Diseases & Conditions
Discoid Meniscus
The meniscus is a wedge-shaped piece of cartilage that sits in between the bones of the knee and acts as a cushion to protect the bones during movement. Each knee has two menisci.
Healthy menisci are shaped like crescent moons (in fact, "meniscus" comes from the Greek word for crescent). A discoid meniscus is thicker than normal, and often oval or disc-shaped. It is more prone to injury than a normally shaped meniscus.
People with discoid meniscus may go through their entire lives and never experience any problems. If a discoid meniscus does not cause pain or discomfort, no treatment is needed. Some people, however, will have knee problems related to the discoid meniscus. Symptoms often begin during childhood.
Anatomy
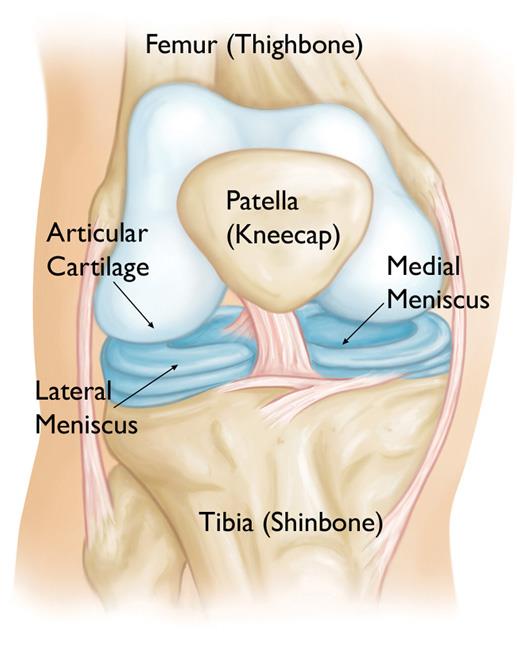
The meniscus acts as a shock absorber between your femur (thighbone) and tibia (shinbone). It protects the thin articular cartilage that covers the ends of the bones and helps the knee to easily bend and straighten.
There are two menisci in the knee: the medial meniscus on the inside of the knee, and the lateral meniscus on the outside.
The menisci are attached to the femur bone by a strong tissue called the meniscofemoral ligament. This ligament also provides a blood supply to a small portion of the meniscus.
Description
In many cases, a discoid meniscus is shaped like a half-moon or complete circle, rather than a crescent moon. It most often occurs on the lateral side (outside) of the knee and can sometimes be found in both knees.
Types of Discoid Meniscus
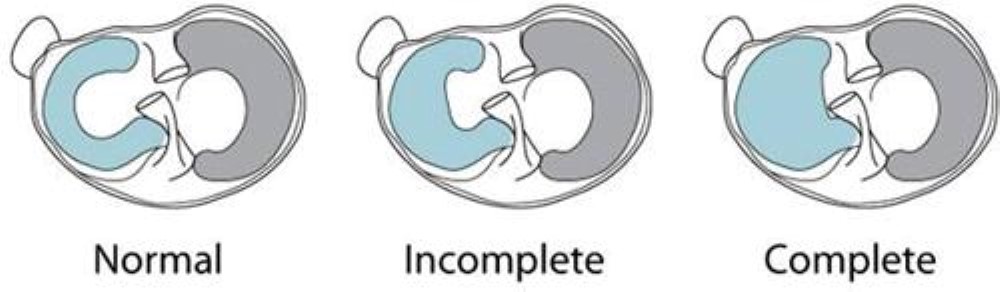
There are three types of discoid menisci:
- Incomplete. The meniscus is slightly thicker and wider than normal.
- Complete. The meniscus completely covers the tibia.
- Hypermobile Wrisberg. This occurs when the ligaments that attach the meniscus to the femur and tibia are not there. Without these ligaments, even a fairly normally shaped meniscus can sometimes move around in the joint and cause pain, as well as locking and popping of the knee.
Discoid Meniscus Injuries
A discoid meniscus is more prone to injury than a normal meniscus. The thick, abnormal shape of a discoid meniscus makes it more likely to get stuck in the knee or to tear. If the meniscofemoral ligament attachment to the femur is also missing, the risk for injury is even greater.
Once injured, even a normal meniscus is difficult to heal. This is because the meniscus lacks a strong blood supply and the nutrients that are essential to healing cannot reach the injured tissues.
In many cases of discoid meniscus, patients experience symptoms without there being any injury to the meniscus.
Cause
Discoid meniscus is a congenital (present at birth) defect.
Injuries to the discoid meniscus often occur with twisting motions to the knee, such as during sports that require pivoting or fast changes in direction.
Symptoms
The most common symptoms of a discoid meniscus or torn discoid meniscus are:
- Pain
- Stiffness or swelling
- Catching, popping, or locking of the knee
- Feeling that the knee is "giving way"
- Inability to fully extend (straighten) the knee
Doctor Examination
Medical History and Physical Examination
After discussing your child's medical history and any events that occurred before symptoms started, the doctor will examine your child's knee.
Your child may or may not have tenderness where the bones meet.
To test for discoid meniscus, the doctor will twist your child's knee with the knee bent and straightened. In many cases of discoid meniscus, there is a popping or clunking sensation. This can sometimes even be heard. In extreme cases, part of the meniscus will pop out of the knee joint and can be seen right under the skin.
Imaging Tests
X-rays. Although X-rays do not show tears of soft tissues like the meniscus, they can show whether there are other problems in the knee. In addition, because the discoid meniscus is so thick, the space between the femur and tibia on the lateral part of the knee may appear widened on an X-ray.
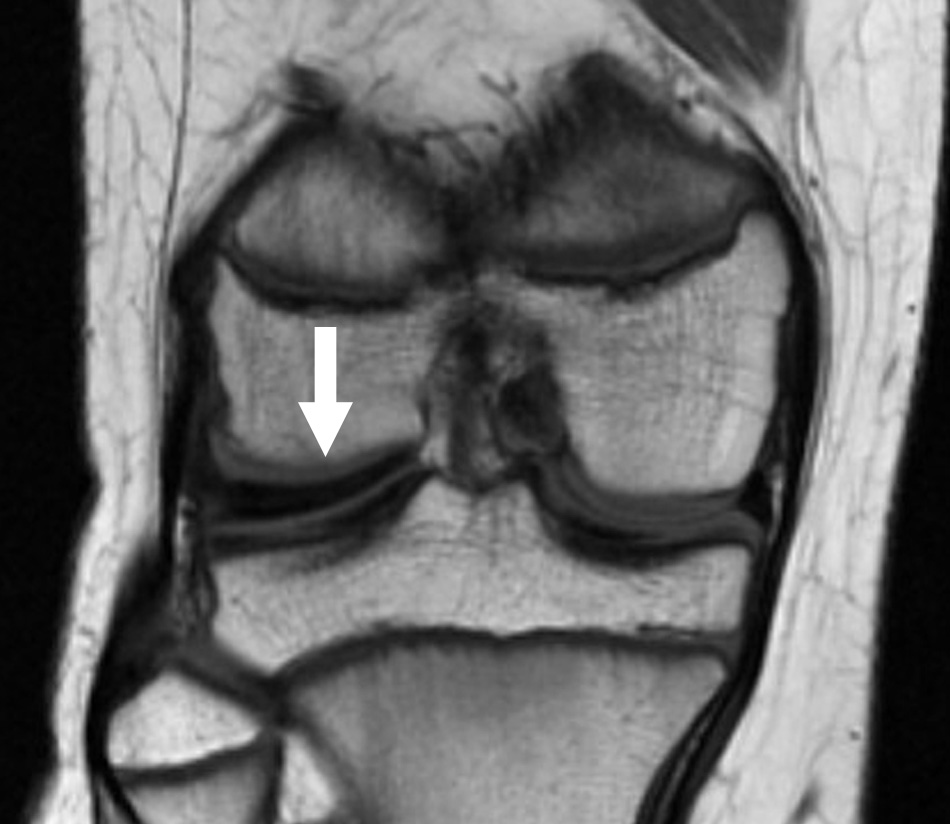
Magnetic resonance imaging (MRI) scan. An MRI scan creates detailed images of the soft tissues of the knee joint and is, therefore, the best imaging test for discoid meniscus.
The MRI can show the abnormal shape of the discoid meniscus, as well as tears within the meniscus. However, the rare Wrisberg type of discoid meniscus cannot be diagnosed with an MRI scan because the problem only occurs when the patient is moving.
An MRI involves lying still for 30 to 45 minutes. Many young patients require some sedation or anesthesia to complete the test.
Treatment
Sometimes, a doctor discovers a discoid meniscus when evaluating the knee for a different problem. If the discoid meniscus is not causing any symptoms, specific treatment for it may not be necessary.
When a discoid meniscus is causing pain, popping, or other symptoms, however, your child's orthopedic surgeon will probably recommend arthroscopic surgery.
Surgical Treatment
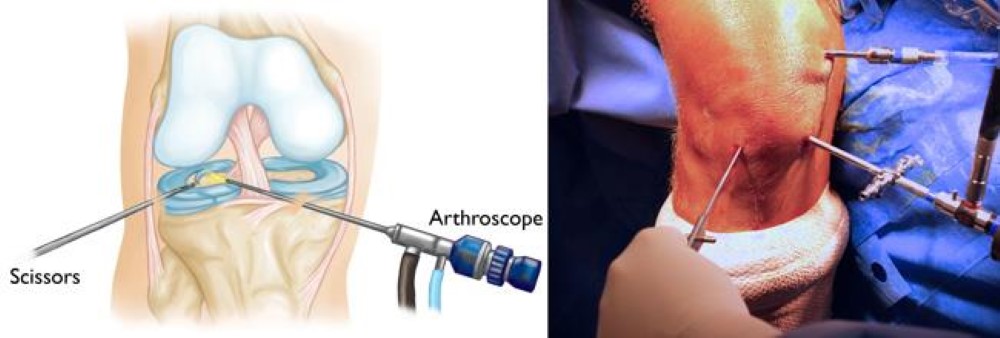
Knee arthroscopy is one of the most commonly performed orthopaedic surgical procedures.
During arthroscopy, the surgeon makes a few small incisions around the knee and inserts a small camera, called an arthroscope, into the joint. The camera displays pictures on a video monitor, and the surgeon uses these images to guide miniature surgical instruments.
Most arthroscopic surgeries are done on an outpatient basis. Patients usually go home a few hours after the procedure.
Anesthesia. To prevent pain during the procedure, the patient is given anesthesia. There are different types of anesthesia:
- Local and regional types of anesthesia numb just parts of the body, and the patient remains awake.
- General anesthesia puts the patient to sleep. Most children are given general anesthesia for arthroscopic surgery.
Surgical Procedure. Treatment will depend upon the type of discoid meniscus.
- Complete and incomplete discoid menisci with no tears are typically treated with saucerization, a procedure in which the meniscus is cut and re-shaped into a crescent.
- If the discoid meniscus is also torn, the surgeon may perform a saucerization and then trim away the torn portion. Some tears can be repaired with stitches, rather than removed.
- The hypermobile Wrisberg form of discoid meniscus is saucerized if necessary, then stabilized with stitches to sew the meniscus to the lining of the joint.
Rehabilitation
- After surgery, the doctor may put your child's knee in a brace or a soft bandage wrap.
- Your child may need to use crutches for a short period of time. Very young children may need a wheelchair for several weeks because they do not have the balance or strength to use crutches.
- Once the initial healing is complete, your child's doctor may prescribe physical therapy exercises to restore strength and mobility. These may be done at home or with a physical therapist.
Recovery
Most patients return to normal daily activities after arthroscopy for a discoid meniscus. However, if the entire meniscus was removed, there is a risk for continued pain and, potentially, early arthritis.
Surgeons sometimes recommend that patients avoid sports that overstress the knee with cutting type movements. These include soccer, tennis, basketball, and football.
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.