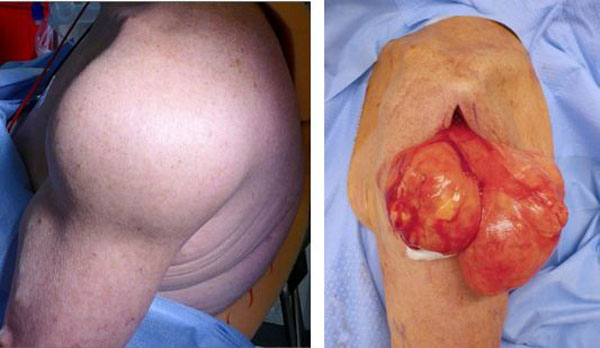
It often takes longer to notice lipomas that are in deeper tissue, and these tumors can be quite large by the time patients notice them and they are actually discovered.
Deeper lipomas, or intramuscular lipomas), also tend to be less mobile (meaning, you cannot move them with gentle pushing, as you can with lipomas that lie just under the skin).
Doctor Examination
Medical History and Physical Examination
Before a physical examination, your doctor will:
- Talk with you about your general health, as well as your current condition.
- Get a thorough history of the problem from your perspective, particularly how long the mass has been there and which symptoms — such as pain — are associated with it.
During the physical examination, your doctor will:
- Feel the mass, checking its size and consistency, as well as its mobility
- Examine the skin overlying the mass, looking for any changes
Tests
Doctors can usually diagnose lipomas based on history and physical examination alone. However, imaging tests can be helpful for some cases.
X-rays. Although X-rays are best known for their ability to create clear pictures of dense structures like bone, plain X-rays can also show a prominent shadow caused by a soft tissue tumor, such as a lipoma.
Computerized tomography (CT) scans. CT scans are more detailed than X-rays and will often show a fatty mass to confirm the diagnosis of lipoma.
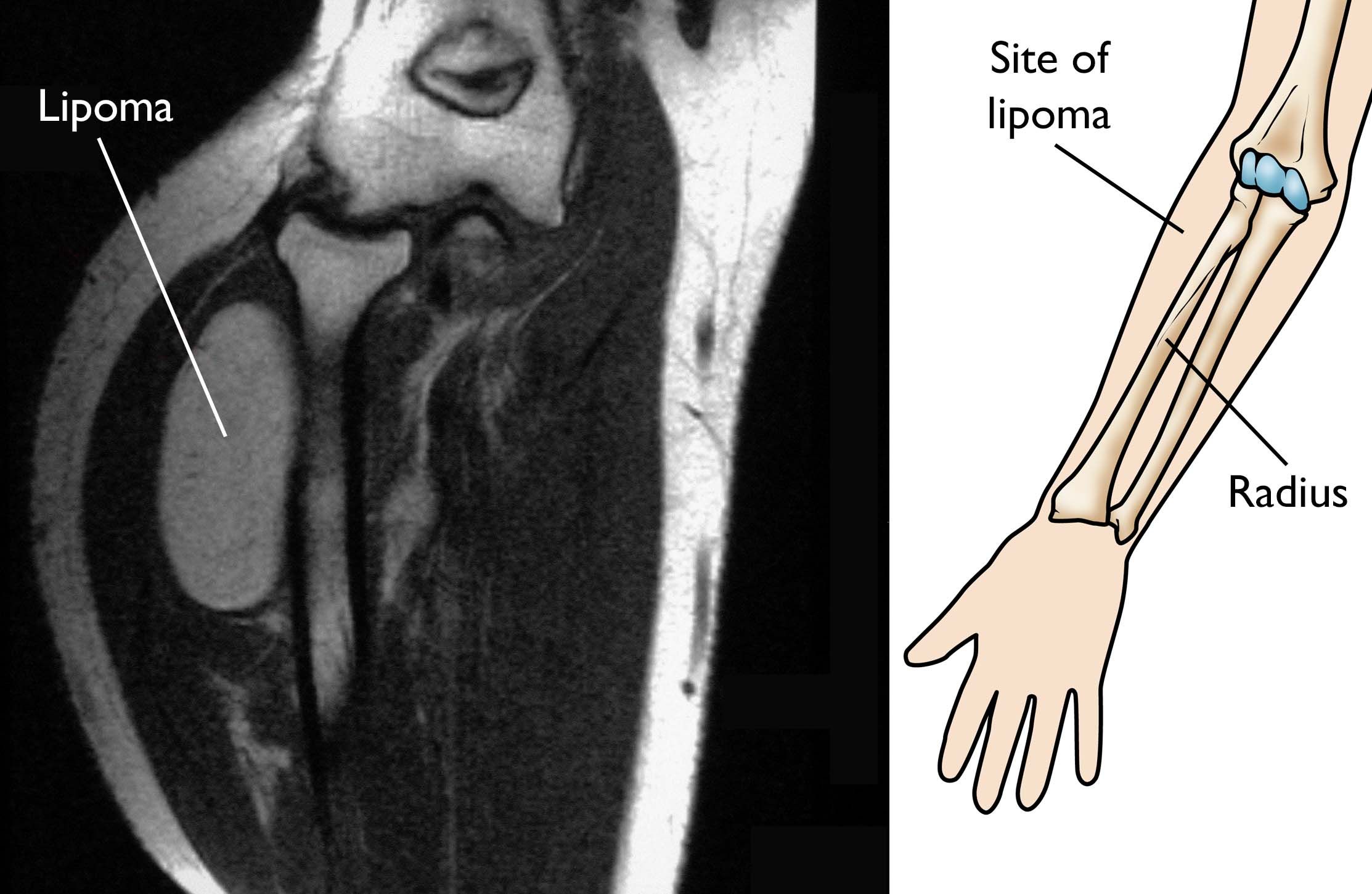
Magnetic resonance imaging (MRI) scans. The best information for diagnosing lipomas comes from an MRI scan, which can create better images of soft tissues like a lipoma than an X-ray can. MRI scanning will show a fatty mass from all perspectives. Often, doctors can make the diagnosis of lipoma based on MRI imaging alone, and a biopsy is not required.
Biopsy. A biopsy is not often recommended for a lipoma if the MRI images show that the mass is made up of fatty tissue. If there are certain areas of the tumor that look unusual, a biopsy is sometimes necessary to confirm the diagnosis.
In a biopsy, a tissue sample of the tumor is taken and examined under a microscope. Your doctor may give you a local anesthetic to numb the area and take a sample using a needle. Biopsies can also be performed as a small operation.
After the lipoma is removed, a pathologist will analyze the tumor. Under a microscope, lipomas often have a classic appearance, with a lot of mature fat cells.
Liposarcoma. During the diagnosis phase, your doctor will work to determine whether the tumor is a lipoma or a more aggressive form of fatty tumor called liposarcoma.
- While lipomas and atypical lipomatous tumors are not considered cancerous, liposarcomas are cancerous.
- The symptoms of liposarcoma vary from those of lipoma. Liposarcomas typically grow quickly and are not as moveable as lipomas.
People with lipomas are not more likely to develop a fatty cancer in the future.
Treatment
Observation
Because lipomas are benign (not cancerous) tumors, no treatment may be an option, depending on your symptoms. If you choose no treatment, it is very important that you see your doctor for regular visits to monitor any changes in the tumor. This is sometimes called "watchful waiting."
Surgical Excision (Removal)
If the fatty tumor is painful, bothersome, or interfering with daily activities, surgery can be considered.
Procedure. Surgical excision is performed through an incision over the tumor.
- Small tumors (<5 cm) can be removed in an in-office procedure with local anesthetic to numb the area.
- Typically, large lipomas (>5 cm) or those that are deep require a trip to the operating room. Based on patient and surgeon preference, you may be given regional anesthesia, general anesthesia, or both. Regional anesthesia numbs a large area by injecting numbing medicine into specific nerves. General anesthesia puts you to sleep.
Recovery. Most commonly, surgical excision is an outpatient procedure, meaning you go home the same day. Most surgeons recommend light activities for 2 to 4 weeks following surgery to allow for wound healing and full recovery. Your doctor will provide you with specific instructions to guide your recovery.
Recurrence. The chances of the tumor growing back depend on the type of tumor.
- Lipomas are almost always cured by simple excision. It is unusual for a lipoma to grow back. If a lipoma does come back, excision is again the best treatment option. Surveillance is not needed once a lipoma is removed.
- Atypical lipomatous tumors can more frequently grow back. Most surgeons recommend some sort of surveillance after tumor removal. This usually involves a physical exam and imaging every 6 to 12 months.
Research
There is ongoing research to learn more about the various subtypes of lipomas and why they form in the first place. In the future, there may be specific treatment recommendations for various lipoma subtypes.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.