Diseases & Conditions
Anterior Cruciate Ligament (ACL) Injuries
The following article provides in-depth information about anterior cruciate ligament injuries. The article Anterior Cruciate Ligament (ACL) Injury: Does It Require Surgery? provides in-depth information about treatment for ACL injuries and is recommended as a follow-up to this article.
An anterior cruciate ligament (ACL) tear, or rupture, is one of the most common knee injuries. It affects more than 200,000 people annually in the U.S. and represents more than 50% of all knee injuries.
Anyone can tear their ACL, but the injury most often occurs when a person is pivoting, cutting, or jumping with their leg fully straightened on impact with the ground. These movements are common in activities like volleyball, soccer, football, and basketball.
Interestingly, most ACL injuries happen without direct impact to the knee. It is a matter of power imbalance: The ACL is overwhelmed by the sudden extreme forces associated with these movements and it cannot stabilize the abrupt forces through the knee joint.
If you injure your ACL, you may need surgery to regain full function of your knee. This will depend on several factors, such as the severity of your injury, your age, how much joint degeneration (wear and tear) you have, whether you feel instability in your knee, and your activity level.
Anatomy of the Knee
Bones
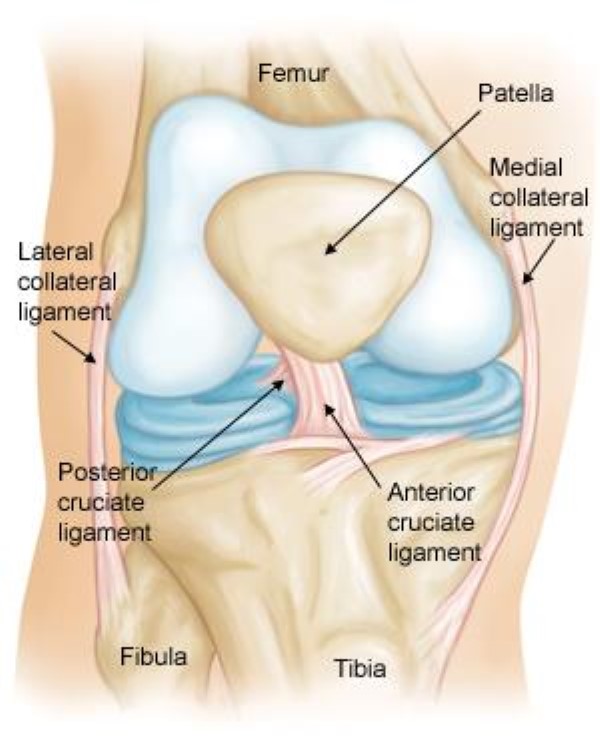
Three bones meet to form the knee joint:
- The femur (thighbone), which sits above the knee
- The tibia (shinbone), which sits below the knee
- The patella (kneecap), which sits in front of the joint
Bones are connected to other bones by ligaments. There are four primary ligaments in your knee. They act like strong ropes to hold the bones together and keep your knee stable.
Ligaments
Collateral ligaments. These are found on the sides of your knee. The medial collateral ligament (MCL) is on the inside, and the lateral collateral ligament (LCL) is on the outside. They control the side-to-side motion of your knee and brace it against unusual movement.
Cruciate ligaments. These are found inside your knee joint. They cross each other to form an X, with the ACL in front and the posterior cruciate ligament (PCL) in back. The cruciate ligaments control the front and back motion of your knee.
- The ACL runs diagonally in the middle of the knee. It prevents the tibia from sliding out in front of the femur and provides rotational stability to the knee.
- The PCL keeps the shinbone from moving backward too far. It is stronger than the ACL and is injured far less often.
Cartilage
The ends of the femur and tibia, and the back of the patella are covered with articular cartilage. This slippery substance helps your knee bones glide smoothly across each other as you bend or straighten your leg.
Meniscus
Two wedge-shaped pieces of fibrocartilage act as shock absorbers between the femur and tibia. These are menisci. The menisci help to transmit force from one bone to another and play an important role in knee stability and smooth joint motion.
Commonly, people who tear their ACL will also suffer a meniscal tear on the outside of their knee.
Tendons
Bones are connected to muscles by tendons. These are fibrous connective tissues that allow for joint movement and provide stability. The role of all the tendons is to transfer force from muscles to bones. Although the quadriceps tendons are not directly affected when you tear your ACL, their stability and strength play an important role in both ACL tear recovery and future injury prevention.
Description
A "torn ACL" refers to the rupture of the ligament. This can happen within the ligament itself or at the point where the ligament connects to bone. A rupture occurs when the force applied to the ligament is too much for the ligament to bear.
Injuries to the ACL often occur along with damage to other structures in the knee, such as the MCL, lateral meniscus, and medial meniscus. It is important to identify if you have any related injuries so you and your surgeon can make informed decisions about your treatment and ensure the best possible outcome.
Classification of ACL Tears
Injured ligaments are classified on a three-grade sprain system based on the degree of injury to the ligament. Your doctor will use a magnetic resonance imaging (MRI) scan to see how much ligament damage there is.
Grade 1 Sprains. The ligament is mildly damaged. It has been slightly stretched but is still able to help keep the knee joint stable. The ACL is intact.
Grade 2 Sprains. A Grade 2 sprain stretches the ligament to the point where it becomes loose. This is often referred to as a partial tear of the ligament.
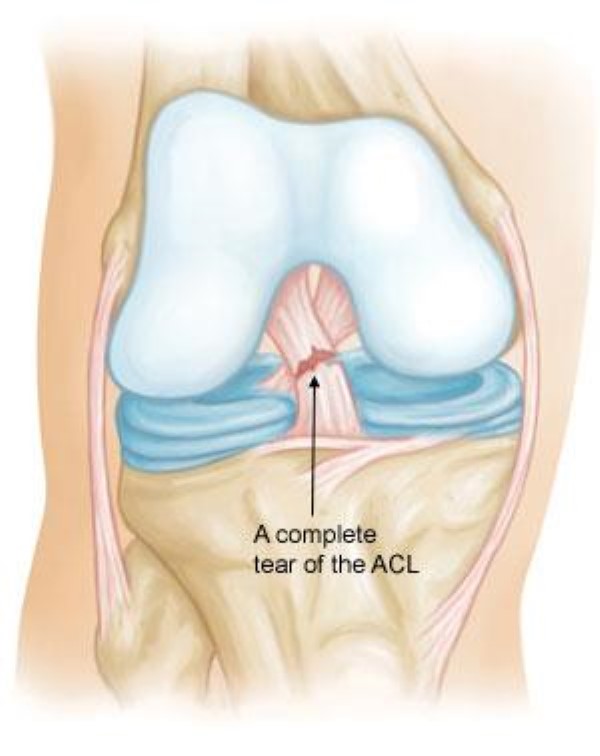
Grade 3 Sprains. This type of sprain is most commonly called a complete tear of the ligament. The ligament has been torn in half or pulled directly off the bone. The knee joint is unstable.
In addition, the ACL Injury Severity Scale (ACLISS) documents any damage to the meniscus, cartilage, bones, and/or other ligaments that happened at the same time as the ACL tear.
Risk Factors for ACL Tears
- Being female. Female athletes experience ACL injuries at rates 2 to 8 times higher than males. This may be due to differences in knee morphology, biomechanics, and hormonal influences. Other suggested causes include differences in pelvis and leg alignment.
- Having a higher body mass index (BMI)
- Having more joint laxity (looser joints)
- Being younger
- Decreased lower leg strength
Causes of ACL Tears
The ACL can be injured in several ways:
- Changing direction rapidly
- Stopping suddenly
- Slowing down while running
- Landing from a jump incorrectly
- Direct contact or collision, such as a football tackle
Symptoms of an ACL Tear
When you injure your anterior cruciate ligament, you might hear a popping noise, and you may feel your knee give out from under you. Other typical symptoms include:
- Pain with swelling. Within 24 hours, your knee will swell. The swelling and pain may go away on their own. However, returning to normal activities often worsens the feeling of instability and risks further damage to the surrounding structures in your knee.
- Loss of full range of motion.
- Tenderness along the joint line.
- Discomfort while walking.
Diagnosing an ACL Tear
Physical Examination and Patient History
During your clinic visit, your doctor will ask about the following:
- The specific movement or impact that caused the injury
- Your current symptoms (swelling, bruising, etc.)
- What you have tried to help manage your symptoms and what has worked
During the physical examination, the physician will check all the structures of your injured knee and compare them to your non-injured knee. Often, this will be enough to diagnose your injury, but advanced imaging is usually included to remove any uncertainty and evaluate for other possible injuries.
Imaging Tests
X-rays. X-rays do not specifically show ligament injuries. However, they are a quick and useful tool for identifying any related injury to bone. When an ACL tears at the spot where it attaches to bone, it sometimes pulls away a small piece of bone. This is called an "avulsion fracture." The piece of bone can be seen on an X-ray.
Magnetic resonance imaging (MRI) scan. An MRI offers the best view of your injured ligaments or cartilage. An MRI is not required to make the diagnosis of a torn ACL, but it allows your doctor to look for injuries to other soft tissue structures in the knee (e.g., meniscus, cartilage). It also offers better insight into the severity of the ACL injury.
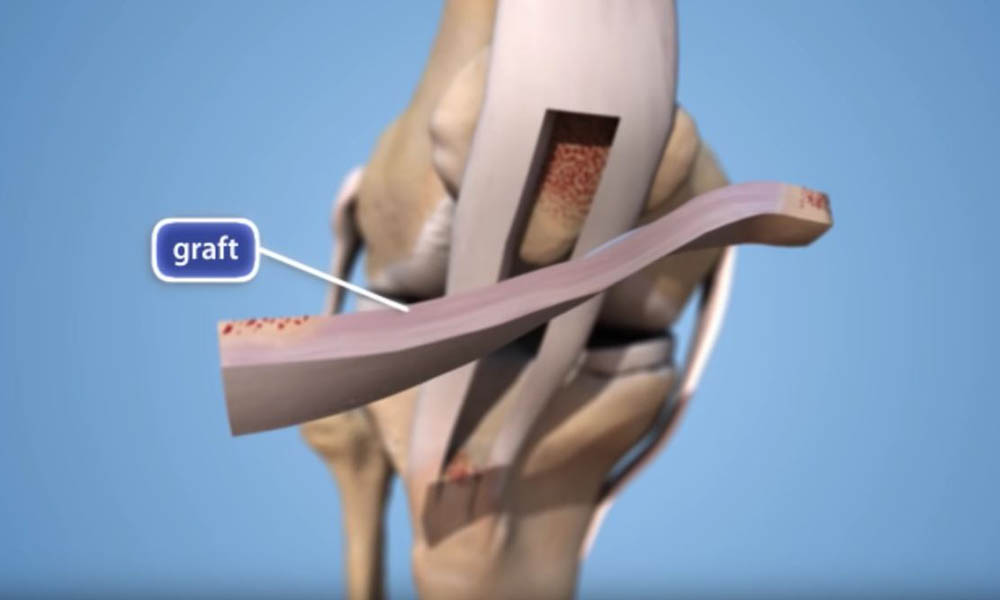
Treatment for an ACL Tear
Treatment for an ACL tear will depend on the patient's individual needs and desired goals for recovery. Non-operative management is always an option. It includes reducing inflammation with medications and working with physical therapy to gradually rebuild quadriceps strength and confidence in your knee.
The decision about whether to have surgery begins with a conversation between you and your orthopaedic surgeon to establish goals, review surgical options, and optimize post-surgery recovery plans.
Broadly, surgical options include repair or reconstruction. Reconstruction remains the most common surgical treatment. Repair is typically reserved for:
- Tears close to where the ligament attaches to the bone
- Partial tears that are causing symptoms
Your surgeon will help you determine which treatment option is best for you.
Continue to the next page: ACL Injury: Does It Require Surgery?
To assist doctors in the management of anterior cruciate (ACL) ligament injuries, the American Academy of Orthopaedic Surgeons has conducted research to provide some useful guidelines. These are recommendations only and may not apply to every case. For more information: Plain Language Summary - Clinical Practice Guideline - Anterior Cruciate Ligament Injury - AAOS
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.