Diseases & Conditions
Ankle Fractures (Broken Ankle)
A broken ankle is also known as an ankle fracture. This means that one or more of the bones that make up the ankle joint are broken.
A fractured ankle can range from:
- A simple break in one bone, which may not stop you from walking, to
- Several fractures, which may require one or more surgeries. These types of fractures can be very disabling. In some cases, you may not be able to put weight on your ankle for a few months. Some fractures are so severe that you may have permanent changes affecting your ability to walk, drive, play sports, and work.
Although ankle fractures can occur in people of all ages, they typically happen more often in adults; in fact, they are the fourth most common type of fracture in adults.
Anatomy of the Ankle
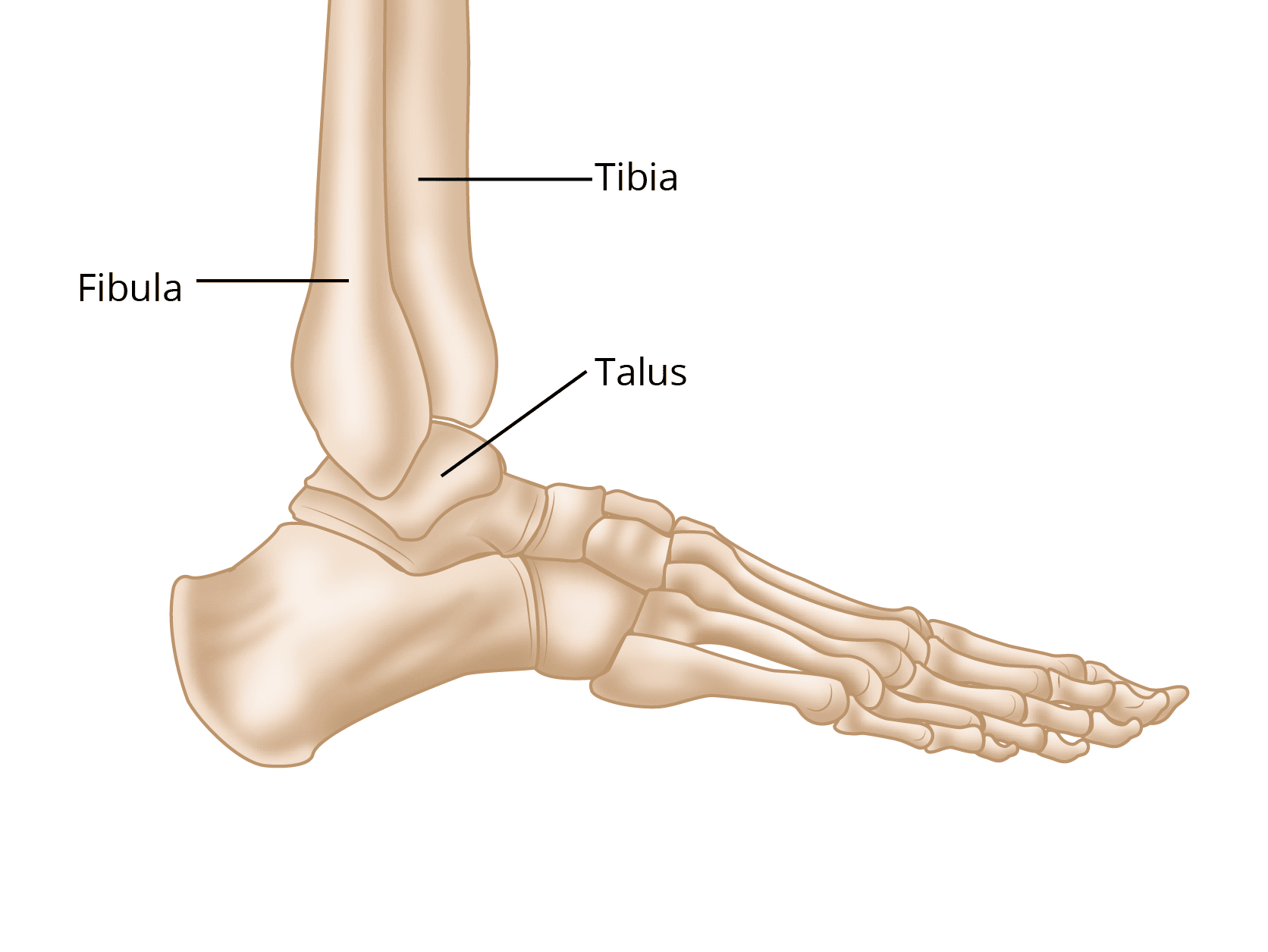
Three bones make up the ankle joint:
- Tibia — the shinbone
- Fibula — the smaller bone of the lower leg
- Talus — the small bone that sits between the heel bone (calcaneus) and the tibia and fibula
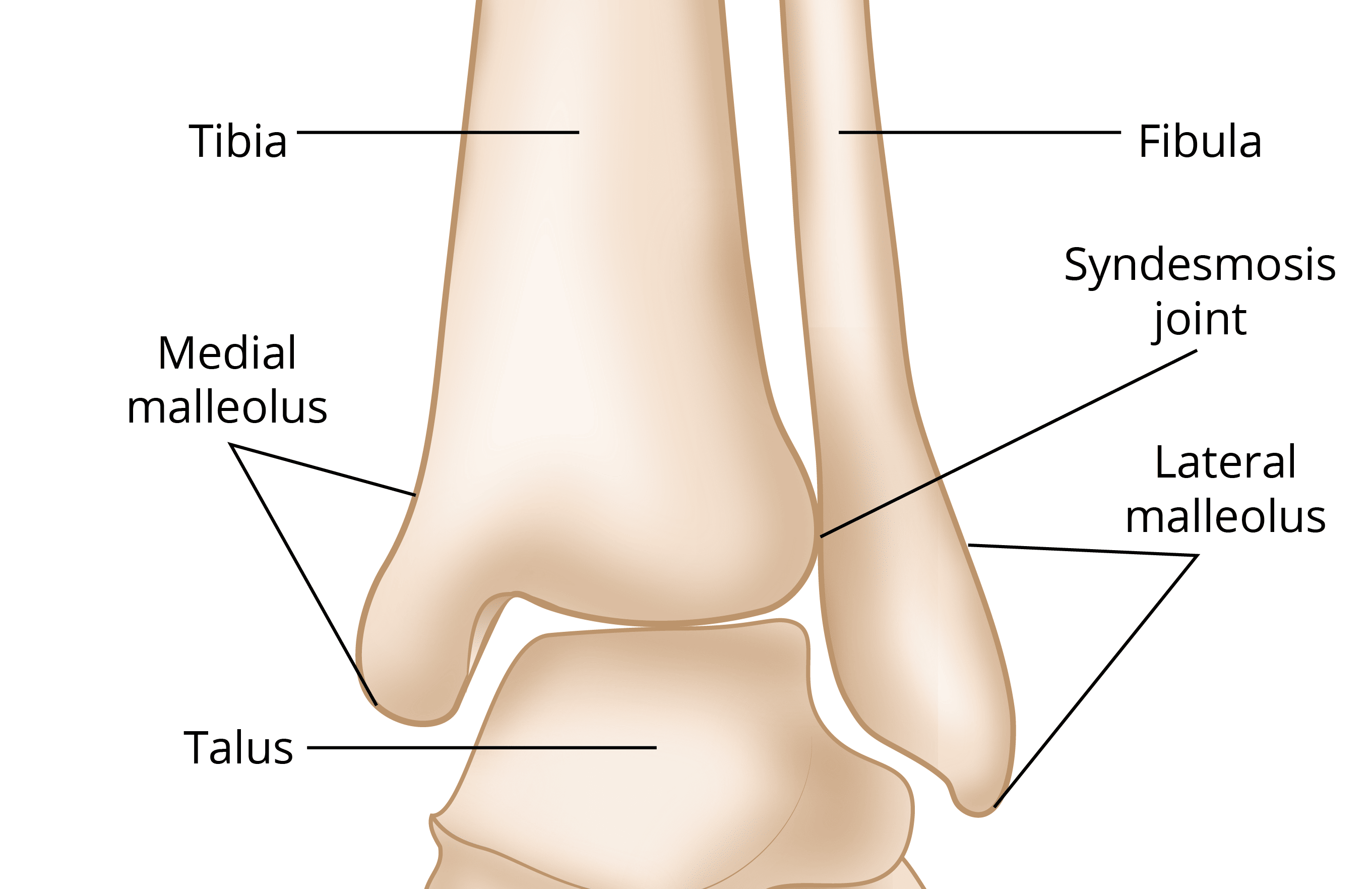
The tibia and fibula have specific parts that make up the ankle:
- Medial malleolus — the small prominent bone on the inner side of the ankle at the end of the tibia
- Posterior malleolus — the back part of the tibia
- Lateral malleolus — the prominent bone on the outer side of the ankle at the end of the fibula
Doctors classify ankle fractures according to the area of the bone that is broken. For example:
- A fracture at the end of the fibula is called a lateral malleolus fracture.
- If both the tibia and fibular are broken at the inside and outer side of the ankle, it is called a bimalleolar fracture.
- A trimalleolar fracture is if the medial malleolus, lateral malleolus, and posterior malleolus are broken.
- Sometimes, the breaks are so severe that the entire weightbearing part of the tibia bone at the joint is broken. This is a special type of ankle fracture called a pilon fracture.
Two joints are involved in ankle fractures:
- Ankle joint — where the tibia, fibula, and talus meet
- Syndesmosis joint — the joint between the tibia and fibula, which is held together by ligaments
Types of Ankle Fractures
Fractures can also be classified (described) by how much the pieces of bone have moved out of their normal position.
- Nondisplaced fracture. A nondisplaced ankle fracture is where the bones are not out of place. These fractures may not require surgery.
- Displaced fracture. A displaced ankle fracture is where the broken bone fragments are separated. There may be breaks in one, two, or three areas, and the ankle joint may also be dislocated. Most ankle fractures with dislocations require surgical treatment.
- Open fracture. When the broken bones break through the skin, the injury is called an open, or compound, fracture. An open fracture is an emergency and you should seek care right away. This is because an open wound allows outside material, dirt, and debris to contaminate the fracture, increasing the risk of infection.
Causes of Ankle Fractures
Many types of injuries can cause an ankle fracture. They include:
- Twisting, rotating, or rolling your ankle while walking or running
- Tripping or falling from a height, such as a fall from a ladder
- Impact during an accident, such as a motor vehicle collision
Symptoms of an Ankle Fracture
Common symptoms of a broken ankle include:
- Immediate and severe pain
- Swelling
- Bruising
- Tenderness to touch
- Inability to put any weight on the injured foot
- Deformity, especially if the ankle joint is also dislocated
- Numbness and coolness in the foot (in some cases)
Doctor Examination
Physical Examination
After discussing your medical history and how the injury occurred, your doctor will do a careful examination of your ankle, lower leg, and foot.
Imaging Tests
If your doctor suspects an ankle fracture, they will order X-rays to diagnose and evaluate the fracture
X-rays. Most ankle fractures can be diagnosed with X-rays, which provide images of bone. They can show where the bones are broken and if any of the bones are out of place (displaced). They can also show how many pieces of broken bone there are. Your doctor may also take X-rays of your leg and foot to make sure there are no other injuries.
Depending on the type of ankle fracture, your doctor may put pressure on the ankle and take a special X-ray called a stress X-ray. A stress X-ray is an X-ray taken while you are standing on the ankle. This X-ray will help the doctor see whether you have a stable fracture that does not require surgery or a fracture that is more unstable and therefore requires surgery.
Computed tomography (CT) scan. A CT scan provides detailed cross-sectional X-ray images of the ankle and is sometimes done to further evaluate the ankle injury. It is helpful for evaluating the extent of the injury to the ankle joint and for planning surgery if surgery is needed.
Magnetic resonance imaging (MRI) scan. MRI scans are rarely needed for ankle fractures. Because MRI scans can show soft tissues better than other imaging tests, they may be used to see if there are any ligament injuries.
Treatment for Ankle Fractures
Treatment of ankle fractures depends on the type and severity of the injury.
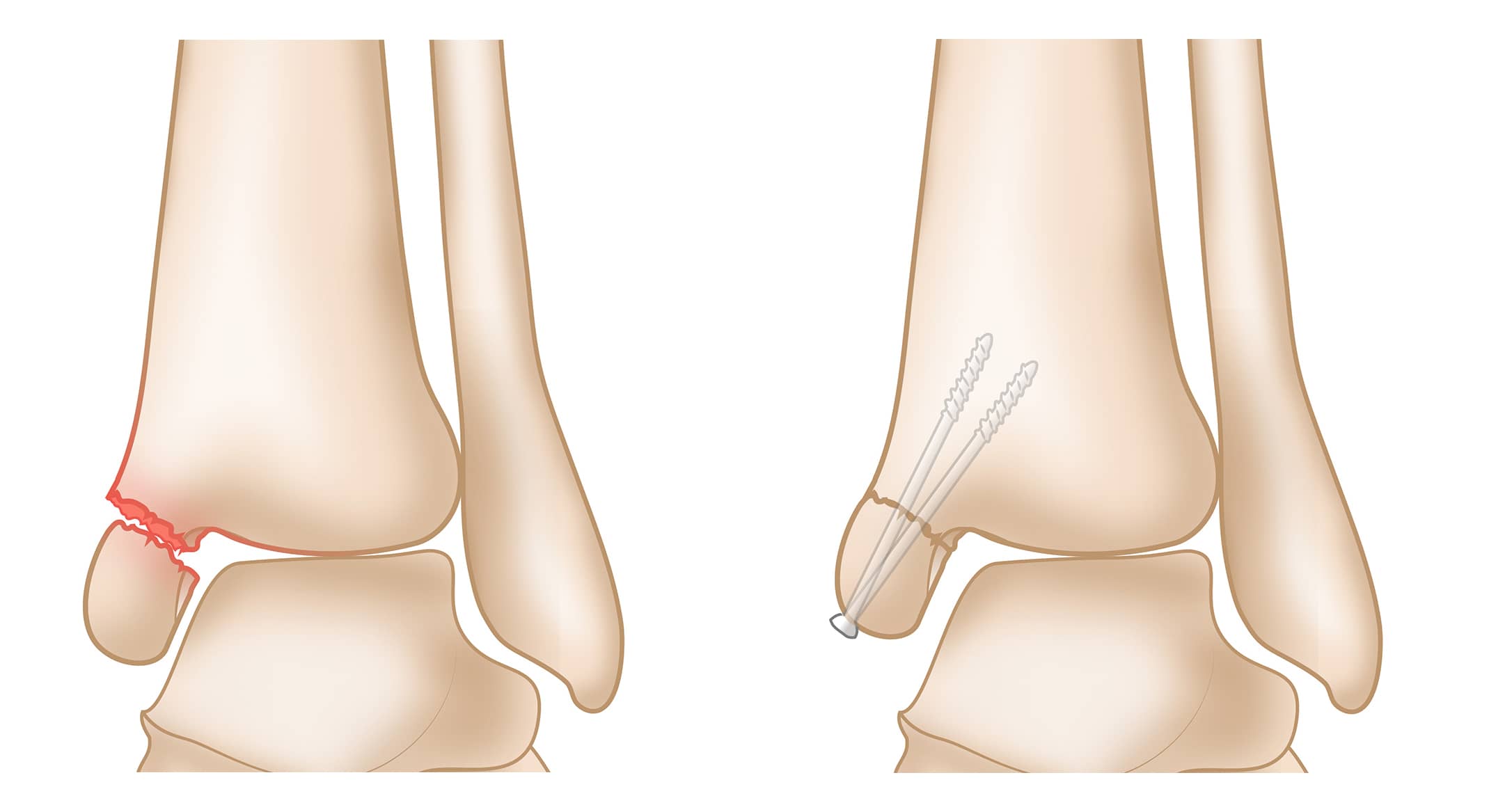
Medial Malleolus Fracture
A medial malleolus fracture is a fracture of the lowest part of the tibia. Although they may occur on their own, fractures of the medial malleolus most often occur together with fractures in other parts of the ankle.
Nonsurgical Treatment
A medial malleolus fracture that is not out of place (nondisplaced) can be treated with a short leg cast or walking boot. Your doctor may or may not recommend that you avoid putting weight on your ankle for several weeks. During this time, the doctor will take X-rays to make sure that the fracture is healing properly.
Surgical Treatment
A medial malleolus fracture that is out of place (displaced) can be surgically repaired with one or two screws. If the fracture is large and extends into the ankle joint, a plate and screws may be required.
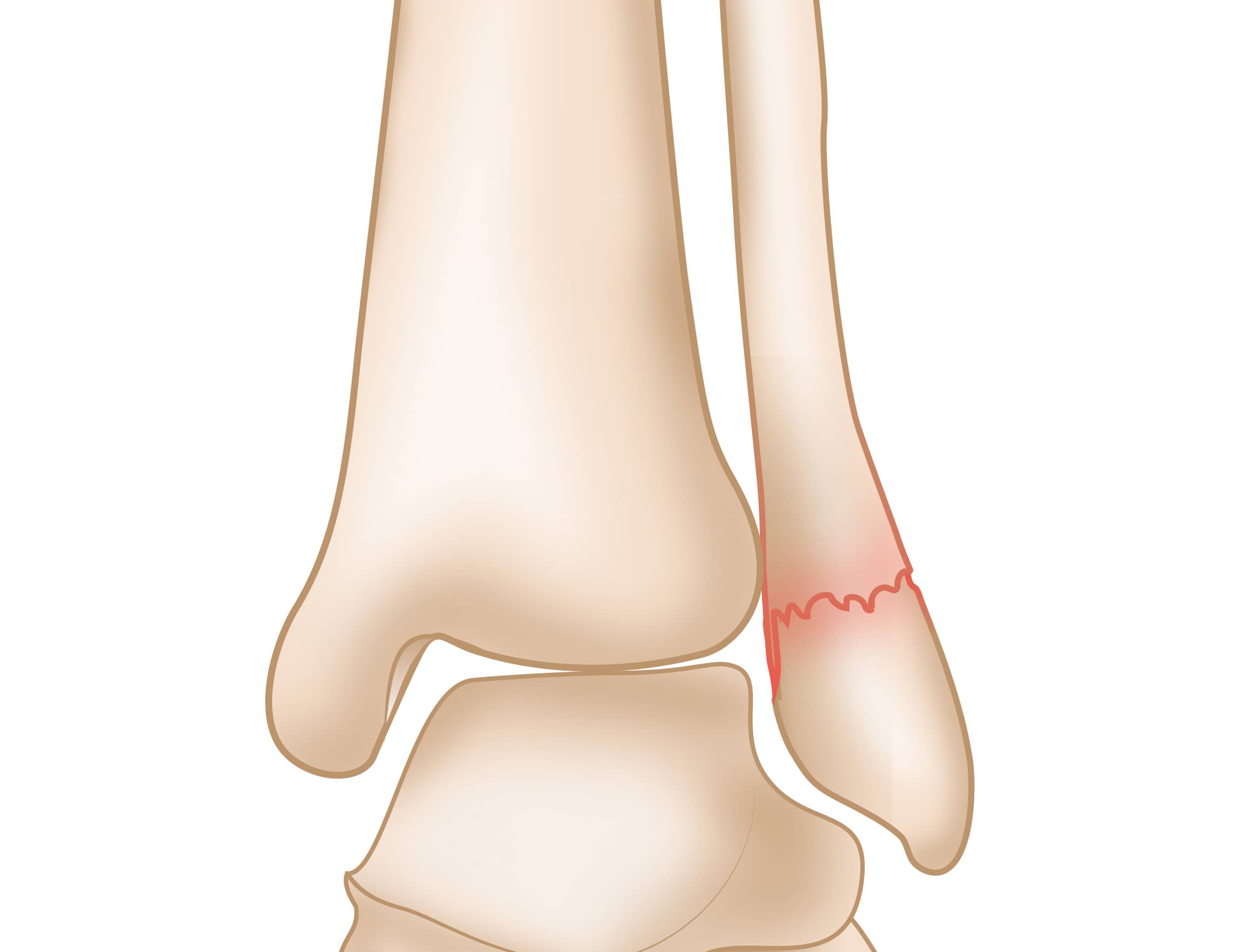
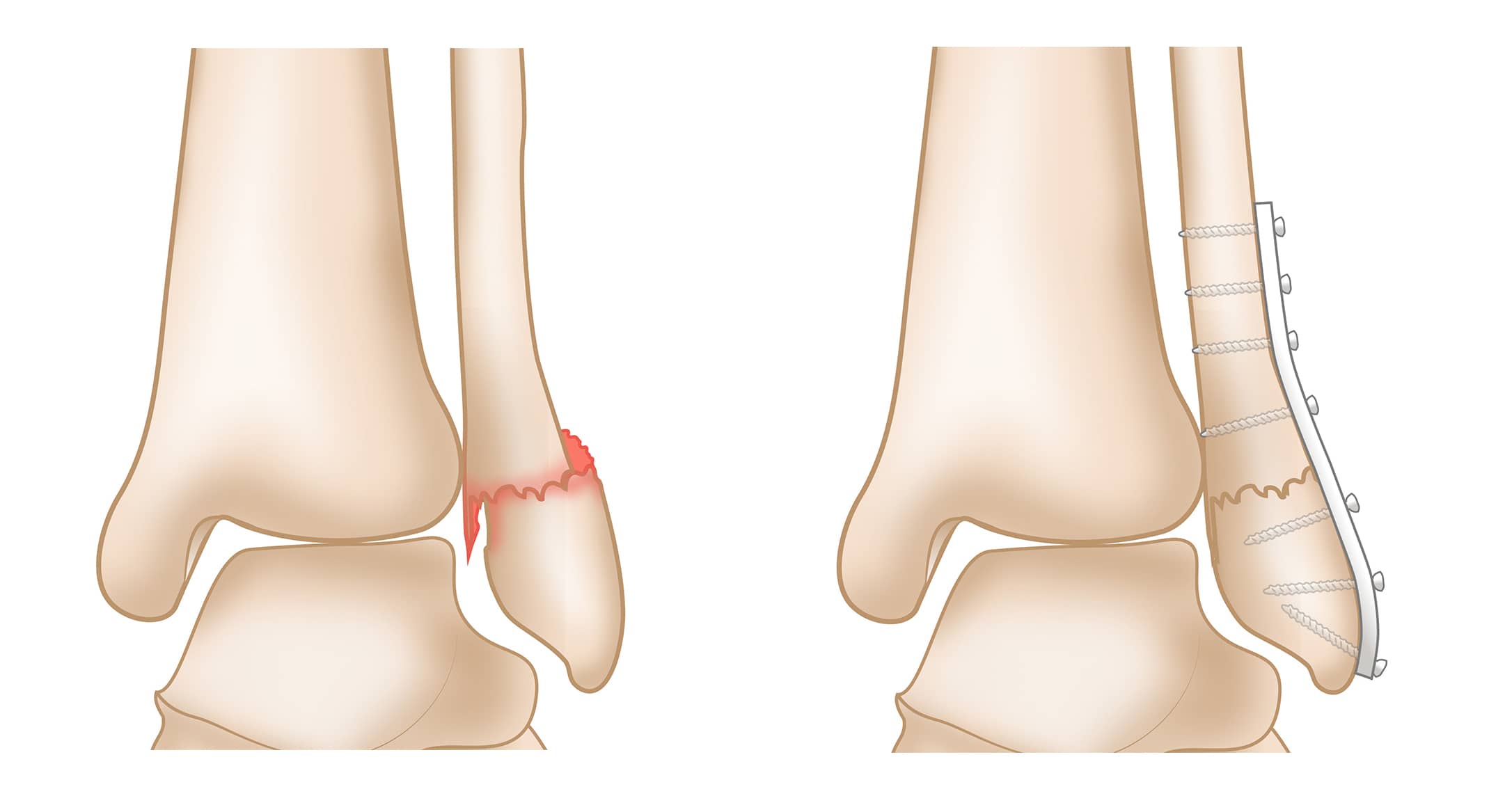
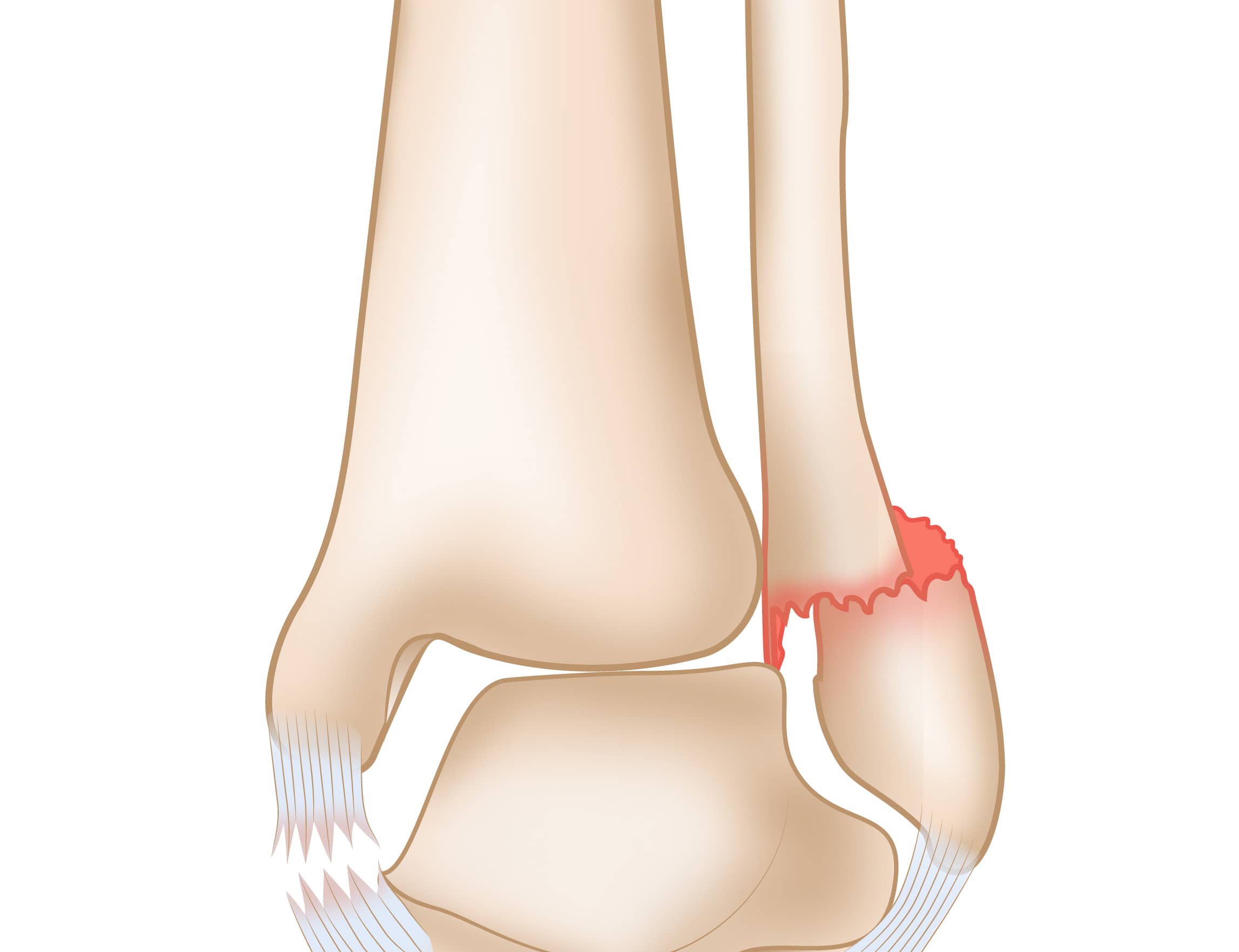
Lateral Malleolus Fracture
A lateral malleolus fracture is a fracture of the lower end of the fibula.
Nonsurgical Treatment
Like a nondisplaced medial malleolus fracture, a nondisplaced lateral malleolus fracture can often be treated with a short leg cast or walking boot. Many isolated lateral malleolus fractures are stable enough to allow you to put weight on the ankle.
Surgical Treatment
Surgical repair is needed on certain types of lateral malleolus fractures that make the ankle joint unstable. The repair is sometimes done with a plate and screws, or a long rod/nail or screw. Sometimes after surgery, your doctor will tell you not to put weight on the leg. This depends on your fracture type and the quality of the bone.
Posterior Malleolus Fracture
A posterior malleolus fracture is a fracture of the back of the tibia. Most posterior malleolus fractures are associated with another injury, usually a fracture of the lateral malleolus. This is due to attachments of ligaments between the two bones.
Nonsurgical Treatment
Many posterior malleolus fractures are small and do not require surgery. Treatment may involve wearing a short leg cast or a removable brace. These types of injuries often occur when other parts of the ankle are broken. Although these other parts may need to be fixed, sometimes the posterior malleolus fracture may not need to be fixed.
Surgical Treatment
Surgical fixation is required if the fracture is large and out of place. This can be done:
- With screws alone, from either the front to the back or the back to the front of the tibia
- With a plate and screws placed directly on the back of the displaced bone fragment
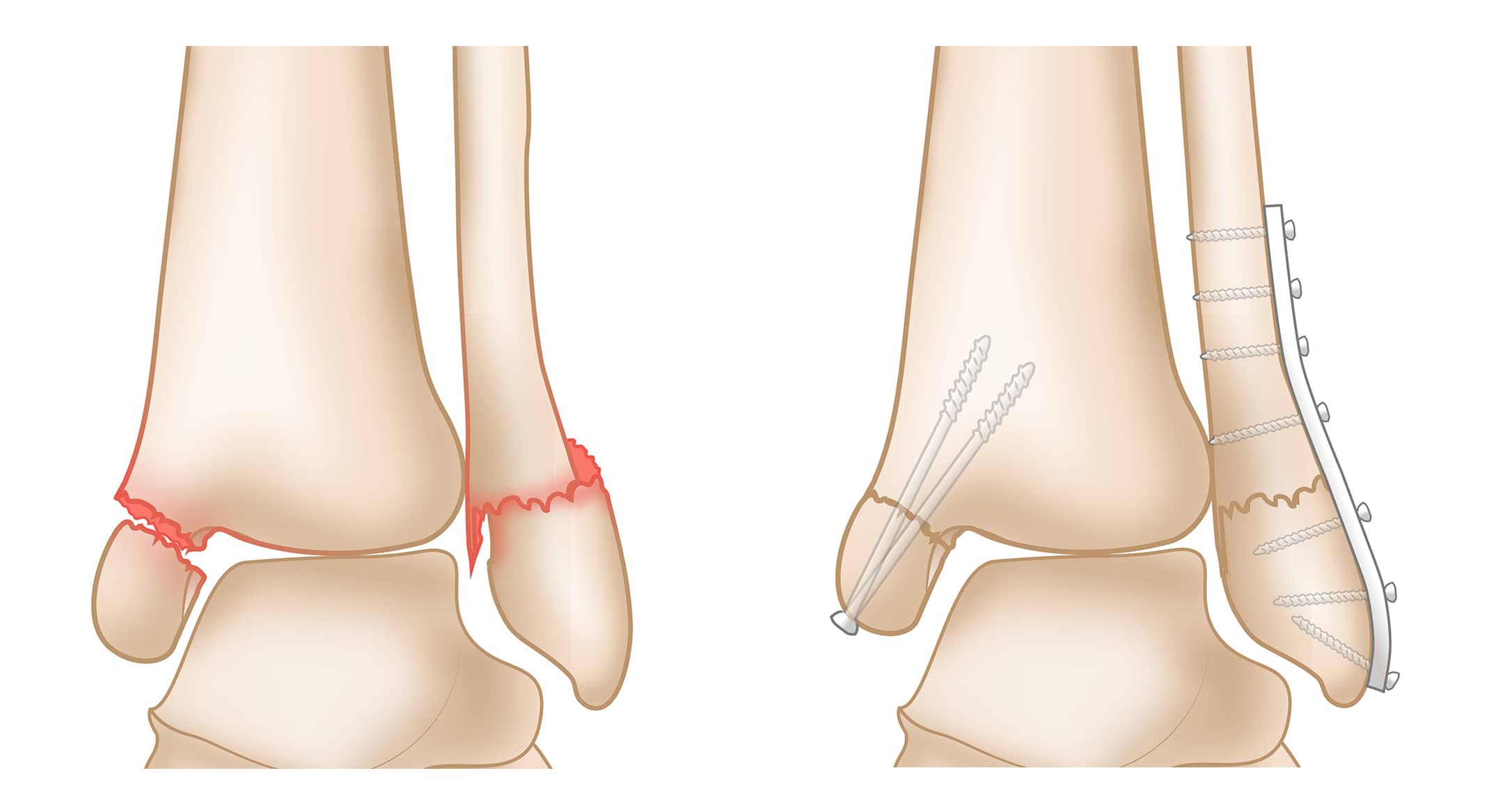
Bimalleolar Fracture and Bimalleolar Equivalent Fracture
A bimalleolar fracture occurs when both the medial malleolus and lateral malleolus are broken. Since there are injuries to both sides of the ankle, bimalleolar fractures are often unstable, and the ankle is often dislocated.
Nonsurgical Treatment
A stable bimalleolar fracture may be treated with cast immobilization for several weeks. During this time, you cannot put weight on your ankle. While you are in the cast, your doctor will take X-rays to make sure that the bones do not slip out of place.
Surgical Treatment
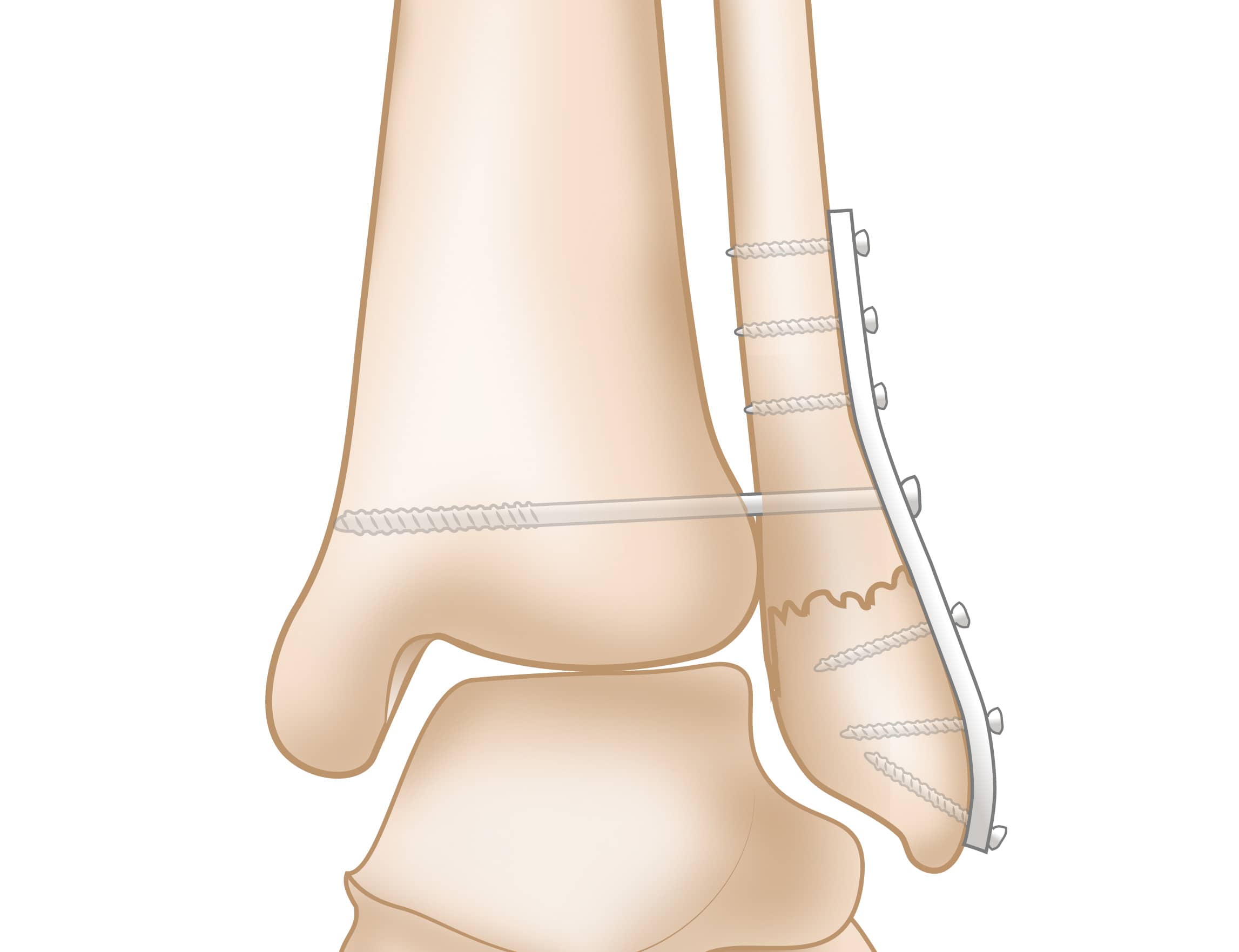
Because there are injuries to both sides of the ankle, most bimalleolar fractures need surgery. This is usually done with a plate and screws or a nail.
Sometimes, only the fibula needs fixation and the medial malleolus fracture does not need to be separately fixed. Other times, both will need to be fixed.
A bimalleolar equivalent fracture means that the ligaments on the inside (medial) part of the ankle are injured, and that only one bone has broken. The torn ligaments can cause the lower bone (talus) to shift and the ankle joint to go partially out of place or dislocate. Treatment involves putting the joint back in place and repairing the broken bone.
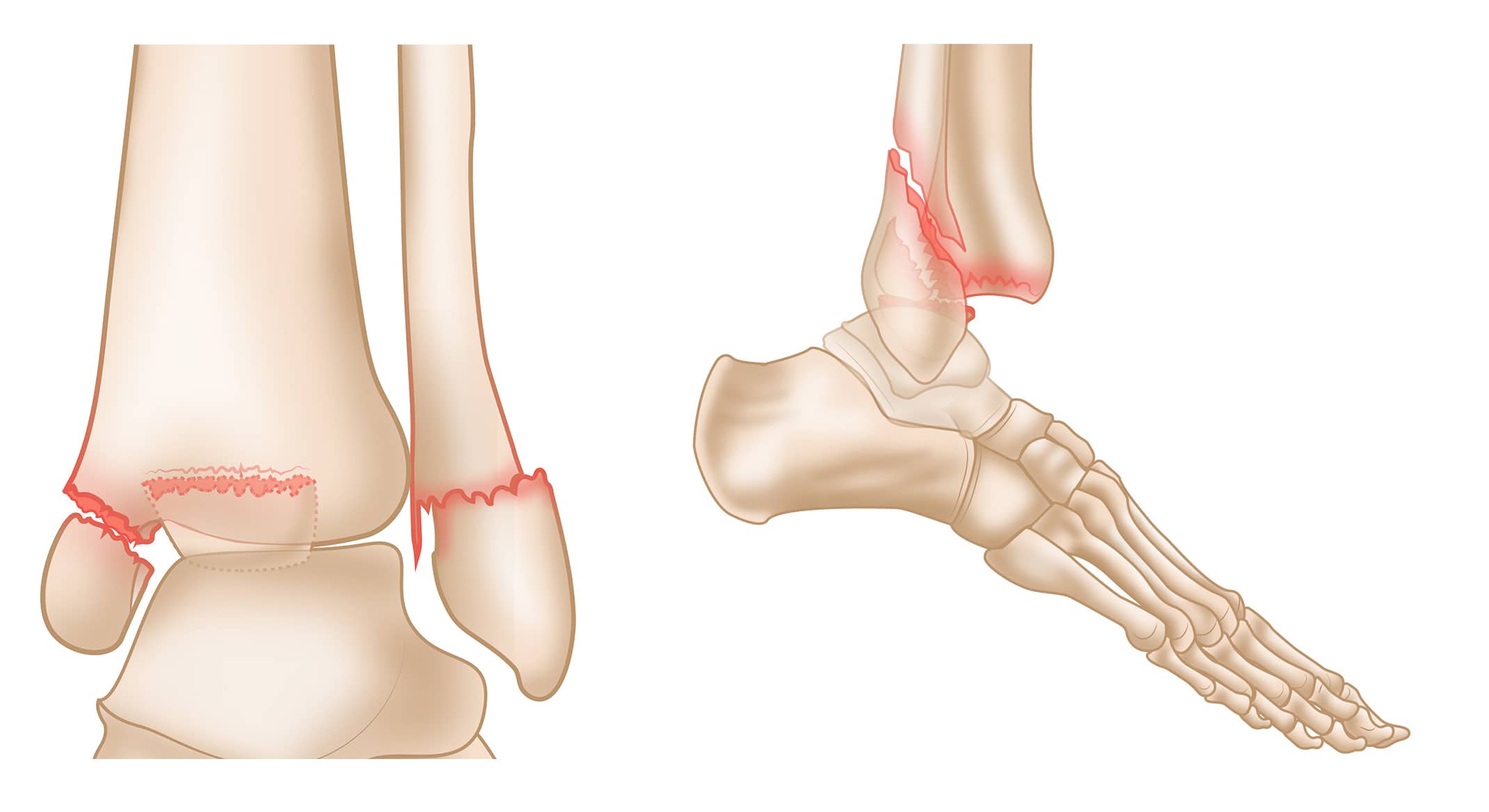
Trimalleolar Fracture
A trimalleolar fracture is similar to a bimalleolar injury except the posterior malleolus is also broken. Like bimalleolar fractures, these injuries are often unstable, and a dislocation can occur.
Most of the time, if the medial malleolus and lateral malleolus fractures are repaired, the posterior fragment will go back into place on its own. If the posterior fragment is out of place and large, you may need surgery.
Syndesmosis Injury
The syndesmosis is a group of ligaments that stabilizes the small joint between the lower end of the fibula and the lower end of the tibia.
A syndesmosis injury that involves only the ligaments is often called a high ankle sprain. It can be usually treated without surgery but may take longer than a normal ankle sprain to heal.
A syndesmosis injury can also involve both a ligament sprain and one or more fractures. In these cases, surgery is required. In addition to repairing the fracture(s), the syndesmosis is repaired with one or more screws or a suture button construct. The screws may or may not be removed after the injury heals.
Recovery From Ankle Fractures
The healing time for ankle fractures depends on the extent of the injury. Most ankle fractures take at least 6 weeks for early healing and 10 to 12 weeks for complete healing. However, it may take longer for any damaged ligaments and tendons to heal.
Regardless of the type of treatment you receive, your doctor will most likely monitor the bone healing with repeated X-rays. This is typically done at 2 weeks, 6 weeks, and 12 weeks but may depend on your specific circumstances.
Pain Management
After surgery, you will likely feel pain because this is a natural part of the healing process. Your doctor will work to reduce your pain. Typically, you will be given pain medicine intravenously (through an IV) in the first few hours after surgery. You will then be switched to oral pain medication. If you have not had surgery, you will be taking oral medication from the start.
Many types of oral medicines are available to help manage pain, including opioids, non-steroidal anti-inflammatory drugs (NSAIDs), and over-the-counter pain medication such as acetaminophen. Your doctor may use a combination of these medications to manage your pain, as well as minimize the need for opioids.
Be aware that although opioids help relieve pain after surgery or an injury, their use has risks and complications. These medications can be addictive and potentially dangerous. It is therefore important to use opioids only as directed by your doctor, to use as little as possible for as short a time as possible, and to stop taking them as soon as your pain starts to improve.
Rehabilitation
Rehabilitation is the key to your recovery, no matter which type of treatment you have.
Rehabilitation usually begins after your fractures have started to heal and your cast or walking boot has been removed. Your doctor will let you know when you can start putting weight on your ankle. They may also refer you to a physical therapist to start an exercise program.
It is very important to follow your doctor's instructions about weightbearing. If you put weight on the injured ankle too early, the fracture fragments may move out of place, and the fracture may not heal (nonunion) or may not heal correctly (malunion).
Your doctor may also recommend that you wear an ankle brace for sports for several months after your fracture has healed.
Complications After an Ankle Fracture
Many patients will experience stiffness and swelling in the injured ankle for many months, even after the fracture has healed.
Rehabilitation will help improve the motion in your ankle and prevent stiffness. The swelling can be relieved by elevating your leg.
Other general complications include malunion, where the bones do not heal properly, or nonunion, where the bones do not heal at all.
Some complications are specific to ankle fracture surgery. These include:
- Infection
- Bleeding
- Damage to blood vessels, tendons, and nerves
- Problems with the plates or screws used to repair your ankle
- Arthritis, which can develop years after the injury
People who smoke, have diabetes, or are elderly have a higher risk of complications after surgery.
Outcomes for Ankle Fractures
Most people return to normal activities within 3 to 4 months after the injury occurs.
If your right ankle is affected, you can probably resume driving at 9 to 12 weeks. You may still be limping after several months, and it may take longer to return to sports.
Complete recovery from some ankle fractures may take up to 2 years.
Contributed and/or Updated by
Peer-Reviewed by
AAOS does not endorse any treatments, procedures, products, or physicians referenced herein. This information is provided as an educational service and is not intended to serve as medical advice. Anyone seeking specific orthopaedic advice or assistance should consult his or her orthopaedic surgeon, or locate one in your area through the AAOS Find an Orthopaedist program on this website.